Private health insurance premiums
3.1
This chapter considers the economic structures that increase and
constrain private health insurance premiums in Australia.
Factors driving premium increases
3.2
As discussed in the previous chapter, submitters told the committee that
some Australians have been dropping or downgrading their private health
insurance because of affordability or because they perceive that the product is
not value for money.[1]
3.3
However, submitters held differing views about what was causing
significant premium increases.
3.4
Submitters told the committee that increases in underlying cost
pressures are largely to blame for rising premiums.[2]
3.5
The Australian Healthcare Reform Alliance told the committee that
private health insurers were experiencing increased costs in a number of areas,
but questioned insurers' ability to control those costs:
Premiums are rising due to both the growth in consumer demand
for services and increased health technology and pharmaceutical costs. Private insurers
have little or no capacity to influence either of these factors and so have
argued for more control over provider behaviour, in order to reduce inflated
costs and low value care.[3]
3.6
The factors that private health insurers say they cannot control include
utilisation, medical costs, private patients in public hospitals, management
costs and intermediaries.
Utilisation
3.7
Utilisation measures the rate at which insured persons demand hospital
services.[4]
Some submitters considered that increased utilisation had caused premiums to
increase by 50 per cent between 2010 and 2016.[5]
3.8
According to research conducted by the Australian Private Hospitals
Association (APHA), the rate at which consumers accessed services increased by 20 per
cent between 2010 and 2016.[6]
In 2010, the rate was 321 hospital episodes per 1000 insured people.[7]
In 2016, that rate had steadily increased to 384.8 hospital episodes per 1000
insured people.[8]
Table
3.1—Annual ratio of episodes per 1000 persons insured 2010–16
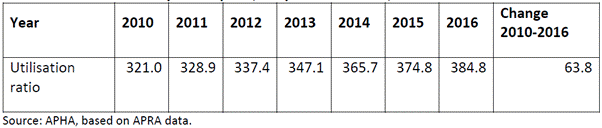
Source: Australian Private
Hospitals Association, Submission 80—Attachment 2, p. 9.
3.9
The APHA told the committee that the 20 per cent increase in the
utilisation rate over this period accounted for 'forty percent [sic] (40.2%) of
the growth in benefits paid out over 2010–2016'.[9]
3.10
Private Healthcare Australia explained to the committee that the
increase in utilisation could be directly attributed to rising consumer
expectations about what the health system ought to deliver:
Consumer expectations of what the health system should deliver
are increasing in line with economic growth and increasing life expectancy.
Many people who have a hip or knee replacement these days do so with the
expectation of returning not only to work, but also to an active lifestyle.[10]
3.11
Other submitters pointed to Australia's ageing population to explain the
increase in utilisation.[11]
Specifically, older Australians make up a larger proportion of the
insured cohort.[12]
3.12
Representatives from the Department of Health (Department) suggested
that Australia's ageing population and the ability to safely provide a wider
range of medical services to an older cohort was leading to increased
utilisation:
I think the underlying cost pressures driving premiums up are
that people are getting older. Doctors and technology companies are inventing
more and more things that can be done to folk, especially as they get older.
Anaesthetic technology has now advanced to the point that 80-year-olds can be
anaesthetised safely for things that wouldn't have been done 15 years ago.[13]
3.13
The Grattan Institute agreed with the Department's assessment.[14]
3.14
Private Healthcare Australia also explained to the committee that an
ageing population has an effect on private health insurers because older
Australians are 'more highly represented in PHI [private health insurance] than
younger age groups and cost significantly more in healthcare than younger
groups'.[15]
3.15
Private Healthcare Australia's observation about the demand and cost of
healthcare in older populations is supported by data published by the
Australian Prudential Regulation Authority (APRA) that demonstrates that
greater hospital benefits are paid to persons in older age groups.
Graph 3.1—Hospital treatment benefits by age
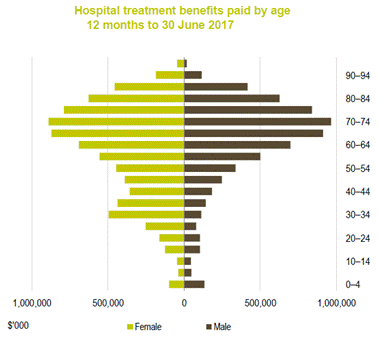
Source: APRA, Private
Health Insurance Quarterly Statistics, June 2017, p. 6.
Medical costs
3.16
Private Healthcare Australia and its members told the committee that
medical costs were also contributing to health inflation and placing pressure
on private health insurance premiums.[16]
3.17
Hirmaa, which represents not-for-profit and restricted membership funds,
similarly told the committee that the rising cost of medical services was
placing pressure on private health insurance premiums:
We would love premiums to be even lower, but unfortunately
insurers have to set premiums in line with the growing cost of medical
services.[17]
3.18
The Australian Medical Association (AMA) disagreed that the increased
cost of medical services was a substantial contributor to private health
insurance premiums, saying:
Medical expenses are a small proportion of total benefit
outlays for private health insurers. Medical expenses have remained static at
around 16 per cent since 2007. In fact, administration expenditure by private
health insurers is around 10 per cent. So it is costing insurers almost as much
to run their business as it is to pay the doctors who treat their customers.[18]
3.19
The APHA also disagreed that medical expenses were significantly impacting
premiums. According to APHA's research, once adjusted for inflation, increased
medical costs only accounted for 1.1 per cent of the growth in benefits
paid to patients.[19]
The APHA considered that utilisation, inflation and the number of insured
people had a greater effect on premiums.[20]
Private patients in public
hospitals
3.20
Another factor that may be placing pressure on premiums is the practice
of insured patients being treated privately in public hospitals. The committee
heard that consumers are often encouraged to use their private health insurance
to 'help the hospital' or to obtain benefits like a private room, their choice
of doctor or faster admission to surgery.[21]
3.21
The APHA told the committee that it believes that this practice has
contributed significantly to pressure on premiums:
Private Healthcare Australia has equated that to a six per
cent increase in premiums; premiums are six per cent higher than they would
otherwise be if that outlay wasn't there.[22]
3.22
Bupa Australia explained that whilst using their private health
insurance in a public hospital may not leave the consumer out-of-pocket,
consumers are not necessarily informed that using their private health
insurance in a public hospital contributes to the overall pressure on premiums.[23]
This practice will be discussed further in Chapter 4.
Remuneration and management
3.23
Several submitters to this inquiry highlighted that private health
insurance companies have moved from being structured as member-owned
not-for-profit mutuals to being large corporations.[24]
The effect of that change is that profit becomes a substantial consideration
for companies.[25]
3.24
Of Australia's 37 private health insurers, 13 operate as for-profit
companies.[26]
Those for-profit companies have been generating 'substantial' profits in recent
years.[27]
3.25
In 2015–16, Australia's 37 private health insurers made $1596 million in
profit before tax and $1252 million after tax.[28]
3.26
In 2016–17, Australia's 37 private health insurers made $1822 million
before tax and $1396 million after tax.[29]
3.27
Some submitters to the inquiry argued that the need to generate a profit
and a return to shareholders has fuelled a rise in premiums. The AMA told the
committee:
The shift to a full-profit industry has created the need to
ensure that there are sufficient profits to allow a return to shareholders.
This is driving much of the growth in increased premiums.[30]
3.28
Other stakeholders, such as the Medical Technology Association of
Australia (MTAA), suggested that private health insurers' rising profits
indicated that private health insurers had capacity to reduce premiums further:
The evidence of private health insurers' increasing profits,
increasing cash reserves and increasing CEO salaries suggests that they should
do some belt tightening of their own to keep premium growth to a CPI [consumer
price index] level.[31]
3.29
According to APRA, the industry average for management expenses was
8.5 per cent in 2015–16 and 8.8 per cent in 2016–17.[32]
3.30
Private health insurers disagreed that management expenses were
contributing to rising premiums.[33]
Instead, private health insurers indicated that their management expenses were
relatively low compared to other types of insurance.[34]
3.31
Representatives of hirmaa told the committee that:
My funds operate on very narrow management expense ratios, and
that includes salaries for running the fund. There's been no jump-up in MER [management
expense ratio] within my funds. It's very narrow, and you don't have that MER
for anyone else in the health supply chain. If there were a jump in the MER,
the management expense ratio, I would say, yes, you'd have every right to
question why there is an increase in the management expense ratio, but there's
not.[35]
3.32
Representatives of Bupa Australia similarly indicated that they were
committed to keeping their management costs down:
We have committed internally next year to have our costs grow
by no more than one per cent. The only reason those costs are growing is
because we face rental costs with landlords and commission costs for some of
the things we do for people, like students and so on. There's just no way I can
easily get out of some of those costs.[36]
3.33
As the representative from hirmaa noted, management expense ratios are
published by APRA but submitters noted that there is currently a difference
between the levels of transparency required of insurers depending on whether
they are listed on the Australian Stock Exchange (ASX).[37]
3.34
One of those transparency factors is executive remuneration. Currently,
only the two ASX listed companies, Medibank Private and NIB, are required to
disclose what their senior executives are paid.[38]
3.35
Some submitters, such as Dr Stephen Duckett, Director of the Health
Program at the Grattan Institute, considered that all private health insurers
ought to disclose these amounts:
My view is that we should have requirements on health
insurance funds in the same way we have requirements on listed companies about
disclosure and about transparency of how they're spending the money.[39]
3.36
Some of the private health insurers the committee spoke to did not consider
that revealing executive remuneration would be a problem, but wanted it to be
consistent across the industry. Representatives of Bupa Australia told the
committee that:
We don't have a problem if it's done for the industry. People
could reasonably argue that where public money is being spent—as long as there
is consistency involving suppliers, medical device companies, even industry
associations and all the rest of it—it should be a matter for the public
record.[40]
3.37
Dr Rachel David, Chief Executive Officer of Private Healthcare
Australia, the peak body representing private health insurers, agreed that
executive remuneration ought to be disclosed in more areas of healthcare:
What you'd need to do is ensure that in the hospitals—whether
they be church, charitable or publicly listed—their senior executives do the
same; and I also believe quite strongly medical specialists and dental
practices as well.[41]
3.38
Whilst not all submitters agreed that the disclosure of remuneration
ought to necessarily extend to individual medical practitioners, Private
Healthcare Australia suggested that its members would not oppose greater
transparency:
Should our elected representatives or our regulators agree
it's in the community interest for a heightened level of disclosure to occur,
we certainly will not oppose that. We will comply with anything along those
lines that is required of us.[42]
Intermediaries
3.39
In Chapter 2, the committee considered the role of the
privatehealth.gov.au website in helping consumers select a policy. In that
chapter, the committee noted that the privatehealth.gov.au website was one of the
only independent comparison websites and that many other websites operate on a fee-for-placement
basis. On a fee-for-placement website, the private health insurer pays a fee or
commission to the website when an individual takes out a private health
insurance policy after using the intermediary's website.[43]
Bupa Australia and other submitters suggested that commissions paid to
intermediaries to facilitate consumers switching private health insurers may also
be contributing to rising premiums.[44]
3.40
The Private Health Insurance Intermediaries Association (PHIIA) told the
committee that the mission of its members was to increase market competition
and improve consumer outcomes.[45]
3.41
However, Bupa Australia told the committee that the commissions claimed
by intermediaries were large and did not assist consumers:
Comparators claim as much as 40 per cent of the first year's
premium as their commission for informing people of their choice. This fee
doesn't go to buying health services, it must be absorbed, and inevitably leads
to higher premiums. This causes further pressure on premiums each year.[46]
3.42
Bupa Australia suggested that removing commissions to intermediaries
would reduce pressure on private health insurance premiums:
Eliminating commissions that would have otherwise been paid
to on-line brokers, who currently capitalise on this gap, would flow through to
lower premiums for all customers.[47]
3.43
PHIIA however rejected suggestions that commissions paid to comparison
websites were increasing pressure on premiums:
In reality the comparators are just another sales channel,
such as TV, Facebook, Google etc., among various marketing costs. In many
instances, the cost of member acquisition via comparison sites is more
cost-effective – particularly for smaller funds – than undertaking their own
marketing activities and sales channels.[48]
Constraining factors
3.44
While all the factors mentioned in the previous section play a part in
increasing premiums, a combination of regulation, incentives and market factors
act to constrain rising premiums.
Regulation
3.45
The Commonwealth Government encourages people to take up private health
insurance to relieve pressure on state public hospitals and to 'provide
consumers with a greater choice of care options'.[49]
3.46
To ensure that patients with a high risk profile are not charged
prohibitive private health insurance premiums and insurers are not discouraged
from insuring high risk consumers, Australia's private health insurance market
is based on the principles of community rating and risk equalisation.
Community rating and risk
equalisation
3.47
Community rating is the principle that private health insurers cannot
discriminate between consumers seeking coverage on the basis of their health,
age or likelihood to claim.[50]
3.48
Community rating guarantees that anyone who wants to take out private
health insurance has access to it.[51]
In its Efficiency in Health report, the Productivity Commission noted
that 'community rating and other price regulations effectively act to
cross-subsidise private health insurance premiums'.[52]
The Department clarified that:
Community rating prohibits insurers from discriminating on
the basis of past or likely future health or risk factors such as age,
pre-existing condition, gender, race or lifestyle in the premiums that they
charge. Although community rating means that people who are older or sicker do
not have to pay higher premiums commensurate with their risk, it also means
that younger and healthier people pay more than they otherwise would.[53]
3.49
Community rating is supported by a system of risk equalisation. In its
submission, the Department explained the rationale for risk equalisation in the
private health insurance market:
Risk equalisation attempts to adjust for the risk of adverse
selection. It is designed to spread the burden of high cost claims across all
insurers, helping to keep them all financially viable...These arrangements are
designed to ensure that insurers (and policy holders with those insurers) with
higher numbers of older members or high users are not financially disadvantaged
compared with those insurers with a younger or healthier membership.[54]
3.50
Submitters to this inquiry were almost unanimous in their agreement that
community rating and risk equalisation are important to the effective operation
of the existing private health insurance regime.[55]
Private health insurance rebate
3.51
Two other elements of the existing regulatory regime are designed to
help to control the price of private health insurance premiums: the premiums
reduction scheme—commonly known as the private health insurance rebate—and the
Minister for Health's approval of premiums.
3.52
The private health insurance rebate was introduced from 1 January 1999
as one of three government incentives to encourage people to take out private
health insurance cover during the late 1990s and early 2000s.[56]
3.53
Today, the existing structure of the rebate is based on the age and
income of the beneficiary/beneficiaries of the private health insurance policy.[57]
Since 2014, the rebate has also been reduced by up to one percent per year.[58]
3.54
Some submitters considered the rebate to be an inefficient use of public
money.[59]
For these submitters, the inefficiency stemmed from the fact that a plurality
of private health insurers lacked the efficiency of scale of a universal health
system.[60]
3.55
The Grattan Institute questioned the value of the rebate and stated that
other factors, such as the lifetime health cover loading, had a much more
significant effect on participation than the introduction of the rebate.[61]
3.56
The Grattan Institute also noted that changes to the rebate for older
and wealthier Australians in 2005 and 2014 did not appear to change their
participation rate in private health insurance.[62]
Therefore, the Grattan Institute advocated for gradual curtailment of the
rebate.[63]
3.57
Some private health insurers expressed concern about the impact of the
annual reduction in the rebate: representatives of hirmaa called for a price
floor to be set to ensure that the rebate does not drop below 25 per cent.[64]
Private health insurers want a price floor to be established as the diminishing
rebate is compounding the affordability problem caused by rising premiums:
...the Australian government rebate is no longer at 30 per
cent; it is in the 25 per cent zone and it is dropping by a per cent every
year, and it is means-tested. That means that only those who really deserve it
receive the rebate and it is dropping by a per cent a year. So, if a health
fund puts up premiums by four per cent, you can add another per cent through
the Australian government rebate dropping as well, and that is causing a lot of
cost pressures.[65]
Minister's approval of premiums
3.58
The Minister for Health (Minister) is required to approve private health
insurance premium increases, unless there is an overriding public interest
reason not to do so.[66]
3.59
Mr Shaun Gath, the former head of the Private Health Insurance
Administration Council, suggested that the law was drafted to reflect a
compromise:
There is little doubt that their purpose was to reflect a
compromise, namely that insurers could reasonably expect that their
application would be approved (the Minister ''must'' approve ...) subject only to
some quite exceptional event where a decision to approve would actually be ''contrary
to the public interest''. In practice, however, ministers of both political
persuasions continued to regard themselves as primarily responsible for an approval
process where intense micro-scrutiny was applied to the applications (often
with little transparency) with a view to approving the lowest increase
prudentially acceptable.[67]
3.60
Dr Duckett explained that it seemed to be contrary to private
health insurers' interests to propose higher than needed fee increases, which
led him to conclude that price may not be the most important factor for private
health insurers:
When Minister Ley, I think it was, knocked them back...they
came back with lower proposals, which suggests that there was padding in their
initial proposal. That suggests they don't care about fee increases, because
they have a whole lot of other structures which stop people dropping out as
much.[68]
Medicare levy surcharge and
Lifetime health cover
3.61
Other structures that encourage individuals to maintain coverage are the
Medicare Levy Surcharge (MLS) and the Lifetime Health Cover (LHC) loading.
3.62
The MLS is a tax applied to persons who earn over a threshold amount and
do not hold private hospital insurance.[69]
Between 2014–15 and 2017–18 the MLS was calculated in accordance with the table
below.[70]
Table 3.2—MLS income thresholds 2014–15 to 2017–18

Source: Department, Submission
127, p. 24.
3.63
The Department explained that the LHC was an incentive that was
introduced on 1 July 2000 to 'encourage people to take out hospital insurance
earlier in life, and to maintain their cover throughout their life'.[71]
3.64
It works by applying an extra two per cent loading to their private
hospital insurance premium for each year after the age of 30 that the person
did not hold an appropriate level of cover and allows the insurer to charge the
person the premium plus the loading for the next ten years.[72]
3.65
Together, the LHC loading and the MLS are intended to encourage younger,
healthier people to enter the private health insurance risk pool earlier than
they otherwise might.
3.66
According to Private Healthcare Australia the MLS and the LHC provide
stability to Australia's private health insurance market:
Market research estimates these measures together, underpin
75% of demand for PHI [private health insurance], and successfully stabilised
uptake of private health insurance at its current level of approximately 50% of
the population.[73]
3.67
Consumer surveys also confirmed that the MLS and the LHC were important
factors in individuals' decision to maintain coverage. A survey by Choice found
that 34 per cent of respondents considered avoiding paying the MLS to be a key
reason to take out private health insurance while another 24 per cent of
respondents considered avoiding LHC loading to be a key reason.[74]
Among households earning over $150 000, 55 per cent cited avoiding the MLS
as a key reason for taking out private health insurance.[75]
Market factors
3.68
As noted above, an older insured cohort that is more likely to claim
will put upward pressure on premiums. Therefore, to reduce pressure on
premiums, private health insurers, collectively, need to attract younger,
healthier people to join the insured pool who are less likely to make a claim.[76]
3.69
Some submitters raised concerns that a failure to attract younger people
to take up private health insurance may lead to a 'death spiral':
An important consideration regarding the incentive policy is
the age structure of the insurance pool it generates. Generally speaking, in
order to maintain a sound risk structure and affordable premiums, low risk
insurees are required to balance out the high risk insurees. An imbalance in
the insurance pool toward high risk individuals will drive the premiums up
which may cause more low risk persons to drop out, leading to further premium
increases. This process is known as the insurance market 'death spiral'.[77]
3.70
While participation numbers are down, APRA disagrees that the insurance
market is headed for a 'death spiral'.[78]
However, some private health insurers suggested that the existing incentives—the
rebate, LHC and the MLS—are not sufficient to encourage younger, healthier
people take out private health insurance:
Current sticks and carrots, including the Medicare Levy
Surcharge, Lifetime Health Cover and even the PHI [private health insurance] Rebates,
don't do enough to make the product sufficiently attractive to healthy under
30s. It is this group that is essential to deepening the community rated risk
pool and therefore keeping premium growth down.[79]
'Reverse' Lifetime health cover
3.71
Some private health insurers suggested that the government implement a
'reverse' LHC to provide a financial incentive for people under 30 to take out
private health insurance.[80]
3.72
On 13 October 2017, the Minister announced that the insurers would be
allowed to discount premiums for people who take out private health insurance
between the ages of 18 and 29.[81]
3.73
Under the plan, a discount of up to 10 per cent could be applied to
premiums until the person turns 40 when the discount would start to be phased
out.[82]
3.74
The Department confirmed that the purpose of this plan was to lower
premiums.[83]
3.75
However, some submitters raised concerns that an additional incentive
may not be sufficient for young people to take out private health insurance.[84]
Dr Duckett explained to the committee that even under the recently announced
plan he would not advise his daughter to take out private health insurance:
...it's not good value for money. She's 22, relatively healthy,
and until she turns 30 there's no particular reason for her to take out health
insurance at all. As the health insurers know, and as the government knows, the
whole point of the deductions is to encourage people into health insurance who
will not use their health insurance. That's the whole point of it.[85]
Junk/basic policies
3.76
The low value that junk/basic policies provide to consumers was
considered in Chapter 2. However, submitters to the inquiry explained that the
benefit of these policies is that their policyholders contribute to the risk
equalisation pool and place downward pressure on premiums:
They all contribute to the risk equalisation pool and,
therefore, the total pool of funds available to members, thereby keeping
overall premiums stable.[86]
3.77
The Department agreed that one reason junk/basic policies are allowed to
continue is because they play a role in placing downward pressure on premiums.[87]
Some submitters also observed that people may see some value in a policy that
allows them to be treated as a private patient in a public hospital or allows
them to contribute to the risk equalisation pool.[88]
3.78
The Department agreed that some people do see value in the product:
...there are a greater or lesser number of people who do see
value in those products. They do offer cover for some things. You can question
whether you get your money back. Most people with health insurance don't get
their money back in the short run, but that's what insurance is.[89]
Prostheses
3.79
Some submitters also raised concerns about the price of prostheses
increasing pressure on private health insurance premiums.[90]
3.80
The term 'prosthesis' specifically refers to a surgically implantable device,
such as a cardiac pacemaker or an intraocular lens in a cataract surgery.[91]
3.81
Earlier this year, the Community Affairs References Committee completed an
inquiry into Price regulation associated with the Prostheses List Framework.[92]
The inquiry examined the impact of benefit-setting on the price of prostheses
available and used for privately insured patients.
3.82
Submitters to both inquiries noted that prostheses benefits amount to
approximately 14 per cent of hospital rebate expenditure for private health
insurers.[93]
The committee also heard evidence that the different prices were being charged
for prostheses in public and private hospitals and that the differential
between the price paid in public and private hospitals was having a substantial
impact on premiums.[94]
3.83
In its inquiry into Price regulation associated with the Prostheses
List Framework, the committee made 16 recommendations including that the 'the
nature and costs of services associated with a medical device on the Prostheses
List be disclosed separately to the cost of the device'.[95]
3.84
Prior to the conclusion of the committee's inquiry, the Commonwealth Government
announced and implemented an initial review and reduced the benefits for
certain groups of items on the Prostheses List, signalling that this would
represent an initial saving of $86 million and $500 million over 6 years.[96]
3.85
The government's response to the inquiry report agreed to ensure that
there is greater transparency in relation to decisions and benefit setting by
the Prostheses List Advisory Committee, and to continue the process of refining
the number, range and benefit level of items available on the Prostheses List.[97]
3.86
On 13 October 2017, the Minister announced that a round of benefit
reductions would commence on 1 February 2018 to save private health insurers $188 million
in 2018.[98]
Combined with further benefit reductions in subsequent years, the government
announced that:
Total estimated savings to private health insurers over the
next four premium years (2018 to 2021) are more than a billion dollars.[99]
3.87
This agreement with the MTAA, who represent device manufacturers, is
designed to place downward pressure on premiums. The Minister announced that:
Private health insurers have publicly stated that every $200
million in prostheses benefits reductions will decrease private health
insurance premiums by one per cent.[100]
3.88
To ensure that the Prostheses List savings were passed on, the MTAA
suggested that the Australian National Audit Office should audit the books of
all private health insurers:
MTAA would like to propose that private health insurers be
required to open up their books to the Australian National Audit Office, to
verify that they are passing on all of these savings, and to publish revenue
and claims payout ratios. This would be entirely appropriate for an industry in
receipt of $6 billion in taxpayer funds. We would encourage the committee to
consider this as a recommendation that should be enshrined in legislation. A
simple amendment to the Private Health Insurance Act should be able to
facilitate this.[101]
3.89
Dr Duckett also suggested that an audit would be possible:
I think the Auditor-General has follow-the-dollar powers, and
may be able to initiate an audit of that kind. It would possibly be impossible
to tell what the impact of the prostheses changes are going to be. If I were a
health insurance fund I'd say, 'Yes, we made all those savings and we've
ploughed them back because our fees aren't increasing next year as much.'[102]
3.90
The private health insurers did not oppose the suggestion of an audit:
In the premium round you have to be very specific about the
claims on medical devices, how they've decreased, get the actuaries to do the
modelling, put it in the premium and ensure they have been passed on. If that
was found not to be sufficient, and it was suggested by the government that the
ANAO's involvement would add something, we would open our books and show them.
There is absolutely nothing to hide. We were the ones who put this issue on the
table—that we would pass on all the savings in the prostheses list negotiation.
We were the ones who put our hands up and said that we would do it. There is
nothing to hide.[103]
3.91
However, APRA was less certain that an audit would be a significant
benefit as it considered that it would be clear if additional funds were being
held by the private health insurers:
In terms of whether they have passed on savings, I think we
again understand that, if you look at the numbers over the last 10 years, the
MERs [management expense ratios], the amount of benefit payments made each year
happen to have remained relatively the same over that period. So it would suggest
that, if the costs are going up and premiums are going up, there are no excess
profits being held within the institutions, given that the benefit payments
have stayed around 85 to 86 per cent, the MERs have been at the same per cent
and the net margin has been at 4½ or thereabouts...I personally don't think
there's a lot to be gained.[104]
Will premiums go down?
3.92
Despite the government's recent announcement, no submitter to the
inquiry expected that health insurance premiums were likely to drop in the
short term as costs will continue to rise.[105]
3.93
The Department summarised the position of many of the submitters:
[Private health insurance premiums] will not go up as fast as
they otherwise would have done.[106]
3.94
Instead, submitters suggested that upward pressure would continue to be
placed on private health insurance premiums. APRA noted that over the longer
term rising premiums had the potential to be a significant issue:
We've identified [the private health insurance business
model] as an emerging risk. We see it as a long-term challenge for the
industry. With the participation rates coming down amongst the younger cohort,
it's going to put pressure on pricing and, of course, that's a long-term structural
issue that the industry needs to face. Our role, obviously, is to understand
how the industry is actually going to cope with that to ensure that it remains
sustainable going forward.[107]
Committee view
3.95
The committee acknowledges that there are a number of factors that are
increasing underlying costs for private health insurers including utilisation,
an ageing demographic, intermediaries, prostheses costs and operating margins.
3.96
The committee considers that the existing principles of community rating
and risk equalisation are key to ensuring equity in Australia's private health
insurance market and supports their continuation.
3.97
The committee notes the reforms announced by the government on
13 October this year. The committee's comments on these reforms are included
in Chapter 5.
3.98
The committee also notes the substantial profits that private health
insurers are recording which to a certain extent undermines their argument that
underlying costs are driving up premiums.
Navigation: Previous Page | Contents | Next Page