Using private health insurance
4.1
This chapter will consider the use of private health insurance in a
range of different settings, including in public hospitals, out-of-hospital
care and in dentistry.
Public hospitals
4.2
A number of submitters to the inquiry were concerned that current
arrangements allow policy holders to be treated as private patients in a public
hospital.[1]
4.3
The National Health Reform Agreement (Reform Agreement) allows a patient
to elect to be treated as a private patient in a public hospital.[2]
4.4
The Independent Hospital Pricing Authority (IHPA), one of the bodies
created by the Reform Agreement, commissioned professional services firm Ernst
and Young (EY) to write a report on the utilisation of private patients in
public hospitals.[3]
The IHPA provided the committee with a copy of the EY report that noted that
more people are choosing to be treated as private patients in public hospitals.[4]
The rate of increase has varied across Australia as the below table shows.
Table 4.1 - Proportion of public hospital separations funded
by private health insurance by State and Territory 2008-09 to 2014-15
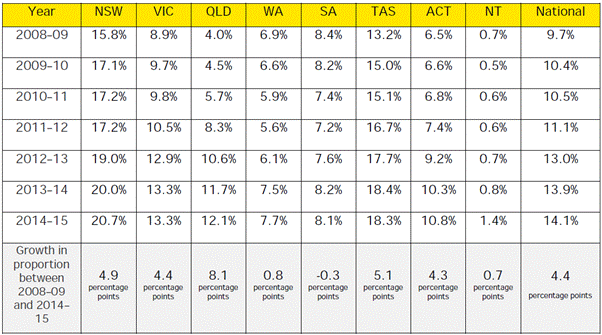
Source: IHPA, Submission 2,
p. 10.
4.5
The EY report investigated whether a change in the hospital funding
model—from block funding to Activity Based Funding (ABF)—was driving the
increase in the number of patients electing to be treated privately.[5]
The report concluded that ABF was not a significant driver of the increase, but
that intentional policy settings adopted by state governments are attracting
larger numbers of private patients.[6]
4.6
IHPA told the committee that the Commonwealth provides ABF to the states
in accordance with the Reform Agreement.[7]
However, public hospitals may have a financial incentive to attract private
patients depending on whether the funding model adopted by the state or territory
accounts for the revenue generated by private patients:
...funding provided to State and Territory governments per
National Weighted Activity Unit (NWAU) is discounted for private patients
through the implementation of a Private Patient Adjustment to account for
additional revenue for private patients from Private Health Insurers... and other
Commonwealth sources.
Without making allowances for additional funding for private
patients through private patient adjustments, there would be financial
incentives for State and Territory governments, LHNs [Local Hospital Networks]
and public hospitals to increase the number of patients admitted as private
patients to public hospitals to generate additional funding.[8]
4.7
The below table briefly explains that there is a financial incentive in
some jurisdictions to treat private patients in public hospitals.
Table 4.2—Incentives to attract private patients
| State |
Private patient adjustments |
Incentive |
| NSW |
Local Health Districts
(LHDs) and Specialty Health Networks (SHNs) were set private patient targets.[9]
Where private patient targets are exceeded, the LHD / SHN retained the
associated own source revenue (OSR) and where targets were not met LHDs /
SHNs experienced a decline in funding.[10] |
Yes |
| QLD |
Only 36 QLD public
hospitals were funded using ABF (87 block-funded). There were no private
patient adjustments because the Health and Hospital Service (HHS) contributed
some OSR. When the HHS was above its target for private patients, it retained
the surplus funds. QLD Health advised the IHPA that these funds were used to
mitigate the financial impact of unrecovered revenue.[11] |
Yes |
| TAS |
The Tasmanian ABF model
provided funding to health organisations on a gross basis with revenue
targets.[12]
The Tasmanian model made no adjustment for private patient accommodation or service
adjustments.[13]
Therefore, there was an incentive to recruit more private patients because
there was no deduction to account for the additional revenue received from
private patients.[14] |
Yes |
| VIC |
Victoria used a Weighted
Inlier Equivalent Separation (WIES) funding model.[15]
The WIES model had a 24 per cent discount for private patients.[16]
Across some Diagnosis Related Groups (DRGs) the Victorian model did not
adequately adjust and there may have been an incentive to target private
patients with particular conditions where additional revenue had not been
fully incorporated into the discounted WIES price.[17] |
May be a residual incentive |
| WA |
The WA ABF model did not
apply any private patient adjustments and so the same amount was received
from the state government for public and private patients.[18]
The IHPA model provided a private patient discount to offset the revenue states
and territories received from alternate sources.[19]
However, there may have been an incentive to target private patients if the
provider considered it could obtain additional revenue from the Commonwealth
or the private health insurer.[20] |
May be a residual incentive |
| SA |
SA adopted the National ABF
model for acute care but not sub-acute or non-acute care, including the
private patient accommodation and service adjustments.[21]
The Local Health Networks that provided sub-acute and non-acute care received
the same amount from the state government regardless of whether the patient
was a private or a public patient.[22]
However, they may have had an incentive to target private patients if the
provider considered it could obtain additional revenue from the Commonwealth or
the private health insurer.[23] |
May be a residual incentive |
| ACT |
Hospitals in the ACT
received the same amount regardless of whether the patient was public or
private because it implemented the full ABF model including the adjustments.[24] |
No |
| NT |
There was insufficient
information publicly available to determine whether there were price
differences between public and private patients.[25] |
Unknown |
4.8
The committee received evidence that some hospitals or health services
have hired specific staff, often known as a Private Patient Officer (or
similar), to encourage consumers to be treated as private patients in a public
hospital.[26]
One way hospitals or health services have promoted the use of private health
insurance in a public hospital is to tell patients that using their private
health insurance will assist the hospital.[27]
4.9
The Haemotology Federation of Australia conducted an 'online community
survey' to assist in preparation of its submission to the inquiry.[28] Based on that
survey, Haemotology Federation of Australia advised the committee that:
Although [respondents] were largely required to attend public
hospitals due to their bleeding disorder, some respondents described being
asked to be admitted as a private patient. Many were happy to do this as they felt
it was a contribution to the public health system, and some also preferred this
where it gave them the possibility of a single room and choice of doctor, and
covered telephone and newspapers.[29]
4.10 Some submitters raised concerns that some institutions apply pressure to
policy holders to get them to use their private health insurance.[30]
4.11
The Consumers' Health Forum of Australia told the committee that some
policy holders are being coerced or are being asked to elect whether to use
their private health insurance in circumstances of severe stress. The Consumers'
Health Forum of Australia provided the following example from a patient who
responded to one of its private health insurance surveys:
I had a minor operation at a Private Hospital. Pneumonia from
op... Ended up in casualty at a major hospital for 14 hours on a trolley as
there was no bed. Serious pain, no relief. A bed became available and I was
asked am I "Private or Public"? No explanation. I said private and I
just got bills as a result.[31]
4.12
Bupa Australia also told the committee that it had received anecdotal
evidence from policy holders that some public hospitals had pressured patients
into using their private health insurance:
Current behaviour by many public hospitals sees many Bupa
members receiving a bedside visit after a procedure or letters two or three
months after an event pressuring them to declare their private cover and we
believe this is unquestionably inappropriate and contrary to the intent of
private patient declaration.[32]
4.13
Accordingly, Bupa Australia recommended to the committee that policy
holders should only be able to elect to use their private health insurance for
pre-booked admissions and only if the patient signs a form that is submitted to
the insurer at least 24 hours before admission to hospital.[33]
Waiting times
4.14
The committee received evidence that many people believe they will gain
access to surgery more quickly if they are admitted to a public hospital as a
private patient.[34]
4.15
Choice conducted a survey of 1027 consumers about their reasons for
purchasing private health insurance in April 2017.[35]
The respondents to Choice's survey found that 43 per cent of respondents and 56
per cent of respondents over the age of 56 considered 'avoiding public hospital
waiting lists' as one of the key reasons for purchasing private health
insurance.[36]
4.16
The Consumers' Health Forum of Australia received a similar indication
from consumers:
[Consumers' Health Forum of Australia's] work with consumers
has found that one of the main reasons they value having PHI [private health
insurance] which they can use in a public hospital is that it allows them to 'jump
the queue' for elective surgery and obtain it in a period they are satisfied
with, instead of the extremely long waiting lists that they perceive come with
relying on the public system.[37]
4.17
The Department of Health (Department) provided the committee with a copy
of Clause 4 of the Reform Agreement which provides:
States will provide health and emergency services through the
public hospital system, based on the following Medicare principles:
- eligible
persons are to be given the choice to receive, free of charge as public
patients, health and emergency services of a kind or kinds that are currently,
or were historically provided by hospitals;
- access
to such services by public patients free of charge is to be on the basis of
clinical need and within a clinically appropriate period; and
- arrangements
are to be in place to ensure equitable access to such services for all eligible
persons, regardless of their geographic location.[38]
4.18
The Department explained to the committee that this means that:
...providing that access to services for public patients is on
the basis of clinical need and within a clinically appropriate period, the NHRA
[National Health Reform Agreement] does not prevent public hospitals from
treating private patients before public patients.[39]
4.19
Mr Charles Maskell-Knight, the Department's Principal Adviser,
Health Systems Policy Division, was more explicit, suggesting hospitals may
positively discriminate in favour of privately insured patients:
Mr Maskell-Knight: There's a misconception that the
Medicare principles require access to services within public hospitals to be
based on clinical need, and that was the case from 1984 until 1998. In 1998 the
then state and healthcare agreements were changed and the relevant principle
was that public patients should receive care on the basis of clinical need
within clinically appropriate periods.
Senator DI NATALE: What does that mean for private
patients?
Mr Maskell-Knight: That hospitals may differentiate in
favour of them.[40]
4.20
Earlier this year the Australian Institute of Health and Welfare (AIHW)
released its Admitted patient care 2015–16: Australian hospital statistics
report.[41]
One of the key findings from that report related to the difference in the
median waiting times between public and private patients:
Overall, Public patients had a median waiting time of 42
days, compared with 20 days for hospitalisations with a funding source of
Private health insurance.[42]
4.21
Some submitters were very concerned by the prospect that privately
insured patients may be receiving preferential treatment on the basis of their
insurance status.[43]
4.22
The AIHW noted that there may be some legitimate reasons for differences
in the timeframes for private and public patients:
...there may be differences between public patients and
patients funded by other sources, in the conditions treated and in the urgency
categories assigned, that may account for some variation in waiting times.[44]
4.23
The Australian Health and Hospitals Association (AHHA) noted that the
AIHW data did not take account of acuity or case mix, both of which would
impact on waiting times.[45]
In relation to the AIHW data, the Queensland Government told the committee
that:
It is important to note that published results do not
separate the different urgency categories patients are placed into, which
consist of different clinically recommended treatment times (treatment within
30, 90 and 365 days for Category 1, 2 and 3, respectively).[46]
4.24
Consumers' Health Forum of Australia agreed that the AIHW data may
require further investigation:
...the data from which these conclusions are drawn are not
necessarily robust and there may be clinical reasons for this apparent trend.
There needs to be a recommitment by all stakeholders to the principle of
treatment in the public system being based on clinical need. This should be
supported by enhanced monitoring and data collection to allow for more
investigation before major policy decisions are made in this area.[47]
4.25
In December 2017, the AIHW released a more comprehensive report—Private
health insurance patients in Australian hospitals, 2006–07 to 2015–16—to
address the issues identified in the Admitted patient care 2015–16:
Australian hospital statistics report.[48]
The AIHW Private health insurance patients in Australian hospitals, 2006–07
to 2015–16 report identified that:
Private health insurance patients were more likely to be
assigned to clinical urgency category 1 (admission within 30 days) compared
with public patients and other patients (39%, 27% and 23%, respectively).
Among surgical specialties, the largest differences in the
proportion assigned to clinical urgency category 1 were for Neurosurgery (50%
for private health insurance patients, 30% for public patients, and 32% for other
patients).[49]
4.26
As an example, the AIHW examined data for total knee reconstructions.
The data revealed that patients with private health insurance had shorter
median waiting times than public patients:
For Total knee replacement, 50% of private health insurance
patients were admitted within 76 days for their surgery, compared with 203 days
for public patients and 54 days for other patients.[50]
4.27
Whilst some submitters called for an end to policies that would allow
patients to be treated as a private patient in a public hospital, other
submitters warned that ending such policies could have unintended consequences.
The Queensland Government told the committee:
A possible unintentional outcome of restrictions on private
patient practices could be that hospitals might have difficulty attracting and
retaining medical practitioners, leading to increased difficulty meeting
growing health service demand.[51]
Committee view
4.28
The committee is concerned about the trend in the number of people
electing to be treated as private patients in a public hospital. The committee
has concerns that state and territory governments are implementing policies
that encourage hospitals and health networks to attract private patients.
4.29
The committee notes the AIHW findings that confirm that median waiting
times for private patients are shorter than for public patients, but longer
than for 'other' patients.
4.30
The committee was also concerned by the evidence of consumer groups that
some people feel pressured to elect to be treated as a private patient. The
committee maintains that the decision on whether to be treated as a private
patient ought to be made by the patient with full knowledge of the financial
and associated consequences.
Hospitals and out-of-hospital care
4.31
The committee received evidence that current regulation prevents private
health insurers from being able to constructively engage with insured consumers
to manage their risks.[52]
4.32
Private Healthcare Australia told the committee that:
Legislation currently prevents private health insurance from
covering medical services that are provided out-of-hospital and covered by
Medicare. This may inhibit insurers from funding up-to date models of care for
chronic conditions which are based out-of-hospital, and out-of-hospital care
which may help to avoid unnecessary hospitalisations. In some cases,
out-of-hospital care is preferable to treatment within a hospital for clinical
reasons. By preventing insurers from funding out-of-hospital care in these
cases (which is often more cost effective than in-hospital treatment), the
legislation is putting upwards pressure on premiums.[53]
4.33
Private Healthcare Australia also told the committee that as a result of
these legislative restrictions people may be unnecessarily hospitalised:
It also creates an obvious perverse incentive for doctors to
admit patients to hospital, particularly for short-stay admissions when it isn't
clinically required. This is because in doing so, the provider can claim gap
cover, and additional revenue if they have an additional financial stake in a
short-stay hospital facility. This has fuelled huge growth in hospitalisation
of patients previously treated in doctors' rooms and in the community, for
everything from excision biopsies to cognitive behavioural therapy, and has
inevitably put upward pressure on premiums. It would make much more sense to
amend the legislation, permitted [sic] health funds to negotiate with providers
for appropriate remuneration in an appropriate setting of care.[54]
4.34
As noted in Chapter 2, the Royal Australian College of General
Practitioners (RACGP) have also acknowledged that private health insurers may
have a role to play in helping to keep Australians healthy:
PHI [private health insurance] organisations can improve the
health of their members and Australians more widely through supporting services
not funded through Medicare such as:
-
chronic disease management –
providing additional services for patients with complex and chronic disease
-
care coordination and team care –
supporting patients to access nurse services, additional allied health visits
and programs to assist patients transitioning between primary and tertiary
healthcare, including preadmission or post-operative care
-
general practice modernisation –
supporting patients to access telehealth consultations and services with their
regular GP [general practitioner]; supporting the use of newer technologies...[55]
4.35
The private health insurance industry has indicated that this is an area
that it would like to move into. Private Healthcare Australia told the committee:
Out-of-hospital, we can't contribute. The costs of people
treating their cancer out-of-hospital, we can't contribute. Mental health
treatment out-of-hospital...the current regulatory system means we cannot easily
contribute to patient out-of-hospital costs in the situations where that would
avoid hospitalisation. That is something in the modern world we think needs to
change. It's also currently acting as a perverse incentive encouraging
unnecessary admissions to hospital in some key treatment areas.[56]
4.36
The AHHA suggested that private health insurers ought to be able to
contribute to out-of-hospital care in certain circumstances:
The AHHA recommends that where medical services are provided
on referral from the hospital in an outpatient, community or home setting, that
these services be eligible for cover through private health insurance.[57]
4.37
NIB also suggested that extending the Broader Health Cover provisions
may help to attract more young people and keep premiums low.[58]
4.38
The Department, however, told the committee that private health insurers
have been able to provide some of these services since April 2007.[59]
The Department indicated that private health insurers could already offer
Chronic Disease Management Programs and hospital-substitute treatment,
including chemotherapy or a dialysis in a patient's own home or a community
clinic.[60]
4.39
The Grattan Institute was supportive of providing private health
insurers some greater latitude to determine what products they offer:
The most recent Australian study I've seen suggests that
home-based rehab is just as useful as in-patient rehab. We need to give the
private health insurance funds more ability to manage what they are paying for.
At the moment they are highly constrained by regulation. If there's going to be
more transparency, and more demands made on them, they ought to have a right to
more flexibility in what they do.[61]
4.40
However, the RACGP considered that the committee should be cautious in
extending the reach of private health insurers into primary care.[62]
The RACGP warned that some of the risks may include the duplication and
fragmentation of care—potentially involving 'preferred GP [general
practitioner] providers'—removal of general practitioners' clinical
independence or access on the basis of insured status.[63]
Case study: dentistry
4.41
The committee received a significant number of submissions from dental
practitioners, or individuals who work in the dental industry, about the effect
that private health insurance has had on private dentistry.[64]
The committee received some similar submissions from optometrists and
physiotherapists.[65]
The committee considers that dentistry provides a useful a case study through
which to examine the role of private health insurance in the provision of
primary health care.
Contracted dentists
4.42
The committee heard that some dentists have entered into contracts with
private health insurers to charge agreed fees to the private health insurer's
policy holders.[66]
In return, the private health insurer markets the dental practice and provides
better rebates to the private health insurer's policy holders when they visit
that clinic.[67]
Private health insurers often refer to these contracted dentists as 'preferred
providers' or 'member's choice' providers.[68]
4.43
The most common concern raised by dental practitioners was that private
health insurers provided different rebates to insured consumers based on whether
their dentist had a contract with the consumer's private health insurer.[69]
4.44
Dental practitioners submitted that it was unfair to consumers who had
paid for extras policies to receive lower rebates because they decided to use
their private health insurance to visit a non-contracted dentist.[70]
These submitters argued that consumers who purchase the same extras policy from
the same insurer ought to receive the same rebate regardless of which dentist
the consumer decides to visit.[71]
4.45
The Australian Dental Association (ADA) told the committee that in some
cases, the rebates private health insurers paid to consumers that visited
non-contracted dentists were so low that dentists who charged substantially
lower rates struggled to compete against contracted providers:
You will see from these examples that the issue is not with
the fee charged, but rather the rebate paid. In the first two scenarios the fee
for the porcelain crown is less at an independent, non-contracted dentist.
However, the rebate provided by the fund is significantly higher when the
patient is treated by a contracted dentist. This results in a substantial
difference in the patient's out-of-pockets cost, which has little or nothing to
do with the fee charged by the dentist.[72]
4.46
The ADA and many dental practitioner submitters considered that
consumers would be better empowered to make decisions about where to use their
private health insurance if insurers were required to pay the same rebate to
insured consumers regardless of which dentist they visited.[73]
Accordingly, the ADA and the dental practitioners called for an end to the
practice of applying differential rebates depending on whether the dentist was
contracted or not.[74]
4.47
In response to a question on notice, Bupa Australia disputed the
suggestion that a consumer who visited a cheaper dentist could end up with
larger out-of-pocket costs because of the rebate provided by the private health
insurer.[75]
However, the ADA provided the committee with further documents to substantiate
its claim.[76]
4.48
Submitters advised the committee that clients who called their private
health insurer have often been provided with incorrect information. One concern
was that clients were sometimes told that the reason they received a low rebate
was because the dentist 'charged too much'.[77]
4.49
Specialist dentists, such as orthodontists and endontists, told the
committee that private health insurers were providing advice to insured
consumers that, instead of going to see the dental specialists recommended by
their dentist, they should visit a 'preferred provider' dentist.[78]
4.50
One endontist told the committee:
...most of my patients are seeking relief from pain or
discomfort caused by either trauma or infection. They are seeking that
treatment through a registered specialist because they have been referred by
their general dental practitioner to achieve the best possible outcome for
their long-term health. Most have complex management needs. However, my
patients report at least weekly that they are disappointed and frustrated by
the fact that, on inquiry about rebates, health funds actively endeavour to
redirect them to health fund preferred providers, or health fund clinics, where
no specialist care is available. The justification for this is that the
preferred providers or health fund clinics provide better rebates (despite the
fact it is not specialist care).[79]
4.51
Many other specialists expressed similar views and considered the advice
of the private health insurer's staff to be clinical in nature and therefore
inappropriate.[80]
4.52
Another concern that dental practitioners raised with the committee was
that new dentists are unable to join the 'preferred provider' schemes.[81]
The inability to become a preferred provider meant that they were unable to
ensure that their clients received higher rebates. In some cases, this meant
that independent dentists lost clients who were under financial pressure.[82]
Anti-competitive practices
4.53
The dental practitioner submitters to the inquiry considered that the
'preferred provider' schemes, and a number of other practices engaged in by the
private health insurers, are anti-competitive.[83]
4.54
One of the concerns that the dental practitioners raised was that
private health insurers have started a process of vertical integration where
private health insurers now own some contracted dental clinics.[84]
4.55
Many dental practitioners considered that owning clinics was a conflict
of interest because the private health insurer, with whom they were now in
competition, was able to unilaterally determine the rebate that insured
consumers would get if they visited a non-contracted dentist.[85]
4.56
In addition, submitters told the committee that private health insurers
were actively steering or redirecting policy holders toward contracted dentists
where they could obtain a better rebate.[86]
This steering could take the form of a letter or phone call to a client
after a visit to an independent dentist advising them that they should visit a
'preferred provider'.[87]
4.57
Bupa Australia rejected the suggestion that it redirected insured
consumers from independent dentists to contracted dentists:
There are a lot of things said about us 'directing' people—we
don't. We promote that there is a range of benefits people can access via their
products. Every consumer has the same choice in their product.[88]
4.58
Dental industry submitters were also concerned that the private health
insurers could compete against them with full knowledge of what practitioners'
fees are and what rebates patients are receiving. Private health insurers
obtain this information through a billing system called the Health Industry
Claims and Payment Service (HICAPS).[89]
4.59
Dental practitioners told the committee that through HICAPS:
The PHI's [sic] have access to all of the information
processed by the HICAPS machine in every dental surgery. This means that they
can monitor a dentists [sic] fees, the type of work, client base size and
composition, and obviously if any of their own customers are patients to that
dentist. This puts the dentist at an extreme disadvantage.[90]
4.60
Since 1999 the Australian Competition and Consumer Commission (ACCC) has
produced 18 reports for the Senate about the anti-competitive practices of
private health insurers.[91]
The ACCC has been asked to consider if 'preferred provider' schemes are
anti-competitive on a number of occasions.[92]
Management of services
4.61
Both 'preferred provider' dental practitioners and independent
practitioners raised concerns in relation to attempts by private health
insurers to influence the treatment of patients by refusing to pay for
particular item combinations to be charged together or by imposing restrictions
on benefits.[93]
4.62
One submitter explained to the committee:
For example, you are not allowed to have a comprehensive
dental examination and a dental crown on the same day...I once had a patient
present with a broken tooth so I undertook a comprehensive examination and
performed a crown for the tooth on the same day to fix the problem. But the
patient received no rebate for the crown. The patient obviously was very upset.
The patient left to discuss it with the PHI [private health insurer's] office,
and so I received a call by the PHI representative. I was told that to do a
crown on the same day as the comprehensive exam was not a reasonable treatment
and violated their rules... So I was told that perhaps I should not charge the
patient for the dental examination. That way the patient can receive the full
rebate for the crown. They were asking me to remove a legitimate code and were
trying to manipulate my clinical operations by suggesting that my treatment was
not reasonable! That is not their decision to make as the insurer.[94]
4.63
Another submitter explained that they had a similar experience with
private health insurers placing restrictions on performing clinically necessary
dental work:
Some health funds restrict or do not pay on item numbers
related to crowns (611, 613, 615 or 618) when an item of removing a crown has
been performed on the same day (655). It is common practice that if a crown
needs replacement due to decay or breakages, then the crown is removed, the
tooth repaired and a crown commenced for a new crown on the same day to avoid
further harm and exposure of the tooth. Patients I have treated have been left
paying higher out of pocket costs and financially worse off than expected
because the health fund has not been clear in their rebates on these items when
associated with other items.[95]
4.64
The dental practitioners explained that they used to be able to
accurately predict patients out-of-pocket costs because private health insurers
used to publish guides to their rebates:
Many years ago, the Health Funds used to publish their
rebates in a booklet. This was of benefit to their customers and to their
Dentists because we were able to let our patients know how much they might
receive as a rebate from their Health Fund and what the gap payment may be. The
Health Funds stopped publishing these rebate booklets because we were able to
show our patients (ie their customers) that the rebates had not increased, or
increased only slightly, over the years and also we were able to show
comparisons of rebate amounts between various Health Funds. The Health Funds
claimed that they stopped publishing their rebates because they were "commercial
in confidence". The current situation is that when we present a treatment
plan to our patients, we give them our fees as well as the item numbers
involved so that they can contact their PHI [private health insurer] to see how
much they may get back as a rebate. In some cases, when the patient has
contacted their PHI to make this enquiry, they have been told that our fees are
high, or in some cases, that the patient would receive more rebate if they went
to one of the PHI's "preferred providers".[96]
Hospital contracting in paediatric dentistry
4.65
The committee heard evidence that some forms of surgery are financially
unviable for private hospitals because private health insurers provide them
with very low rebates.[97]
4.66
The committee heard evidence from paediatric dentists that they have
been excluded from private hospitals and day surgeries because the hospitals
receive low rebates from private health insurers:
The rebate provided by private health insurers to private
hospitals for in-hospital paediatric dental surgery is so low it is not
financially viable for private hospitals to accommodate paediatric dentistry in
their facilities. As a result, patient access to care is becoming increasingly
restricted due to hospitals and other facilities excluding paediatric dentistry.[98]
4.67
The Australian Association of Paediatric Dentists (AAPD) noted that the
unwillingness of the private health insurers to negotiate contracts meant that
facilities that accommodate paediatric dentists are forced to rely on second
tier default benefits.[99]
Second tier default benefits are a safety net for small hospitals that do not
have agreements with private health insurers, which is approximately 85 per
cent of the average rate for a particular service.[100]
4.68
The AAPD told the committee that the second tier default benefits were
inadequate:
Given that the full rebate is inadequate, the amount paid
under 2nd Tier benefits is grossly inadequate to cover the cost of
providing the services and the patient must be charged a fee over and above the
2nd Tier rate. This results in reduced access to care and financial
hardship.[101]
4.69
That financial hardship is compounded because the Child Dental Benefits
Schedule prevents children from being eligible to receive benefits if they
received treatment under general anaesthetic.[102]
4.70
The AAPD noted that a survey of its members indicated that fewer
facilities were accommodating paediatric dentists:
...our members have reported; the closure of facilities due to
unsustainability financially, a reduced number of operating sessions,
unreliable ad hoc time only, changes in sessions to accommodate a more
profitable surgeon, time restraints on cases and denial of access despite being
accredited for many years at a facility.[103]
4.71
The Australian and New Zealand Society of Paediatric Dentistry also
reported that its members have had operating rights restricted in favour of
surgeons performing more profitable surgeries.[104]
Committee view
4.72
The committee acknowledges that private health insurers may be able to
play a greater role in the management of chronic conditions and out-of-hospital
care. The committee accepts that it is desirable, where possible, to avoid
unnecessary hospitalisation and that providing private health insurers with
some greater latitude to offer these services may be beneficial. However, the
committee is mindful of the concerns raised by the RACGP about duplication and
fragmentation of care.
4.73
The committee acknowledges the concerns of dental practitioners and, in
particular, the financial pressure that can be applied to their businesses by private
health insurers. The committee is concerned by some of the practices raised
above, such as the active redirection of patients and the restriction on the
payment of certain item numbers.
4.74
The committee is also concerned about the exclusion of paediatric
dentists from operating theatres in private hospitals and day surgeries and its
effect on children who are in need of specialist dental services.
4.75
Until the issues raised in this chapter are resolved the committee would
be concerned about the further extension of private health insurance to
out-of-hospital care.
Navigation: Previous Page | Contents | Next Page