Consumers
2.1
This chapter considers the difficulties faced by private health insurance
consumers in terms of affordability and out-of-pocket costs. This chapter also
examines why there has been an increase in the number of individuals dropping
or down-grading their private health insurance.
Number and content of policies
2.2
Throughout the inquiry, submitters raised concerns about the complexity
of private health insurance products and the lack of information provided by
insurers.[1]
Many submitters noted that a greater number of available policies, changes to
available benefits, difficult to understand terminology and a rise in
non-comprehensive policies added to complexity for consumers.[2]
2.3
In June 2015, the Australian Competition and Consumer Commission (ACCC) noted
there were approximately 46 500 private health insurance products on offer.[3]
At the same time, research has suggested that up to 60 per cent of Australians
have low levels of health literacy.[4]
2.4
The Commonwealth Ombudsman and Choice emphasised that health insurance
policies are often unnecessarily complex and difficult for consumers to
understand.[5]
Both submitters noted that this complexity is compounded by private health
insurers using different terminology to explain similar concepts. Choice noted
that 'complex jargon makes it challenging for consumers when reading, comparing
and understanding their policies'.[6]
The Commonwealth Ombudsman further stated that the 'information provided by
health insurers causes a number of problems for some consumers who consider the
policy they received does not match their expectations.'[7]
One consumer noted the difficulty in finding appropriate coverage and comparing
it to other private health insurance policies:
My wife is a doctor and we have two children. After having
decided recently that we would not be having any more children we thought we
would investigate if we could obtain a better rate from another fund as the
Doctors fund does not let you separate maternity cover. We spent a few weeks
doing so but ended up very confused. Trying to find which [policy] is the best
for the consumer is very difficult and the government needs to act.[8]
Exclusions, co-payments and changes
2.5
The number of policies with exclusions or co-payments has increased
dramatically in recent years.[9]
According to the Australian Private Hospitals Association (APHA) citing Australian
Prudential Regulation Authority (APRA) data, the number of people covered by
exclusionary policies has increased from seven per cent in June 2007 to 40
per cent in 2017.[10]
2.6
The Department of Health (Department) noted that the most commonly
excluded services include: heart investigations and surgery, eye surgery,
pregnancy and birth related services and hip and knee replacements.[11]
2.7
These exclusions mean that individuals who use the private healthcare
system are left with a lower value policy.[12]
Day Hospitals Australia noted that the rise in exclusions can lead to unnecessary
stress for policy holders when they require care, particularly if exclusions in
a policy are not properly explained:
The failure by health funds to clearly explain the policy
holders [sic] cover and the associated product restrictions and exclusion, at
the time of purchase, creates enormous stress for the consumer when they
require hospital services.[13]
2.8
The committee heard evidence regarding the influence that co-payments
and 'gaps' have on driving up medical costs.[14]
While some health funds have 'no gap' arrangements with certain providers,
these may not be the providers the patient is referred to. A patient diagnosed
with breast cancer experienced the financial impact of this gap:
I queried the gap with the private health fund and they said
to me: 'Well you've got the wrong surgeon' and I said: 'Well when you're told
you've got breast cancer, you don't say "hold on a minute, I'll go find
another surgeon"'. You're sort of overwhelmed by the diagnosis and you
want to get the treatment. I had confidence in him (the surgeon) but not in his
bills. It was a lot of money we weren't expecting to pay.[15]
2.9
Another consumer noted the large and unexpected out-of-pocket payment
they faced when their policy changed despite holding top cover:
I had a 15-year policy with Medibank Private which I thought
was "Top Cover" but when the daughter needed braces and an operation,
no cover. $16,000 out of pocket despite the $3500 per year payments. Policies
change and cover degrades we were not aware [sic].[16]
2.10
COTA Australia noted that older people are also susceptible to
unexpected out-of-pocket costs:
A recurring story...is older people having maintained [private
health insurance] for decades, only to find when they need to draw on it in
later life they cannot realise the benefits because they cannot afford to meet
the co-payments or other out-of-pocket costs associated with a procedure or
treatment.[17]
2.11
Dr Michael Gannon, President of the Australian Medical Association
(AMA), outlined the case of an elderly woman who was recently told by her insurer
that her surgery was covered. However, the insurer decided not to pay after the
surgery was performed, leaving the woman out of pocket by $7000.[18]
Dr Gannon suggested that the insurer may not have paid because evidence of the
clinical necessity of the surgery was not provided to the insurer prior to
surgery.[19]
2.12
The AMA suggested to the committee that changes to a policy after
purchase had the capacity to shake consumer confidence in private health
insurance:
When policies change haphazardly and reduce choice, consumers
lose faith that the product provides value for money. Private health insurance
provides choice for the patient and without that choice, its value is diminished.[20]
Affordability and rising out-of-pocket costs
2.13
Some submitters raised concerns about rising out-of-pocket costs and the
difficulties faced by consumers in accurately estimating these costs before and
after they received treatment.[21]
2.14
A 2015 poll on healthcare and insurance in Australia conducted by Ipsos found
that Australians were most concerned about the affordability of private health
insurance.[22]
Of those surveyed, 61 per cent of people identified the cost of premiums as the
primary reason for allowing their private health insurance to lapse.[23]
A further 71 per cent of people without private health insurance reported that
the primary reason was that premiums were too high.[24]
Further research commissioned by Private Healthcare Australia shows that if trends
of low-wage growth and increasing premiums continue, private health insurance will
'potentially become unaffordable for up to one in five current hospital
policyholders within the next 5-6 years'.[25]
2.15
Ms Alison Verhoeven, Chief Executive of the Australian Health and
Hospitals Association (AHHA) noted that numerous Australians over the age of 50
held concerns that affordability was a barrier to purchasing private health
insurance.[26]
2.16
Ms Verhoeven told the committee that the affordability of private
health insurance was affecting uptake among the Aboriginal and Torres Strait
Islander (ATSI) community and the elderly.[27]
Ms Verhoeven referred the committee to the most recent data available, an
Australian Institute of Health and Welfare study from 2012–13, that showed that
only 20 per cent of ATSI adults had private health insurance and 72 per cent
indicated they could not afford private health insurance, or believed it was
too expensive.[28]
2.17
Concerns about affordability have led to an increase in the number of
members who have downgraded their private health insurance. As the figure below
demonstrates, HBF is one company that has experienced an increase in policy
downgrades.
Graph 2.1—HBF Policy upgrades and downgrades between FY2010–11
and FY2016–17
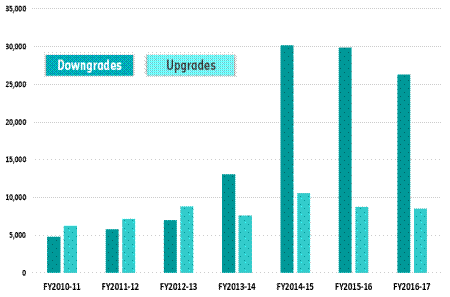
Source: HBF, Submission 63,
p. 6.
2.18
HBF also noted a dramatic increase in the number of its members who took
out 'less comprehensive products'.[29]
In 2009–10, 31 per cent of HBF members chose 'top hospital' coverage.[30]
By 2017 the percentage of HBF members who chose 'top hospital' cover had fallen
to 14 per cent.[31]
2.19
Submitters expressed concern about rising out-of-pocket costs. In
Australia, out-of-pocket costs now account for roughly 20 per cent of
healthcare expenditure.[32]
According to the AHHA, this figure is higher than other similar countries such
as Canada (14 per cent), New Zealand (13 per cent) and the United Kingdom (10
per cent), though similar to the Organisation for Economic Co-operation and Development
(OECD) average.[33]
2.20
A similar trend in higher out-of-pocket costs was identified by a number
of specialist health organisations. The Australian Federation of AIDS Organisations
and the National Association of People with HIV Australia noted concerns about
the affordability of HIV medication:
Each time a medication is dispensed, there is a co-payment –
currently $38.80 at the general rate, and $6.30 at the concessional rate. In
addition to the costs of HIV medication, many people with HIV pay additional
co-payments for treatments associated with other HIV-related medical
conditions, for example the control of lipids, diabetes and depression. Research
shows that these cumulative costs cause financial stress, and result in some
people forgoing treatment, leading to lower medication adherence. The outcomes
of this are poorer individual health outcomes and increased onward
transmissions, as a result of viral rebound.[34]
2.21
The Australian Dental Prosthetists Association voiced concern that
'dental services generally fall under ancillary or extras cover'.[35]
As a result, roughly 10 per cent of insured adults pay all their dental
expenses and 76 per cent registered dissatisfaction with the level of rebates
received for dental treatment.[36]
2.22
Other issues relating to out-of-pocket costs in dentistry are canvassed
in Chapter 4.
2.23
The committee received evidence regarding the scale of fees charged by
some specialists.[37]
The Royal Australasian College of Surgeons (RACS) drew the committee's
attention to the Surgical Variance Report 2017: General Surgery.[38]
The surgical variance report revealed that there can be significant variations
in separation costs, surgeon out-of-pocket costs and out-of-pocket costs for
other medical services.[39]
Private Healthcare Australia noted that a market exists in specialist fees and
it is information that consumers do not have access to.[40]
2.24
RACS acknowledged that some surgeons charged excessive fees and that
disclosure of those fees may be one way to address that problem.[41]
Dr Stephen Duckett, Director of the Health Program at the Grattan
Institute suggested that publishing surgeons' fees would be relatively simple:
One option, of course, is to say, 'Well, if you want to
charge patients you can charge what you like, but there's going to be no rebate
if you charge more than 50 per cent above the schedule'—or whatever you like
and so force some discipline into the market. The government already collects
information about what fees are charged and it would be relatively easy for
Medicare to publish the information about fees charged by individual doctors by
procedure.[42]
2.25
Dr Duckett also suggested that transparency data should not just
include fees but a range of outcomes at both the surgeon and hospital level:
My view is that we should publish the complication rates. We
already collect information on that. On every patient discharge from every
public and private hospital we collect diagnoses that occurred during the
course of admission, whether there was an infection, or a laceration during
surgery, and so on. We should publish those rates for hospitals—at the hospital
level. Because there is a private contract between the doctor and the patient,
we should also publish that information where such a private contract exists.
That is, the customer should know in advance what the risk of a complication is
with the surgeon from whom they are purchasing their service.[43]
2.26
RACS told the committee that it did not oppose the public disclosure of
surgeons fees, but the college did not wish to be the body to publish them:
We're not opposed; it's just how it's done. We wouldn't be
doing it. We're not opposed to an independent agency doing that, as long as
they're using the right parameters to judge the fees themselves and how they're
presented. Our view is that the best way of managing this is to make sure the
consumer has all of the information that they need and also to make sure that
they ask the right questions from the very start.[44]
2.27
Submitters commonly raised concerns that increasing out-of-pocket costs are
leading to worse health outcomes because individuals are either rejecting or
delaying treatment.[45]
2.28
Lynch Syndrome Australia noted that 19 per cent of respondents delayed
their surveillance or treatment of Lynch Syndrome due to financials costs. A
further eight per cent delayed their cancer treatment for financial reasons.[46]
2.29
The AHHA and the Grattan Institute, among others, highlighted that
out-of-pocket costs disproportionately disadvantage those on low incomes.[47]
2.30
On 13 October 2017, The Hon Greg Hunt MP, Minister of Health (Minister) announced
that a committee would be established 'to consider best practice models for the
transparency of out-of-pocket costs'.[48]
'Junk' policies
2.31
A number of submitters raised concerns about the use of so-called 'junk'
or basic policies. These policies are often cheap and are taken up by people
who perceive a lack of value in more expensive private health insurance coverage.[49]
2.32
'Junk' policies include policies which provide coverage for a small
number of accidents such as knee reconstructions and investigations but have
the majority of services and illnesses excluded or covered in a public
hospital. They also often offer private hospital cover for accident and
ambulance only.[50]
2.33
Choice identified that often 'junk' or basic policies are taken out by
consumers who either:
-
want the cheapest policy possible, but do not realise the policy offers
limited coverage; or
-
who know the policy offers limited coverage, does not intend to
use it and take it out solely for tax purposes.[51]
2.34
The Australian Nursing and Midwifery Federation (ANMF) raised concerns
about the current tax incentives to encourage consumers to maintain private
health insurance and noted a recent ACCC report that found that tax incentives
are 'driving consumers to lower-priced policies than they would prefer, with an
emphasis on tax rather than health outcomes'.[52]
2.35
Some submitters called for an end to 'junk' policies because they believe
that they deliver poor value for consumers.[53]
Others called for the withdrawal of the rebate from these 'junk' policies.[54]
2.36
The Royal Australian and New Zealand College of Obstetricians and
Gynaecologists (RANZCOG) and the National Association of Specialist
Obstetricians and Gynaecologists (NASOG) raised concerns about the
disproportionate effect these junk policies have on women holding private
health insurance.[55]
RANZCOG argued in their submission:
These policies may cover small proportions of treatments
provided in private hospitals...Because these policies usually do not cover
treatments in private hospital for the most important and common needs of women
– maternity care, menstrual disorders, gynaecological malignancies, prolapse
and incontinence, and private psychiatric facilities in case of a perinatal
mental health condition, their value is questionable.[56]
2.37
However, some people do consider that basic policies afford some
benefit.[57]
The benefit is mostly attributed to contributions made to the risk equalisation
pool. This is considered in greater detail in Chapter 3.
Groups who face additional barriers to using private health insurance
2.38
The committee received evidence from groups who considered that they
face additional barriers to using their private health insurance. This included
people living in rural and regional Australia, people suffering from chronic
diseases and those diagnosed with certain illnesses.
Rural and regional consumers
2.39
The committee received substantial evidence from consumers in rural and
regional areas. In particular, numerous submitters drew attention to the lack
of contracted providers in rural towns.[58]
The paucity of private health infrastructure in rural areas can be seen in the
figure below.
Figure 2.1 Locations of private
hospitals in Australia
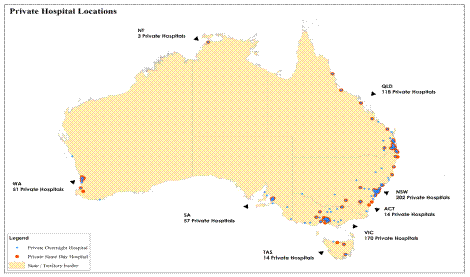
Source: Department, Submission
127, p. 6.
2.40
The National Rural Health Alliance (NRHA) noted that 52.3 per cent of
individuals living in regional and remote communities do not have private
health insurance, compared to 39 per cent in major cities.[59]
2.41
The NRHA argued that private health insurance products need 'to enable
better access to services and supports designed specifically to enhance access
for rural and remote Australia'.[60]
The NRHA's recommendations include an increased range of benefits for
non-hospital based services in rural areas, increased access to higher rebates
to cover transport and accommodation when forced to travel to receive medical
services and progressive reductions based on geographic remoteness to encourage
people to take out private health insurance.[61]
2.42
People living in rural areas have also noted their frustration at their
inability to access 'preferred providers' and therefore face higher
out-of-pocket expenses.[62]
In regional areas the scarcity of these providers means that consumers are
required to travel long distances if they wish to access one.[63]
2.43
Due to the lack of health facilities in rural areas, patients noted they
would often have to travel long distances to receive treatment.[64]
As a result of limited access to facilities and lower access to medical
specialists compared to urban areas, regional Australians have substantially
lower levels of private health membership.[65]
2.44
Despite access to fewer medical facilities, individuals who live in
rural and remote areas pay the same premium as those living in urban centres. Services
for Australian Rural and Remote Allied Health (SARRAH) noted that this is
compounded by the additional financial costs faced by those in rural areas who
often have to travel greater distances and face additional costs to access
adequate healthcare.[66]
These issues often lead to rural and regional consumers accessing health
services 'less frequently' or relying 'on intermittent outreach services'.[67]
2.45
Numerous submissions have therefore recommended initiatives to improve
the value of private health insurance for consumers living in regional and
remote locations. The Australian Physiotherapy Association recommended rebates
for the non-hospital option to include any transport or accommodation costs to
assist rural patients.[68]
The ANMF recommended the 'provision of incentives for private practitioners to
operate in rural areas' and the 'leveraging of models of care that would
enhance access, such as telehealth, remote monitoring and the funding of nurses
and allied health professionals to deliver care, closer to people's homes'.[69]
2.46
SARRAH have suggested that private health insurance products 'should be
tailored to meet the needs of indigenous and non-indigenous Australians living
in rural and remote Australia'.[70]
This includes improving access and value through increasing the range of
benefits for non-private hospital services and increasing transport and
accommodation benefits.
2.47
On 13 October 2017, the Minister announced that insurers would be able
to offer accommodation and travel benefits for people in rural and regional
areas.[71]
Chronic illnesses
2.48
Other submitters raised concerns about high out-of-pocket expenses for
people diagnosed with chronic diseases.[72]
Allied Health Professions Australia stated that high costs for this cohort
'reduce the accessibility of services and results in consumers avoiding
treatment and increasing their risk of avoidable health issues'.[73]
2.49
Breast Cancer Network Australia told the committee that in 2016 it
conducted research into the financial impact of breast cancer. This research
showed that women with private health insurance 'typically pay more than twice
as much for their breast cancer treatment and care than women without private
health insurance'.[74]
2.50
The Haemophilia Foundation Australia also undertook an internal survey
of individuals diagnosed with the disease. This found that 34 per cent of
individuals used the public health care system.[75]
The reasons cited for using the public system instead of private healthcare
included, management of the bleeding risk and that respondents saw 'limited
value in using public health insurance for extras...as the benefits were low and
far outweighed by the premium costs'.[76]
The majority of respondents said they were debating whether they could afford
private health insurance.[77]
2.51
A number of submitters also drew attention to the significant
out-of-pocket expenses incurred by individuals diagnosed with particular
illnesses. Parkinson's Australia noted that patients can face costs of as much
as $50 000 depending on their level of private health insurance coverage.[78]
2.52
Parkinson's Australia told the committee that the high costs associated
with treating particular illnesses could be very substantial:
Parkinson's Australia is aware of people who have had to
mortgage their homes or have had to dip into their superannuation to finance
their DBS [deep brain stimulation] treatment. There are also many who cannot
afford this treatment at all even though it is appropriate for them and is
considered cost effective.[79]
2.53
The Royal Australian College of General Practitioners (RACGP) noted that
chronic disease management is an area where private health insurance can
provide long-term saving to patients.[80]
In particular it noted that '[private health insurance] organisations can
improve the health of their members and Australians more widely through
supporting services not funded through Medicare'.[81]
These include chronic disease management, care coordination and general
practice modernisation.
2.54
Product design relating to the management of chronic illnesses is
considered further in Chapter 4.
Transparency
2.55
Some submitters to the inquiry raised concerns that consumers find it
difficult to understand what their health insurance product covers.
2.56
A common recommendation throughout this inquiry has been for the
implementation of standardised terminology for health insurance products. The
AHHA, for example, recommends a 'mandated simplification and consistency of
product information provided across the sector'.[82]
It was proposed that this would allow consumers to better compare private
health insurance products and increase transparency in the sector.
2.57
The Private Health Insurance Ombudsman (PHIO) provides information for
consumers to understand private health insurance policies via the consumer
website privatehealth.gov.au.[83]
In 2016 this website attracted 1.2 million unique visitors, approximately
one-eighth of the roughly 10 million health insurance consumers in
Australia.[84]
When questioned on these figures, Mr David McGregor, Director of Private Health
Insurance for the Commonwealth Ombudsman, said this was not a 'surprising
figure'.[85]
Mr McGregor also noted that there was currently no allocation in its budget to
promote the website.[86]
2.58
A number of submitters suggested that better promotion of the website by
both the Commonwealth Government and private health insurers is essential to
increase transparency of the industry and to allow consumers to make better
informed decisions about the products available to them.[87]
2.59
Promotion of the PHIO-run site is critical because it is one of the only
independent comparison websites.[88]
Many of the other comparison websites are run by intermediaries, also known as
commercial comparison services.[89]
'Intermediary' is a broad term that includes comparators,—such as Compare the
Market, iSelect and Choosewell—agents and brokers who provide advice and
guidance to consumers about available products.[90]
These companies operate on commissions from private health insurers, but are
not necessarily transparent about the private health insurers they receive
commissions from, which can make it difficult for consumers to know if they are
being shown all of their available options.[91]
2.60
On 13 October 2017, the Minister announced a series of reforms including
a policy to redevelop the privatehealth.gov.au website to assist consumers in
choosing private health insurance products suited to their needs.[92]
The website will also see the introduction of a 'minimum data set' to
communicate private health insurance product data in an online format.[93]
2.61
The Commonwealth Government has also proposed a new system for categorising
private health insurance products. This includes the introduction of categories
('gold', 'silver', 'bronze' and 'basic') which place a minimum standard against
each category. This classification is intended to assist consumers to compare
and contrast private health insurance products. The Commonwealth Government will
seek to introduce a list of standard clinical definitions insurers will be
required to apply across all private health insurance documentation.[94]
2.62
Submitters to the inquiry generally welcomed the new classification
system, but agreed that consumers needed to be able to clearly understand what
they were covered for.[95]
Dr Gannon told the committee that:
With gold, silver, bronze, it is just absolutely important
that people understand what they're getting. And if gold means 'everything',
silver means 'everything with excesses or co-payments', if you must, and
'bronze' means 'a reduced level of service, but more than just junk', then we
can live with that. But what we want is people, your average member of the
community, to be able to understand it and to have something in their hands
that's actually worth something.[96]
Minimum standard benefits
2.63
Some submitters proposed that a new minimum standard for a complying
private health insurance policy be introduced. Currently, the only requirement
for a complying health insurance policy is that minimum benefits are provided
for psychiatric, rehabilitation and palliative care services.[97]
2.64
The Department explained that these requirements reflect concerns by
hospitals and other providers that insurers would not contract for those
services.[98]
2.65
NASOG suggested that obstetric services ought to be a mandatory
inclusion:
Australian society has an overriding responsibility to
support, and care for, the women of our nation who undertake the great
responsibility of our next generation. The inclusion of obstetric cover in the
design of all PHI [private health insurance] policies for women of childbearing
age is paramount, and should be a standard inclusion.[99]
2.66
In relation to obstetrics, RANZCOG made the argument that:
There is evidence that in the Australian community at least
half, and probably more, of all pregnancies are unplanned, so couples or women
don't have the opportunity to make provision through their cover beforehand. It
should not be an issue that they have to wade through thousands of policy types
in the hope that they will encounter or be able to select and buy a private
health insurance product that covers maternity.[100]
2.67
Other submitters singled out mental health care as a feature to be
included in all policies.[101]
Dr Duckett advocated for the inclusion of mental health as a minimum
requirement on the basis that people are unlikely to anticipate whether they
will acquire a mental illness:
Most people would probably think they're never going to have
a mental illness; so they would probably be comfortable about having mental
health as an exclusion. But yet we know...that mental illness is something that
can affect everybody of every age—mental illness is not something that people
like to talk about or people like to think about. But it is a serious illness
and we want to make sure that if people have private health insurance they are
covered for it because, as I said, it's not like orthopaedics or obstetrics,
which have quite different incidents over time. But it's something that can
affect everybody.[102]
2.68
However, the Department clarified that the government recently decided
not to include comprehensive psychiatric care in basic policies because it
would have a dramatic impact on premiums:
...if you look at the range of basic products that are out
there in the market at the moment, and they generally cover those three things
that they must cover and then they cover a range of minor surgery...the question
then becomes: 'Okay, so what would you want to add to those products to make
them more comprehensive?' And this is where the candidate that is often
mentioned is one that is providing full cover for psychiatric care rather than
restricted cover. As soon as you do that, several things happen. One of them is
that all the people who are buying top cover at the moment so that they get
access to psychiatric care and who don't want to get anything else much drop
out of top cover and move down. As soon as you do that, the extra benefits that
have to be paid out of that basic cover go up and that makes premiums go up by
15 per cent. Once that became clear and the advice was provided to the
government around this, the government decided that it didn't wish to pursue
expanding the scope of those basic things.[103]
Committee view
2.69
The committee recognises that consumers are currently confused by the
large number of private health insurance policies that are on offer and that it
can be difficult for consumers to understand what they are covered for. The
committee also understands that rising premiums, exclusions and out-of-pocket
costs are diminishing the value of private health insurance for consumers.
2.70
Whilst a certain onus must be placed on the consumer to understand their
level of coverage and the exclusions in their private health insurance policy, the
committee is concerned about the rising level of exclusions in private health
insurance policies. The committee also considers that consumers who pay for
private health coverage should not face unexpected out-of-pocket payments.
2.71
The committee is concerned about reports of individuals using their
superannuation savings or mortgaging a house to pay out-of-pocket medical costs.
The committee notes the government's announcement relating to accommodation and
travel costs for people in rural and regional areas. The committee's conclusion
on this announcement is contained in Chapter 5.
2.72
The committee believes that private health insurers should be more
transparent about the scope of coverage of their private health insurance
policies.
2.73
The committee recognises there are pressures that are placed on private
health insurers in setting premiums. Premiums are examined in the next chapter.
Navigation: Previous Page | Contents | Next Page