Funding and the Medicare Benefits Schedule
5.1
The Commonwealth Government funds diagnostic imaging services through
the Medicare Benefits Schedule (MBS) and the National Health Reform Agreement
(NHRA).[1]
5.2
The MBS is a Commonwealth Government funded subsidy scheme.[2] Under the MBS,
subsidised professional services are allocated an item number. At the point of
service delivery, if the conditions of the item number are met, the patient is
entitled to a rebate.
5.3
The NHRA was a health funding arrangement signed by the Commonwealth
Government and all state and territory governments in 2011.[3] The NHRA allows public
patients in public hospitals to have their diagnostic imaging provided to them
free of charge.[4]
5.4
This chapter will consider the challenges posed by attempting to provide
financial assistance to the largest number of patients with costly health
conditions against maintaining a sustainable system over the medium to long
term. In particular, this chapter will consider: the number of services that
are currently provided and the cost of providing those services; the benefits
and challenges of managing MBS indexation; items that are currently standard
practice but are not on the MBS; and the operation of special diagnostic
imaging provisions of the MBS.
Volume and cost of services
5.5
According to data provided by the Department, 394.3 million
services were funded under the MBS in 2016–17 at a total cost of $22 billion.[5]
Of this total, diagnostic imaging services accounted for 25.7 million services
(seven per cent) and $3.4 billion in benefits (16 per cent).[6] A visual
representation of these services and their cost appears in Figures 5.1 and 5.2.
Figure
5.1: Number of MBS services by category (millions) 2016–17
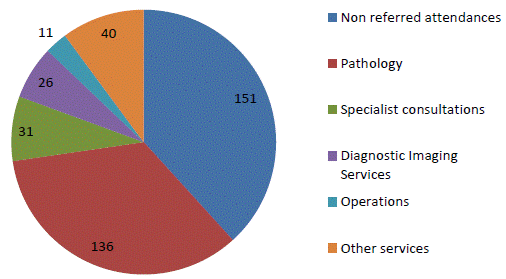
Source: Department, Submission
18, p. 17.
Figure
5.2: MBS benefits by category (billions) 2016–17
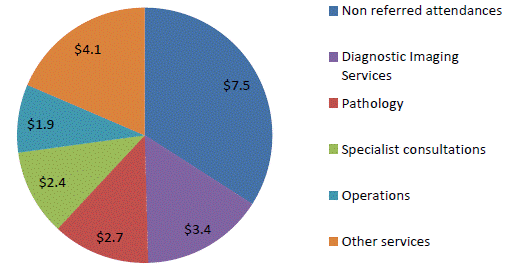
Source: Department, Submission
18, p. 17.
5.6
The funding for diagnostic imaging services is provided for by the Health
Insurance Act 1973 (Cth), and its associated regulations, the Health Insurance
Regulations 1975 and the Health Insurance (Diagnostic Imaging Services Table)
Regulation 2017 (DIST).[7]
The Health Insurance Act 1973 and the DIST provide for 'the conditions
under which Medicare benefits are payable'.[8]
Re-indexation of diagnostic imaging
services
5.7
Whilst the diagnostic imaging component of the MBS is substantial, the
cost to the MBS has been constrained by freezing the schedule fee for
diagnostic imaging services.
5.8
Prior to 1998, decisions about MBS fee increases were made annually.[9]
Between 1 July 1998 and 30 June 2008, diagnostic imaging expenditure was
managed under Memoranda of Understanding (MoU) between the Commonwealth
Government and the diagnostic imaging sector.[10]
In April 2008, the government announced that the MoUs would be discontinued and
'MBS fees applicable at that time would apply'.[11]
5.9
The MBS schedule fee for diagnostic imaging services has remained the
same since 2007.[12]
Table 5.1 lists the dates of the last schedule fee increase for diagnostic
imaging services.
Table
5.1: Dates of last schedule fee increase for diagnostic imaging services
| Group |
Date of last schedule fee
increase |
| Ultrasound (except cardiac) |
1 November 2004 |
| Ultrasound—Cardiac |
1 November 2007 |
| CT |
1 November 2004 |
| Diagnostic radiology |
1 November 2004 |
| Nuclear medicine imaging |
1 November 2006 |
| MRI |
1 July 2006 |
Source: Department, Submission
18, p. 21.
5.10
Professor Mark Khangure from the Australian Medical Association told the
committee that the failure of MBS benefits to keep up with real costs means
that practices have had to continually absorb costs or pass the costs on to
patients:
Indexation for general practice items is a few years;
indexation, or loss of, for imaging is virtually two decades. The total cost of
equipment, of staff salaries, of running the practice itself, has gone up, with
CPI [Consumer Price Index] alone well above, so there's a point in time where
the practice either folds up or it actually has to just say up-front to the
patients: 'I'm sorry. You have to pay.'[13]
5.11
The WA Country Health Service also explained that current MBS revenue
was not sufficient to cover the cost of public imaging services in rural
Western Australia:
MBS rebates are a gross underrepresentation of the costs
associated with providing an imaging service—particularly in regional areas,
where costs are significantly higher. Almost every externally referred patient
presenting for imaging in WA Country Health Service's imaging department costs
the health service a sum of money, even after MBS revenue.[14]
5.12
In the 2017–18 Budget, the Commonwealth Government announced that some
diagnostic imaging services would be re-indexed from 1 July 2020.[15]
The Department advised the committee that this limited re-indexation would cost
$20.6 million in 2020 and would increase diagnostic imaging expenditure by
$700 million over ten years.[16]
The committee heard from the Australian Diagnostic Imaging Association (ADIA) that
the Government's 2016 election commitment to ensure that diagnostic imaging
indexation resumes when the current GP rebate indexation freeze concludes is
yet to be implemented.[17]
5.13
During 2016–17, patients claimed the following diagnostic imaging
services as detailed in Figure 5.3.
Figure
5.3—Percentage MBS services by modality 2016–17
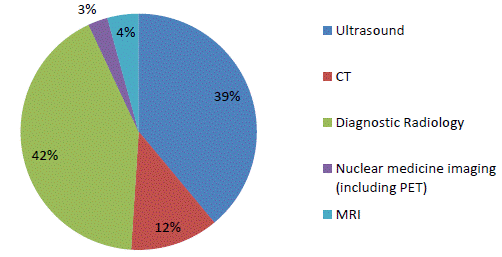
Source: Department, Submission
18, p. 5.
5.14
The Commonwealth Government paid over $3.4 billion in patient rebates
during the 2016–17 financial year.[18]
Thirty-three per cent of this $3.4 billion was provided as ultrasound rebates,
followed by 29 per cent for CT, 17 per cent for diagnostic radiology, 13 per
cent for MRI and eight per cent for nuclear medicine imaging.[19] A visual representation
is included below in Figure 5.4.
Figure
5.4—Percentage MBS benefits by modality 2016–17
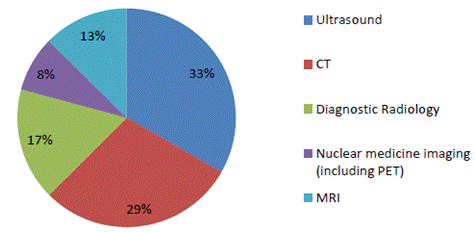
Source: Department, Submission
18, p. 18.
5.15
The Department has also identified that demand for diagnostic imaging
services and the benefits paid (per capita) have grown in line with other MBS
funded services.[20]
Compounded annual growth has increased by three per cent for services and by
five per cent for benefits paid.[21]
Bulk billing for diagnostic imaging
services
5.16
The rates of bulk billing for diagnostic imaging services differ
depending on whether it is an out-of-hospital service or a service provided by,
or on behalf of, a general practitioner (GP).[22]
For out-of-hospital diagnostic imaging services, the general Medicare rate is
85 per cent of the MBS fee.[23]
For GP services, the Medicare benefit is 100 per cent of the MBS fee.[24]
5.17
In 2016–17, 84 per cent of diagnostic services provided out of hospital
were bulked billed. The Department submitted that the 'average out-of-pocket
costs for out-of-hospital non bulk billed diagnostic imaging services in 2016-17
was just over $97'[25]
and '[o]ut-of-pocket costs have grown at an average annualised rate of four
percent since 2004'.[26]
The Department noted that this increase exceeded the average consumer
price index increase of three per cent per annum.[27]
5.18
Seventy eight per cent of services claimed under the MBS in 2016–17 were
provided by private specialist radiology practices, followed by public
facilities (13 per cent), and other practices (10 per cent).[28]
Figure
5.5—Percentage of MBS services claimed by practice type 2004–05 to 2015–16
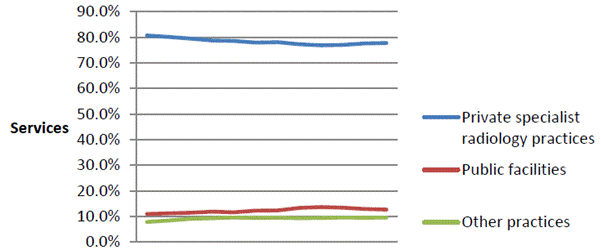
Source: Department, Submission
18, p. 34.
Standard items not included on MBS
5.19
Throughout the inquiry, submitters raised concerns that the number of
diagnostic imaging tests listed on the MBS was too limited and did not include
a number of tests which are now considered as standard.[29]
5.20
Items are only added to the MBS on the advice of the Medical Services
Advisory Committee (MSAC). MSAC is an independent non-statutory committee
largely made up of clinicians and academics to advise the Minister for Health
about the MBS.[30]
According to the Department, MSAC assesses new technologies for comparative
safety, clinical effectiveness and cost effectiveness.[31]
5.21
Breast Cancer Network Australia (BCNA) highlighted that, despite an MRI
being required to confirm a breast cancer diagnosis, no MRI is currently
available for many women.[32]
Ms Spence from BCNA explained to the committee that a failure to rebate breast
MRI caused a significant financial impost on those women:
We know they're paying anywhere from $500 to $1,500 out of
pocket for that procedure. The fact that there's no rebate really does add to the
fact that it's variable depending on where you're referred to.[33]
5.22
Prostate Cancer Foundation Australia expressed similar concerns for men
who require multiparametric MRI or PET scanning. Associate Professor Anthony Lowe
from Prostate Cancer Foundation Australia explained that multiparametric MRI is
required for improved diagnostic accuracy and to prevent unnecessary prostate
biopsies.[34]
PET scanning also allows the specialist to tell if a cancer is recurring.[35]
Associate Professor Lowe explained to the committee how PSMA PET scanning works:
The technique uses a radioactive tracer to attach to the
cancer cell, and then it can be imaged in a PET CT scanner. As people say, it
lights up the Christmas tree when you have cancer. You can see exactly where
the cancer is. It's particularly important for men who've had primary
treatment, whose PSAs reduce to an undetectable level so they feel they've been
cured... After a number of years—possibly 10 years—their PSA starts to rise
again, so we know that the cancer is recurring.[36]
5.23
However, these scans are not currently rebated on the MBS. Associate
Professor Lowe explained that men who require scans to manage their prostate
cancer can incur significant out-of-pocket costs:
On average, they are in the order of $5,000 to $10,000 for a
man over the treatment period but there is currently no Medicare rebate either
for multiparametric MRI or for the PET scanning so men are out of pocket in the
order of $500 to $600 per scan.[37]
5.24
Associate Professor Lowe and Ms Spence agreed that the cost of essential
diagnostic imaging services not included on the MBS places additional financial
stress on patients already suffering from a cancer diagnosis.[38]
An individual told Rare Cancers Australia that 'it is embarrassing and
stressful when you can't afford these things which your specialist teams need
in order to help you.'[39]
5.25
As noted in chapter two, the limited assistance patient transport
schemes provide is often not available if the procedure they are being
transported for does not have an MBS item number attached to it.[40]
Depending upon the person, whether the item is rebated or not may be the
difference between the patient being able to have the scan or not.
5.26
Associate Professor Lowe told the committee that patients are often
confused about why these essential tests do not attract an MBS rebate:
And that probably is the biggest inquiry we receive from men
in our national office. They ask: why is it not rebated? Why do I have to pay
this when my clinician is telling me it is essential for me to have this scan
in order for them to be able to manage the situation?[41]
Adding new items to the MBS
5.27
The committee heard from the Urological Society of Australia and New
Zealand (Urological Society) and BCNA that they have tried to have these scans
added to the MBS.[42]
5.28
As noted above, new items are only added to the MBS on the advice of
MSAC. Dr Peter Heathcote, President of the Urological Society told the
committee that it had been seeking a rebate for multiparametric MRI for
prostate cancer diagnosis and management for the past three and a half years
and would soon be pursuing an application for the PSMA PET scanning.[43]
5.29
Similarly, BCNA told the committee that it had pursued a number of
applications for breast MRI and genomic testing.[44]
The genomic test, Oncotype DX, could have been prescribed to help an oncologist
ascertain whether chemotherapy will help the patient. However, BCNA advised the
committee that the application was unsuccessful:
...the MSAC decision, unfortunately, didn't approve Oncotype
DX, even though it's standard care in most developed countries around the
world. So, for women, if they want to access a genomic test it's $4,500.[45]
5.30
BCNA explained that it had taken MSAC so long to process the application
that the MSAC preferred (and cheaper) solution was no longer available:
Interestingly, the online tool that was cited... It's not
available at the moment because everywhere around the world people are using
Oncotype DX. So the test that MSAC referred to, where people can use this
online algorithm, is not being used by oncologists at the moment because it's
not available.[46]
5.31
Other submitters agreed that the application process and approval of new
items on the MBS by MSAC was too slow.[47]
5.32
The Royal Australian and New Zealand College of Radiologists (RANZCR)
told the committee that there were a number of useful scans that were still
making their way through the MSAC process:
...there are several areas of the body for which imaging under
MRI are very useful. They're not listed yet on the MBS and have been chugging
very slowly through the MSAC process. Examples of that are cardiac MRI, liver MRI,
breast MRI and prostate MRI...[48]
5.33
Submitters were sometimes unsure about why the approval had taken so
long or why their application was refused.[49]
Submitters highlighted that clinical best practice was evolving much faster
than MSAC was able to consider the applications brought to it.[50]
Ms Spence told the committee that MSAC's process need to be compressed:
I think we need to find a way to keep MSAC up to date with
innovation because, by the time these rulings come out, often we've moved on to
something that's standard practice overseas and that we're just now making the
call on, and things have happened in between. As a consumer based organisation,
we don't know whether that new evidence is part of the decision-making or
whether it's just on the dossier that was presented in the beginning of that
process, so it's hard to have that transparency around what influenced that
decision. Was it just what was put forward three years ago, or is it taking
into account the new evidence that's available?[51]
5.34
The Department told the committee that MSAC would next consider the
applications for multiparametric MRI for prostate cancer, breast MRI, obstetric
MRI and other diagnostic imaging applications at upcoming meetings in March and
July 2018.[52]
Reviewing items currently on the
MBS
5.35
In order to align clinical practice with the MBS, the MBS Review
Taskforce is currently conducting a review of all 5700 items on the MBS.[53]
5.36
Since its establishment in 2015, the MBS Review Taskforce has provided the
Minister for Health with a report on obsolete MBS items and two subsequent
tranches of recommendations relating to diagnostic imaging: one into lower back
pain and one into bone densitometry.[54]
5.37
The obsolete items report identified five MBS items for removal on the
basis that their use did not accord with clinical best practice; recommended limiting
the use of one item to a smaller clinical population and recommended further
consideration of a seventh item.[55]
Subsequent reports made four recommendations in relation to imaging for lower
back pain and five recommendations in relation to unnecessary testing of bone
densitometry.[56]
5.38
The MBS Review Taskforce will continue its work into 2018 with a view to
examining co-claiming and capital sensitivity.[57]
Committee view
5.39
The committee understands that the government operates under fiscal constraints
and that there is a need for the MBS to be sustainable over time. It also
recognises that diagnostic imaging services currently account for a substantial
portion of the MBS budget.
5.40
The committee acknowledges that freezing indexation of the diagnostic
imaging service items on the MBS has required private providers and public
health services to either absorb the difference between the cost of the service
and the Medicare benefit, or pass costs on to patients.
5.41
The committee also acknowledges that, whilst it is a substantial
investment to list an item on the MBS, patients are being forced to incur large
out-of-pocket costs in order to have essential imaging services performed.
5.42
Whilst the committee understands that adding new items may be an
increase in public expenditure, the committee considers that patients should be
able to access medical services without placing themselves under significant
financial stress.
5.43
The committee also considers that it would be advantageous if the speed
of MSAC's processes could be increased to allow MSAC to consider all
applications with up-to-date scientific evidence.
5.44
The MBS Review Taskforce appears to be consulting with stakeholders and
completing its work diligently. The committee notes that the changes proposed
to date have been largely focused on the identification of obsolete items, and there
appears to be scope for broader review.
Other MBS funding
5.45
The Commonwealth Government uses the MBS to provide an economic
incentive for providers to upgrade their equipment. This is called the capital
sensitivity measure.
Capital sensitivity measure
5.46
The capital sensitivity measure aims to improve patient access to newer
and better quality diagnostic imaging equipment by reducing the MBS fee once
equipment reaches a certain age, thereby encouraging providers to upgrade or
replace older equipment.[58]
5.47
All diagnostic imaging services listed on the MBS (with the exception of
PET services) have two different MBS fees, schedule K items and schedule NK
items. A schedule K diagnostic imaging service can be claimed if the
service is performed on newer or upgraded equipment, whereas an NK schedule
item is claimed on older equipment with the MBS fee reducing by approximately
50 per cent.[59]
5.48
The Department noted that the number of NK schedule items claimed is
less than one per cent, indicating that the capital sensitivity measure is
effective at ensuring diagnostic imaging equipment in metropolitan areas is
upgraded.[60]
5.49
In accordance with the capital sensitivity measure, diagnostic imaging
equipment must be replaced after 10–15 years (new effective life age),
depending on the modality, or between 15 and 20 years (maximum extended life
age) if the equipment has been upgraded prior to reaching its new effective
life age.[61]
5.50
The Australian Society of Medical Imaging and Radiation Therapy (ASMIRT)
questioned the appropriateness of the life ages, noting that while the new
effective life age and maximum extended life ages may have been appropriate
previously, advancements in technology now occur at a much more rapid pace.[62]
5.51
ASMIRT submitted that diagnostic imaging equipment may now be obsolete
or superseded within only five to eight years, far sooner than the current new
effective life age.[63]
5.52
ASMIRT explained equipment should be upgraded more frequently because
older equipment could lead to worse health outcomes for patients:
An ultrasound scanner that is 10 years old is less able to
diagnose not only foetal abnormalities because the TV screen would have lost
its brilliance or resolution, (a bit like your TV at home) but the electronics
is so poor by today's standards the entire range of examination quality is
poor.[64]
5.53
RANZCR told the committee that it believed that the current measure was
adequate, but that it could be reviewed:
In terms of whether the times that have been set for CT,
angiography equipment and MRI are appropriate or not, I think they're
reasonable and cost achievable. Whether they should be less or not I think
should be looked at by committees. It requires funding by the payer,
essentially, which is the government, so that's a question that needs to be
addressed...[65]
Regional, rural and remote exemptions
5.54
Practices in outer regional, remote and very remote areas are
automatically exempt from the capital sensitivity measure and other inner
regional practices may apply for exemptions in certain circumstances to ensure
continued access to diagnostic imaging services in these locations, despite the
use of older equipment.[66]
5.55
However, RANZCR expressed concern about whether allowing older equipment
to be used in country areas was a disservice to regional, rural and remote
residents:
Basically the old machines are being shipped out to the
country. And I think you could argue that regional patients are being subjected
to imaging on older equipment, which may not be in their best interests. So I
think this should be reviewed. It may be inevitable, given the lower
utilisation of machines in regional areas, but it's a subject of personal
concern for me.[67]
5.56
The Department of Health Western Australia advised that diagnostic imaging
services in regional centres were often conducted on older models which provide
lower quality imaging services compared to technology available in Perth:
Where there are imaging services in regional WA, these do
tend to be older models—for example, in Esperance, Kalgoorlie, Broome and
Geraldton, where there is a 16-slice CT scanner. By contrast, Sir Charles
Gairdner Hospital has a 320-slice scanner, and the new Fiona Stanley Hospital
has two 256-slice scanners. The significance of this for the patient is that
the quality of the images may be lower, the dose of the radiation required may
be higher and the dose of the contrast agent that's required, which can have
risks in terms of renal failure, may be higher. The older machines may also
lend themselves less to hybrid technologies like CT/SPECT, necessitating trips
to Perth.[68]
5.57
Rural service providers made it clear to the committee that the regional,
rural and remote capital sensitivity exemptions were required to make imaging
services in those locations viable.[69]
The WA Country Health Service told the committee that if the rural capital
sensitivity exemption was removed, it may struggle to continue to provide the
same range of services:
The Commonwealth must maintain the current remoteness around
capital sensitivity exemptions for medical imaging in order to maximise the
availability of services to those regional patients. If removed, the costs
associated with providing imaging may further increase, making it more
expensive for [WA Country Health Service] due to more frequent equipment
replacement and possibly resulting in the removal of some imaging services due
to prohibitively expensive costs.[70]
5.58
Whilst equipment may only make up between 10 and 12 per cent of the cost
of imaging, it can be a very substantial cost for rural communities.[71]
Mr Aiden Cook from the Darling Downs Hospital and Health Service told the
committee that whilst upgrading rural equipment was required, some thought also
needed to be given to the cost required to do so:
We have a need to upgrade regional machinery as much as
anywhere, and it comes down to small hospitals and their ability to replace
machinery at $300,000 a pop. It's not easy. That's a lot of cakes that they
need to come up with in some of these small places.[72]
5.59
ADIA told the committee that the capital sensitivity arrangements were
being considered by the MBS Review Taskforce and may be the subject of an
upcoming recommendation.[73]
Section 19(2) exemptions
5.60
To support the availability of diagnostic imaging and defray the cost of
purchasing new equipment in rural areas, the Council of Australian Governments
introduced the Section 19(2) Exemptions Initiative to permit a list of rural
sites to claim Medicare benefits for non-admitted, non-referred professional
services (such as midwifery, nursing and dental services).[74]
5.61
Section 19(2) of the Health Insurance Act 1973 provides that
Medicare benefits are not payable where another payment is available to cover
the service.
5.62
The WA Country Health Service noted that the exemption permits hospitals
to retain Medicare benefits for providing professional services, including
diagnostic imaging services to ensure that imaging can continue in rural areas:
This [exemption] allows the health service provider to charge
Medicare for imaging procedures on patients referred through the hospital
system and not just externally through GPs. The 19(2) exemption significantly
improves the revenue stream to [WA Country Health Service] hospitals to ensure
that we can maintain these needed imaging services.[75]
5.63
In addition to helping maintain the existing imaging services, the
Darling Downs Hospital and Health Service noted that holding a section 19(2)
exemption assisted smaller hospitals to accumulate revenue to purchase or
upgrade its diagnostic imaging equipment:
...some of the smallish hospitals, particularly the 19(2)
exemption sites, have a need to maintain some revenue out of those privately
referred patients to enter the public hospital. The technology at the top end
is quite expensive. In the pool of money available to replace equipment across
Queensland, the pressure will come on to replace those high-value machines, and
the low-value machines in general X-ray will probably have longer and longer
life spans, and I think that a lot of these rural hospitals will start to run
into difficulty.[76]
5.64
Currently, 19(2) exemption sites are determined based on population and
geographic remoteness using the Modified Monash Model.[77]
5.65
The Queensland Nurses and Midwives' Union (QNMU) noted that two
Queensland hospitals (Roma and Mareeba) have recently lost their section 19(2)
exemptions.[78]
The QNMU was concerned because, in addition to the lost revenue stream, the
nurses and midwives operating the diagnostic imaging equipment in those
hospitals have lost their ability to independently claim Medicare rebates.[79]
5.66
The QNMU submitted that the loss of the exemption led to a reversion to less
innovative and efficient ways of working in the hospitals concerned.
5.67
The QNMU instead suggested that the social determinants of health or
some other measure should be considered when deciding which areas ought to be
eligible for section 19(2) exemptions to ensure that the overall number of
hospitals eligible for section 19(2) exemptions was not reduced.[80]
Committee view
5.68
The committee understands that medical technology evolves rapidly and
that newer equipment will provide patients with a better quality of care and
improved chance of accurate diagnosis. The committee considers that capital
sensitivity measures could be reviewed for metropolitan centres and understands
that this will be considered as part of the MBS Review.
5.69
While understanding the issues involved in regional, rural and remote
areas, the committee is concerned about the impact on patient health of the
current rural capital sensitivity exemptions and the section 19(2) exemptions
to assist with the cost of services and equipment. While the committee expects
that tighter capital sensitivity measures for metropolitan centres may permit
modern equipment to be deployed to rural areas more frequently and at lower
cost, the committee believes there needs to be consideration given to the
possible poorer health outcomes of regional, rural and remote patients.
Navigation: Previous Page | Contents | Next Page