Introduction
1.1
One in five Australians will experience mental illness in any given
year, no matter where in Australia they live.[1] Over a lifetime, almost half of all Australians will experience a mental
illness.[2]
1.2
However, Australians living in rural and remote communities are less
likely to seek mental health treatment than their city dwelling counterparts.
1.3
In 2016–17, people living in remote areas accessed Medicare-subsidised
mental health services at a rate of three times less than people living in
major cities. In very remote areas the rate of access decreased even further,
with people accessing services at a rate of six times less than in major cities.[3]
1.4
The reduced access to mental health services is reflected in the high
rate of suicide in rural and remote communities. In 2016, 47 per cent of all
suicides occurred outside capital cities, even though these areas account for
only 32 per cent of Australia's total population.[4]
1.5
The Royal Flying Doctor Service (RFDS) released a major report in March
2017 which sparked a national conversation about the state of mental health in
remote and rural communities.[5]
1.6 Mental Health in Remote and Rural Communities[6] described how even though Australians living in rural and remote areas are
impacted by mental disorders at the same rate as people living in major cities,
they experience unique barriers to receiving care.[7] The report outlined data about the mental health services provided by the RFDS,
including mental health and social and emotional wellbeing programs and
aeromedical retrievals, in order to describe the impact of mental disorders on
rural and remote Australians receiving those services.[8]
1.7
In January 2018, the Chief Executive Officers of the RFDS, Dr Martin
Laverty, and of Mental Health Australia, Mr Frank Quinlan, expressed the view
that a lack of coordination and funding in the sector had led to rural and
remote patients missing out on services. Dr Laverty described the low rate of
people accessing mental health services in rural and remote areas as a crisis.[9] In response to this, the Minister for Health, the Hon. Greg Hunt MP, stated
that he believed there to be a 'very significant challenge' for mental health
services in regional areas.[10]
1.8
In March 2018, the Senate referred an inquiry into the accessibility and
quality of mental health services in rural and remote Australia to the Senate
Community Affairs References Committee (committee).[11] The terms of reference for the committee's inquiry are outlined below:
-
the nature and underlying causes of rural and remote Australians
accessing mental health services at a much lower rate;
- the higher rate of suicide in rural and remote Australia;
- the nature of the mental health workforce;
- the challenges of delivering mental health services in the regions;
- attitudes towards mental health services;
- opportunities that technology presents for improved service delivery;
and
- any other related matters.[12]
Defining rural and remote
1.9
There are a number of classifications used by government health programs
which seek to measure the remoteness of a particular community, such as the
Australian Bureau of Statistics (ABS) Remoteness Areas, the Modified Monash
Model (MMM) and the Accessibility and Remoteness Index of Australia (ARIA). A
'remoteness classification' refers to a set of geographic boundaries that
define the areas contained within them and assigns them to a specific
remoteness category.
1.10
Each of these remoteness classifications rely on data from the ABS and
information collected during the five-yearly Census of Population and Housing.
Effectively, each classification uses the distance from an urban centre as an
indicator of whether an individual may or may not have access to particular
services.
1.11
For example, the ABS Remoteness Areas classifies each area in Australia as:
- Major City;
- Inner Regional;
- Outer Regional;
- Remote; or
- Very Remote.[13]
Figure 1.1—Map of
the 2016 ABS Remoteness Areas
Source: ABS.[14]
1.12
Remoteness classifications are used in a wide variety of settings, such
as to determine a person's eligibility for telehealth, identify areas with a
workforce shortage or to analyse statistical data.
1.13
The committee has not chosen to limit itself to one particular
remoteness classification or to strictly enforce these definitions in the
course of its inquiry. This report refers to particular remoteness
classifications where relevant, and uses the term 'rural and remote' to refer
generally to regional and remote communities.
1.14
The committee held public hearings in a number of locations which may be
considered a regional town. This was in recognition of the fact that often
mental health services for residents of rural and remote areas are located in
regional hubs which have the population to sustain the services. These regional
hubs can also act as a base for outreach services to smaller rural and remote
communities.
Prevalence of mental illness and suicide in rural and remote Australia
1.15
Mental health is defined as 'a state of emotional and social wellbeing
where the individual can cope with the normal stresses of life and achieve
their life potential. It includes being able to work productively and
contribute to community life'.[15]
1.16
Mental illness refers to a clinically diagnosable disorder which affects
a person's cognitive, emotional and social abilities, and interferes with the
lives and productivity of people.[16] Mental illness covers a spectrum of disorders that vary in severity and
duration and include disorders such as anxiety, depression and addiction.[17]
1.17
The most recent National Survey of Mental Health and Wellbeing was
conducted in 2007. The survey found that approximately 45 percent of
Australians aged 16–85 years will experience a diagnosable mental illness in
their lifetime.[18] The survey also found that the prevalence of mental illness outside capital
cities and major urban areas was marginally lower than in capital cities.[19]
1.18
However, the same cannot be said for the prevalence of suicide in
Australia's rural and remote communities. As remoteness increases, so too does
the rate of suicide.
Figure 1.2—Percentage of avoidable deaths from suicide and
self-inflicted injuries (persons aged 0–74 years), 2010–2014
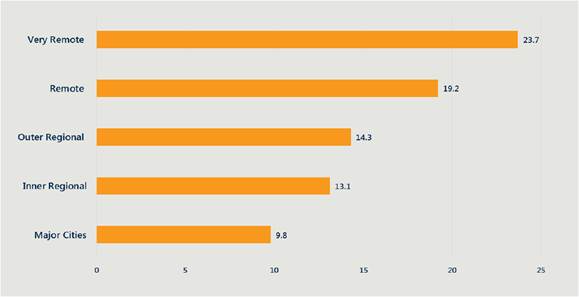
Source: Department of
Health.[20]
1.19
As shown above, between 2010 and 2017, the rate of suicide in remote areas
was almost double that of major cities, while the rate in very remote regions
was almost 2.5 times that of major cities.
1.20
The high rate of suicide in rural and remote communities is in part
driven by the increased rate of suicide amongst Aboriginal and Torres Strait
Islander peoples.[21]
1.21
Statistics show that Aboriginal and Torres Strait Islander peoples are
1.2 times as likely to die from mental illness as non-Indigenous Australians
and 1.7 times as likely to be hospitalised for mental illness. Furthermore,
Aboriginal and Torres Strait Islander peoples aged 12–24 years are three times
as likely to be hospitalised with a mental illness as non-Indigenous young
persons of the same age.[22]
1.22
While the prevalence of mental illness does not differ across Australia,
the impact of mental illness is far greater in rural and remote communities.
Living in rural and remote communities
1.23
Approximately 10 per cent of Australia's population, or 2.6 million
people, live in outer regional, remote and very remote areas.[23]
1.24
While people living in rural areas report high levels of civic
participation, social cohesion, social capital, volunteering and informal
support from friends, neighbours and the community, they experience unique
circumstances such as flood, fire, drought, as well as economic variability and
population downturn, which can impact on their health and wellbeing.[24]
1.25
Residents of rural and remote communities face a unique combination of factors
which are believed to contribute to low rates of access to mental health
services and the high rate of suicide. These include poor access to primary and
acute health care, social and geographical isolation, limited mental health
services, funding restrictions, ongoing stigma surrounding mental illness and
the cost of travelling to and accessing mental health services.[25] In addition, Aboriginal and Torres Strait Islander peoples face cultural
barriers and a lack of mental health services which are culturally appropriate.[26]
1.26
The barriers which impact upon the availability and accessibility of
mental health services in rural and remote communities will be explored further
throughout this report.
Aboriginal and Torres Strait
Islander communities
1.27
Aboriginal and Torres Strait Islander peoples are more likely to live in
rural and remote communities with approximately 20 per cent of all Aboriginal
and Torres Strait Islander peoples living in remote or very remote areas,
compared to only 1.7 percent of non-Indigenous Australians.[27]
1.28
Aboriginal and Torres Strait Islander peoples make up approximately
three per cent of Australia's population but continue to be disproportionately
represented on almost every indicator of social, health and wellbeing outcomes.[28]
1.29
Social determinants of health and historical factors such as
intergenerational trauma, racism, social exclusion, and loss of land and
culture are commonly recognised as factors which contribute to these ongoing
disparities in health care.[29]
1.30
The level of psychological distress for Aboriginal and Torres Strait
Islander peoples over 18 years old is nearly three times the rate of
non-Indigenous people across Australia.[30]
1.31
The alarmingly high rate of suicide amongst Aboriginal and Torres Strait
Islander peoples has led to the development of a number of state and national
strategies which seek to address the over representation of Indigenous
Australians in the mental health system as a priority.[31]
National framework for mental health
1.32
Mental health services, like most other health services in Australia,
are funded through a combination of federal, state and territory, and private
health insurance spending and delivered by a combination of public, private and
non-government sector providers.
1.33
Public mental health services include psychiatric hospitals, psychiatric
units in general hospitals, community residential units and community mental
health services, which are funded by both the Commonwealth and state and
territory governments.[32]
1.34
At a federal level, the Commonwealth Government has established 31 Primary
Health Networks (PHNs) which are responsible for the coordination and
commissioning of health care, including mental health services, in their local
areas.[33] PHNs are expected to work with state and territory Local Hospital Networks to
ensure that the national approach to mental health service delivery is
effective at the local level.[34]
1.35
Mental health services are provided in the private sector by private
psychiatrists, general practitioners, private psychiatric hospitals and private
allied health professionals. However, the Commonwealth Government also
contributes to these services through Medicare Benefits Schedule rebates and
private health insurance rebates.[35]
1.36
Non-government organisations include not-for-profit and community
managed organisations, which promote independence and mental wellbeing, provide
support and advocacy, or provide specialised information, accommodation and
rehabilitation services.[36]
Fifth National Mental Health and
Suicide Prevention Plan
1.37
In 2014, the National Mental Health Commission conducted a review into mental
health services and programs across Australia. The review found that
Australia's mental health system was poorly planned, fragmented, badly
integrated and lacked accountability.[37]
1.38
In response, the Council of Australian Governments (COAG) released the Fifth
National Mental Health and Suicide Prevention Plan (Fifth National Plan) in
August 2017. The Fifth National Plan aims to achieve reform and improved
outcomes in eight identified priority areas:
- Priority Area 1: Achieving integrated regional planning and
service delivery;
- Priority Area 2: Suicide prevention;
- Priority Area 3: Coordinating treatment and supports for people
with severe and complex mental illness;
- Priority Area 4: Improving Aboriginal and Torres Strait Islander
mental health and suicide prevention;
- Priority Area 5: Improving the physical health of people living
with mental illness and reducing early mortality;
- Priority Area 6: Reducing stigma and discrimination;
- Priority Area 7: Making safety and quality central to mental
health service delivery; and
- Priority Area 8: Ensuring that the enablers of effective system
performance and system improvement are in place.[38]
1.39
Notably the Fifth National Plan is the first national mental health
strategy to include a national suicide prevention plan.[39] Under the suicide prevention priority area, governments will establish a new
Suicide Prevention Subcommittee which will develop a National Suicide
Prevention Implementation Strategy.[40]
1.40
The National Suicide Prevention Implementation Strategy will include a
focus on Aboriginal and Torres Strait Islander suicide prevention and a draft
version of the strategy is expected to be released in mid-2019 for public
consultation, prior to release of the final strategy by 2020.[41]
1.41
The Fifth National Plan committed all governments to work together to
achieve integration in the planning and delivery of mental health services and
placed consumers and carers at the centre of how services are planned,
delivered and evaluated.[42]
Overview of state government services and strategies
1.42
State and territory governments provide funding for public sector and
community services and set legislative, regulatory and policy frameworks for
mental health service delivery within their jurisdiction.[43]
1.43
The main government bodies delivering mental health services to rural
and remote areas in each state and territory and the key strategies for mental
health in these areas are outlined below.
Western Australia
1.44
Public mental health services in rural and remote Western Australia (WA)
are delivered by the WA Country Health Service, part of the WA Department of
Health. Health services are organised by a hub and spoke model, with services
based in larger regional and metropolitan centres, and specific rural services
funded to address locational disadvantage.[44]
1.45
The WA Mental Health Commission is responsible for commissioning of
state-government funded mental health services from government and
non-government providers, and also provides and has responsibility for
commissioning mental health, alcohol and other drug prevention and health
promotion programs. Investment has been directed to the implementation of a comprehensive
suicide prevention program (Suicide Prevention 2020), public education
campaign initiatives, and the expansion of community-based bed and treatment
services.
1.46
Mental health services in WA are guided by the Western Australian
Mental Health, Alcohol and Other Drug Services Plan 2015–2025.[45]
1.47
The committee held five public hearings in WA, in recognition of the
vast rurality of the state and high number of remote communities. WA
encompasses 32 per cent of Australia's remote communities and 31 per cent
of very remote communities.[46]
1.48
The committee held its first public hearing in the south-west regional
town of Albany on 5 June 2018. The committee held its next four public hearings
across the remote Kimberley region in northern WA, visiting Kununurra and Halls
Creek on 5 July 2018 and Derby and Broome on 6 July 2018.
Northern Territory
1.49
The Northern Territory (NT) makes up approximately 18 per cent of
Australia's land mass, but only one per cent of the total national population.
Approximately 33 per cent of the NT population live in areas considered remote
or very remote.[47]
1.50
Public health services in the NT, including mental health services, are
delivered by the Top End Health Service (Darwin metropolitan and the northern
part of the territory) and the Central Australia Health Service (Alice Springs
and the southern part of the territory).[48]
1.51
Key strategies relating to mental health services and suicide prevention
in the NT include the Northern Territory Suicide Prevention Strategic
Framework 2018–2023, which was recently launched in September 2018,
the Northern Territory Mental Health Strategic Plan 2015–2021 and the Northern
Territory Health Aboriginal Cultural Security Framework 2016–2026.
1.52
Provision of funding to non-government organisations is managed by the
Mental Health Alcohol and Other Drugs Branch of the NT Department of Health.[49] This funding supports services such as subacute care, mental health promotion,
support and advocacy, primarily in Darwin and Alice Springs, with a small
number of providers in Katherine and Tennant Creek.[50]
1.53
The committee held three public hearings in the NT: two on 9 July
2018 in Darwin and Katherine and a further hearing in Alice Springs on 10 July
2018.
South Australia
1.54
SA Health provides mental health services for South Australians through
community health centres, public hospitals and in-home care.[51] SA Health is also responsible for implementation of the South Australian
Suicide Prevention Plan 2017–2021.[52]
1.55
The South Australian Mental Health Commission was established in 2015 to
strengthen mental health and wellbeing in the state.[53] Subsequently, the commission released the SA Mental Health Strategic Plan
2017–2022 which recognised the need to target support for rural and remote
communities.[54]
1.56
The committee held one public hearing in South Australia in Whyalla on 20 July
2018.
Queensland
1.57
Approximately 33 per cent of Queensland's 5 million residents live in
rural and remote areas, with 95 per cent of Queensland's land mass classified
as rural or remote.[55]
1.58
The committee held two public hearings in Queensland: Mount Isa on
29 August 2018 and Townsville on 30 August 2018.
1.59
The Queensland Department of Health (Queensland Health) is responsible
for the overall management of public health in the state. Public health
services, including mental health services, are provided through service
agreements with 16 independent Hospital and Health Services, each governed by
its own board and chief executive.[56] Queensland Health also commissions non-government organisations to provide
mental health services.
1.60
The Queensland Mental Health Commission was established in 2013 to
provide ongoing reform towards an integrated, evidence-based, recovery-oriented
mental health and substance misuse system.[57] The commission is responsible for preparing, monitoring, reporting and
reviewing the Queensland Mental Health, Drug and Alcohol Strategic Plan
2014–2019.[58] In 2016, the Queensland Government and the Queensland Mental Health Commission
released the Queensland Rural and Remote Mental Health and Wellbeing Action
Plan 2016–18.
New South Wales
1.61
New South Wales (NSW) Health is the provider of public hospital and
health services in NSW, including specialist mental health services. NSW Health
operates seven rural and regional local health districts, each of which has 'the
flexibility to tailor services where most needed and using methods most
appropriate to their communities'.[59] Two specialty networks, Justice Health and Forensic Mental Health Network and
Sydney Children's Hospitals Network, also provide specialist mental health
services to rural and remote areas.[60]
1.62
The NSW Ministry of Health Mental Health Branch funds non-government
organisations to deliver treatment, psychosocial rehabilitation and
recovery/disability support programs. It also invests in the Centre for Rural
and Remote Mental Health to support the mental health of rural and regional
residents through research and evidence-based service design, delivery and
education.[61]
1.63
The Mental Health Commission of NSW is an independent statutory agency
responsible for monitoring, reviewing and improving mental health and wellbeing
for people in NSW.[62] The Mental Health Commission developed Living Well: A Strategic Plan for
Mental Health in NSW 2014–2024, which was adopted by the NSW Government and
informed the development of a new strategic framework for mental health in the
state.[63]
1.64
The NSW Strategic Framework and Workforce Plan for Mental Health
2018–2022 was released in September 2018.[64] Other relevant key plans and strategies for mental health and rural health more
broadly include the NSW Rural Health Plan Towards 2021 and the NSW
Aboriginal Health Plan 2013–2023.[65]
Victoria
1.65
The Victorian Government Department of Health and Human services is
responsible for mental health care in the state of Victoria. The Victorian
Government funds a range of primary, community-based and hospital mental health
services.[66]
1.66
The Mental Health Complaints Commission is an independent, specialist
body established to resolve complaints about Victorian public mental health
services, safeguard patient's rights and recommend improvements to services.[67]
1.67
In November 2015, the Victorian Government launched Victoria's
10-year mental health plan, outlining the government's long term strategy
to improve mental health outcomes for Victorians with a mental illness, their
families and carers.[68]
1.68
Major strategies developed under the plan include the Victorian
suicide prevention framework 2016–25, the Mental Health Workforce
Strategy, and the Aboriginal Social and Emotional Wellbeing Framework.
Tasmania
1.69
The Mental Health, Alcohol and Drug Directorate, within the Tasmanian
Department of Health and Human Services, is responsible for the provision of
mental health services throughout the state.[69]
1.70
Statewide Mental Health Services is the provider of care for people with
a severe mental illness in inpatient facilities and in the community. In
addition, Mental Health Services works with the community sector to provide
support to people with a moderate to severe mental illness.[70]
1.71
In October 2015, the then Minister for Health launched the Rethink
Mental Health Better Mental Health and Wellbeing – A Long-Term Plan for Mental
Health in Tasmania 2015–25 which identified a reform agenda to improve the
mental health of Tasmanians and priority action areas.[71]
1.72
Approximately 40 per cent of Tasmanian's live outside of Hobart and Launceston
in areas classified as outer regional, remote and very remote.[72]
1.73
The committee held two public hearings in Tasmania: one in the
north-west town of Devonport on 5 September 2018 and one on the east coast in
St Helens on 6 September 2018.
Australian Capital Territory
1.74
ACT Health provides mental health services in hospital and community
settings for residents of the Canberra region.[73] However, the committee did not receive any evidence relating to the accessibility
of mental health services in the Canberra region.
1.75
The committee held three public hearings in Canberra on 19 July 2018,
18 September 2018 and 16 October 2018 to hear from peak representative
bodies of the mental health sector, non-government organisations, academics,
and relevant Commonwealth government departments.
Structure of the report
1.76
This report is presented in six chapters:
- This first chapter provides background and context to the
committee's inquiry.
- Chapter 2 outlines mental health services funding and provision
in Australia, the model of practice on which these services are based and
commissioned, and examines opportunities to utilise technology in the provision
of mental health services.
- Chapter 3 explains the numerous barriers people in rural and
remote areas face when accessing mental health services, including attitudes
towards mental health.
- Chapter 4 considers the role and impact of culturally appropriate
services on Aboriginal and Torres Strait Islander peoples.
- Chapter 5 outlines the issues facing the mental health workforce
and how these issues are intensified in rural and remote communities.
- Chapter 6 provides the committee's conclusions and
recommendations.
Conduct of the inquiry
1.77
On 19 March 2018, the Senate referred the inquiry into the accessibility
and quality of mental health services in rural and remote Australia to the
committee for inquiry and report by 17 October 2018.[74] The Senate subsequently granted the committee extensions of time to report
until 4 December 2018.[75]
1.78
The committee advertised the inquiry on its website and wrote to
relevant individuals and organisations inviting submissions by 11 May 2018. The
committee continued to accept submissions after that date.
1.79
The committee received 138 submissions. A list of submissions received
by the committee is available at Appendix 1 and copies of public submissions
can be accessed via the committee's website.
1.80
During the inquiry, the committee travelled across Australia to hear
from state government bodies, mental health service providers, academics, peak
representative organisations, local PHNs and community members about the
quality and accessibility of mental health services in rural and remote areas.
1.81
In total, the committee held sixteen public hearings. A list of the witnesses
who appeared at each hearing is available at Appendix 2.
1.82
The committee also conducted two site visits in the course of its
inquiry. The committee visited the West Kimberley Regional Prison in Derby on 6
July 2018 and the Barkly Work Camp in Tennant Creek on 10 July 2018. Reports
on the committee's sites visits are at Appendix 3.
Acknowledgements
1.83
The committee thanks all of the individuals and organisations who
submitted to the inquiry and appeared as witnesses.
1.84
The committee also thanks the WA Department of Justice and the NT
Department of the Attorney-General and Justice for facilitating the committee's
site visits. The committee extends its gratitude to the staff and prisoners of
the facilities who were generous with their time and willingness to discuss
their experience with mental health.
Notes on references
1.85
References in this report to Committee Hansard are to proof
transcripts. Page numbers may vary between the proof and official transcripts.
Navigation: Previous Page | Contents | Next Page