Availability and accessibility of diagnostic imaging
Introduction
2.1
The availability and accessibility of diagnostic imaging was a central
concern in this inquiry. This chapter will focus on the current distribution of
the following diagnostic imaging machines across Australia and issues relating
to access to them:
-
ultrasound;
-
computed tomography (CT);
-
diagnostic radiology (such as x-ray and mammography) and
-
nuclear medicine imaging, including positron emission tomography
(PET).
2.2
Specific issues relating to the use of and accessibility of Magnetic
Resonance Imaging (MRI) equipment is considered separately in chapter three of
this report.
Distribution
2.3
The distribution of diagnostic imaging machines around Australia is
determined by private providers, based on commercial considerations, and by the
state and territory governments that provide public health services.[1]
2.4
The Department of Health (Department) advised the committee that one
method to consider whether Australia has enough diagnostic imaging machines is
to consider how many machines Australia has per capita relative to other
developed countries. The Organisation for Economic Co-operation and Development
(OECD) collects data on the availability of CT and MRI machines in each
country.
2.5
In 2015, Australia ranked 11th in its availability of CT
equipment per million people compared to other OECD countries.[2]
Between 2013 and 2015, Australia increased its availability of CT equipment
from 53.7 per million to 59.6 per million. The table below shows a
comparison between the top ranking OECD countries and the number of CT machines
per million people from 1998 to 2015.
Table 2.1: CT equipment per million population OECD
countries, 1998–2015
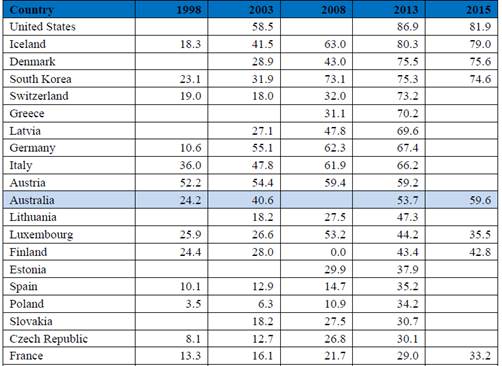
Source: Department, Submission
18, p. 35.
2.6
The Department submitted that there are no international benchmarks for
the optimal number of diagnostic imaging machines per capita and for this
reason the Department submitted that it was not possible to ascertain where
Australia is positioned from an international perspective.[3]
2.7
Within Australia, the evidence provided by the Department indicated that
there is a relatively equal spread of machines per capita between the different
states and territories across most modalities.[4]
For example, the Department advised the committee that there are 28 CT machines
in the Australian Capital Territory—6.9 units per 100 000 residents—and
there are 562 CT machines in New South Wales—7.3 units per 100 000
residents.[5]
2.8
The original tables provided by the Department for each modality are
available at Appendix 3.
2.9
Even if there is relatively equal distribution of machines by state and
territory per capita around Australia, diagnostic imaging machines are not
necessarily distributed evenly around those states, and the geographic
disparities extend both to the availability of diagnostic imaging services and
the availability of experts to operate the equipment and interpret the results.[6]
2.10
According to Primary Health Care Limited—a service provider—attracting
and retaining radiologists and technical diagnostic professionals in regional
centres or low-socioeconomic areas is difficult.[7]
Issues relating to the diagnostic imaging workforce are discussed in chapter
four.
Case study: Queensland
2.11
Queensland, a decentralised state, is a good case study to consider
questions of distribution. Mr Eastgate, President of the Australian
Society of Medical Imaging and Radiation Therapy (ASMIRT) described Queensland
as operating a hub-and-spoke model:
When you look at the hub-and-spoke model, the more the acuity
of the condition the more likely you are to be funnelled back to one of the big
centres. That's where they need the high-acuity equipment to make an accurate
diagnosis for treatment.[8]
2.12
This means that the larger hospitals in major cities—the Royal Brisbane
and Women's Hospitals, The Prince Charles Hospital (Brisbane), Toowoomba
Hospital, Ipswich Hospital and Bundaberg Hospital—offer almost a complete suite
of diagnostic imaging services.[9]
2.13
In other regional areas of Queensland, such as Warwick, Goondiwindi and
Gatton, CT and Ultrasound services are provided in conjunction with a private
provider under a fee-for-service arrangement.[10]
Alternatively, patients may need to be referred to a private provider in some
cases. For example, Maryborough Hospital currently does not offer CT or nuclear
medicine services, though these are available from private providers in
Maryborough.[11]
2.14
In some more regional Queensland areas, such as Dalby and Kingaroy, the
Darling Downs Hospital and Health Service told the committee that CT services
were 'limited', even though they are considered to be regional hubs that
provide 24-hour coverage for emergencies.[12]
2.15
In rural locations, such as Kilcoy, Laidley, Gin Gin and Monto, often
only general x-ray services are provided.[13]
In some cases, these x-rays are taken by a non-radiographer and are reported
from another hospital.[14]
The reason for this is explored in greater detail in chapter four.
2.16
The concentration of equipment and human resources in larger cities, as
seen in Queensland, is replicated across Australia. Children's Healthcare
Australasia (CHA) and Women's Healthcare Australasia (WHA) explained that state
funded hospitals are the only providers of diagnostic imaging services in most
parts of the Northern Territory, Western Australia, far western Queensland and
far western New South Wales.[15]
Case study: PET services in New
South Wales
2.17
PET is a nuclear medicine imaging technology that is used to image
particular types of cancers, such as prostate cancer.[16]
2.18
Associate Professor Anthony Lowe from Prostate Cancer Foundation of Australia
explained to the committee that this form of imaging enabled oncologists to
understand if cancers are recurring and where those cancers are so that better
treatment plans can be developed.[17]
2.19
The location of nuclear medicine imaging, such as PET, is restricted because
PET equipment must be located 'within a facility that has comprehensive cancer
services for Medicare benefits purposes'.[18] A comprehensive facility,
as defined by the Health Insurance (Diagnostic Imaging Services Table)
Regulations 2017 (DIST), is a:
...building or part of
a building, or more than one building, where all of the following services are
performed (whether or not other services are also performed):
- PET;
- computed tomography;
- diagnostic ultrasound;
- medical oncology;
- radiation oncology;
- surgical oncology;
- x-ray.[19]
2.20
The number of facilities that offer all of these services is limited. In
New South Wales, the majority of these facilities are located in major cities. The
below map demonstrates that, despite a number of comprehensive cancer centres
being located around New South Wales, most of the PET scanners are located in
and around Sydney.
Figure
2.1—Location of PET services in New South Wales
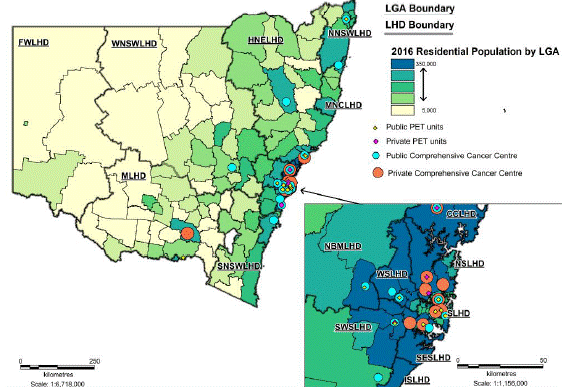
Source: New South Wales
Health, Submission 33, p. 2.
2.21
One reason for this may be the difficulty associated with the production
and transport of the radioisotopes required to operate the PET scanner due to
their short half-life. [20]
Accessibility of diagnostic imaging machines
2.22
Accessibility can take many forms and it means different things to
different people. One of the more comprehensive definitions the committee
received was from Cancer Voices Australia which told the committee that it
considered that full accessibility required physical, geographic, financial and
cultural access and timely reporting of the results.[21] However, the
definition the committee heard most frequently from submitters was based on
geography.[22]
Geographic accessibility
2.23
Submitters were concerned that living in regional, rural and remote areas
has adverse consequences for patients, namely:
-
patients have limited access to appropriate diagnostic imaging
services; and
-
patients face additional costs to access those services.
2.24
Access to up-to-date equipment (capital sensitivity measures) in regional,
rural and remote areas was another key issue discussed with the committee, and
is considered further in chapter five.
2.25
The committee was reminded by submitters that regional, rural and remote
Australians have poorer health outcomes than their urban counterparts.[23]
ASMIRT noted in its submission that 'statistics still demonstrate that the more
remotely people live, the greater the risk of dying young...'[24]
ASMIRT attributed the poorer health outcomes, in part, to diagnostic imaging
not being available in regional, rural and remote areas.[25]
ASMIRT also reported that common procedures, such as perfusion stroke imaging, are
not available and private providers are not required to offer a full range of
services.[26]
2.26
The availability of services in rural areas varies between modalities.
The representative of the Darling Downs Hospital and Health Service and the
West Moreton Hospital and Health Service called the state of CT services in
rural Queensland 'diabolical', and noted that access was particularly problematic
for cases of trauma and stroke.[27]
2.27
Even if the patient is able to obtain the required scan in a regional
area, they are likely to pay more for it. Primary Health Care Limited advised
the committee that independent research had found that rural patients pay
almost 25 per cent more for diagnostic images (the average out-of-pocket
payment for an inner city service is $86 whereas the average out-of-pocket
charge in rural areas is $107).[28]
2.28
These factors often require rural patients to travel to access services.
Travel and patient travel subsidy
schemes
2.29
Travel and other related expenses pose unique financial and personal
challenges for patients from regional, rural and remote areas, including travel
and accommodation costs, absence from work, family travel costs and arrangement
for family members left behind.[29]
2.30
The Queensland Nurses and Midwives' Union (QNMU) noted that 85 per cent
of Australia is classified as remote and that in many cases people who live in
rural, regional or remote parts of Australia must travel long distances to access
imaging services. The QNMU provided the example that a patient who lives in
Weipa must travel 800 kilometres to Cairns if they require an MRI.[30]
2.31
The Australian Medical Association (AMA) provided the committee with an
example of a rural patient who experiences chest pain and may have to make such
a trip multiple times :
...a patient initially presenting to a general practitioner
with chest pain would generally be referred for an X-ray; then if showing an
abnormal result, for a CT scan. If the CT scan indicates a possible tumour, the
patient will need to be referred to a specialist medical practitioner who may
then arrange a fine needle biopsy...Under this scenario, a country patient moving
through this pathway of care would need to return to the city for these
services three separate times, because each time a new referral is required
from the general practitioner and then specialist medical practitioner. Not
only are multiple trips expensive and disruptive for the patient, but a definitive
diagnosis is delayed by many weeks, even assuming the patient complies with
each referral promptly.[31]
2.32
Service providers in both Queensland and Western Australia detailed the
complexity of providing diagnostic imaging services in regional, rural and
remote areas. In some cases, patients are transported from rural hospitals and
taken to either a larger population centre, or to a private diagnostic imaging
service provider.[32]
2.33
Some of these costs can be lessened through state-funded patient travel
subsidy programs.[33]
Rare Cancers Australia argued that travel schemes are needed as a matter of
equity:
Geographical barriers need to be mediated by user-friendly
and accessible transport and accommodation subsidy schemes. The current
state-based travel schemes lack consistency and are funded as an add on
healthcare benefit where they need to be viewed and funded as essential and
first line. Timely access to diagnostic imaging should not be determined by
someone's bank balance or postcode.[34]
2.34
However, the committee heard that subsidy programs, if available, do not
adequately alleviate these financial pressures. The AMA acknowledged that state
and territory travel and accommodation assistance schemes for remote patients
'are administratively difficult and complex to access and provide relatively
small reimbursements'.[35]
2.35
That view was endorsed by the representative of the Darling Downs
Hospital and Health Service and the West Moreton Hospital and Health Service
who described the patient transport service in the following terms:
The process is paper-heavy and inefficient and sees a
significant shortfall between the amounts provided by PTSS [Patient Travel
Subsidy Scheme] and the actual cost of transport and accommodation,
particularly for multiday stays for diagnostics or outpatient care. This acts
as a significant disincentive for having imaging performed and leads to poorer
outcomes for patients. Topping up the state-based PTS or otherwise financially
supporting rural and remote patients for their travel and accommodation
associated with imaging would go a long way to allowing better access to
services by removing financial constraints to attending appointments. This is a
particular issue for Aboriginal and Torres Strait Islander patients.[36]
2.36
Aboriginal and Torres Strait Islander patients often culturally require
an escort. Cancer Council Northern Territory told the committee that a lack of
funding meant that having an escort travel with them was not always possible:
Patient Assistance Travel Scheme are not always able to
provide funding for escorts for remote indigenous patients requiring invasive
procedures or treatments. Patients will decline to come into town unless accompanied
by a family member or escort thus delaying diagnosis, treatment and with the
potential for poorer outcomes in an already disadvantaged population. Cost of
transport from airport to accommodation is not provided and is a significant
outlay for people travelling.[37]
2.37
The QNMU noted that even in cases where funding is available, if the
patient lives in a remote location, the escort may be the only health worker in
the community or the transport vehicle may be the only emergency vehicle in the
town.[38]
2.38
In many cases, having to travel a long distance may either cause the
patient to delay the procedure or elect not to have the diagnostic images taken
at all.[39]
2.39
These problems and costs are exacerbated if the patient requires
multiple scans.
Multiple service rule
2.40
The financial burden is magnified when patients are required to travel
back and forth to access multiple diagnostic services. This concern was raised
by the representative of Breast Cancer Network Australia (BCNA) who explained
that the multiple services rule prevents patients from accessing the Medicare
rebate for the second procedure. For example, in instances of breast cancer
diagnostic ultrasounds being followed by a core biopsy to confirm an ultrasound
diagnostic result, patients wishing to access the Medicare rebate are required
to return the following day to have that procedure.[40]
2.41
Rules applying to the payment of Medicare benefits for multiple diagnostic
imaging services were put in place to reflect efficiencies to the provider when
multiple services are provided to a patient at the same attendance or on the
same day. Providers have a responsibility to ensure they are reflecting these
efficiencies in the costs they pass on to patients, rather than encouraging
multiple visits.
2.42
BCNA's observations were supported by the Australasian Society for
Ultrasound in Medicine which provided the committee with the example of a
patient who attended a clinic with a breast lump:
...a patient who attends an imaging centre with a breast lump
will have their mammogram and ultrasound performed. However. [sic] if it is
decided that the patient requires a biopsy or aspiration for their own benefit
and diagnosis, either the patient pays out-of-pocket or would need to return
delaying the diagnosis or potentially no conclusive diagnosis at all.[41]
2.43
The committee raised the issue of referral pathways for regional, rural
and remote patients with the Department. On notice, the Department responded to
evidence provided by the BCNA regarding diagnostic ultrasound and ultrasound
core biopsy. It explained that the rules that apply to payment of Medicare
benefits when multiple diagnostic services are provided are:
...long-standing and were developed in conjunction with the
diagnostic imaging profession. The rules reflect efficiencies to the provider
when multiple services are provided to a patient at the same attendance or on
the same day.[42]
2.44
For ultrasound services, the Department stated that Medicare benefits
are payable 'for one ultrasound examination performed within a three hour
period on the same day'. The Department reconfirmed that the 'multiple services
rules are being considered by the Medicare Benefits Schedule Review Taskforce'.[43]
2.45
However, the AMA called for the Medicare system and the referral
pathways for diagnostic imaging services to be:
...rationalised to prevent people living in the country having
to travel back and forth to obtain multiple referrals as they move along the
diagnostic and treatment pathway.[44]
Teleradiology
2.46
New and innovative technological advancements have improved the
accessibility of diagnostic imaging services, in particular for patients based
in regional, rural and remote communities.[45]
A large number of submitters told the committee of how telemedicine[46]
has supported the work of diagnostic imaging clinicians, streamlined visits for
patients and co-ordinating support for patients.[47]
The Australian College of Rural and Remote Medicine (ACRRM) noted that
telehealth (telemedicine) supports rural and regional diagnostic imaging
services by increasing the 'accessibility and equity for rural and regional
areas where it is difficult or impractical to recruit and retain radiologists.'[48]
Further, the ACRRM reported that the use of telehealth in outer-metropolitan
Brisbane had saved Redcliffe Hospital $50 000 in one year alone.[49]
2.47
In instances where telehealth is used, ASMIRT pointed out that it is
important for the images or reports to be added to a patient's electronic
health record. However, ASMIRT noted that this was often not the case, making
comparison with earlier scans difficult.[50]
2.48
Telehealth works where there is coordination between hospitals and a
swift transfer of images, but ASMIRT also noted that this is not currently
possible in Tasmania:
At present there is no way to send the patient images except
by DVD and via Australia Post, although images are sent to the mainland every
day for reporting by radiologists. The key issue relates to no data sharing
amongst public hospitals. Although the mainland states have this capability,
Tasmanians are told it is too expensive resulting in 500,000 people being
disadvantaged by this and other e health provisions.[51]
2.49
Cancer Council Norther Territory noted that it too had encountered
similar problems related to the sharing of images:
Lack of co-ordinated/ national approach for sharing of
digital images and reports between private and public radiology services can
potential[ly] delay management plans & treatment when remote clients attend
surgical or other appointments. Valuable staffing resources can be wasted
trying to facilitate this sharing of information.[52]
Physical accessibility
2.50
Spinal Cord Injuries Australia (SCIA) advised the committee of the
unique challenges faced by people with spinal cord injury and other physical
disability accessing diagnostic imaging equipment. SCIA submitted that people
reliant on mobility aids (manual and power wheelchairs):
...often encounter access barriers to services, facilities,
transport, buildings and the built environment, including access to diagnostic
imaging equipment, due to the geographical access barriers, or especially the
physical access barriers to this equipment.[53]
2.51
For example, it is often difficult or impossible for women with
disability to have a mammogram because:
-
mobile mammogram units may not have lift access;
-
a mammogram service with the infrastructure for mobility aids may
be located at a distance resulting in the women having to incur relatively
expensive taxi services;[54]
and
-
mammogram equipment may not be designed for women in mobility
aids.[55]
2.52
SCIA also explained that people using mobility aids may not be able to
undergo scans that require the 'patient to be transferred onto an imaging bed
or examination table if there is no lifting hoist and sling'.[56]
Further, rooms that house diagnostic imaging equipment may not have adequate
floor space for the wheelchair user and a mobile floor hoist (if available).[57]
For bone density scans, patients are required to be weighed, and in some
diagnostic imaging facilities there may not be a hoist or sling with a weighing
mechanism.[58]
2.53
SCIA recommended that the Commonwealth Government engage with diagnostic
imaging equipment companies to ensure equipment, particularly mammography
equipment is designed for people using mobility aids. Further, diagnostic
imaging practices should ensure that patients using mobility aids have access
to:
-
ceiling or mobile hoists and slings that come in various sizes;
-
mobile mammography facilities with wheelchair hoists that are
serviced regularly;
-
weight measuring devices that are used on the hoists;
-
appropriate information about, and financial assistance for,
accessible transport services; and
-
mammography facilities which can accommodate a mobility aid with
non‑detachable armrests.[59]
Regulatory barriers to
accessibility: cone beam computed tomography in Western Australia
2.54
Regulation can sometimes create access issues. For example, the
committee heard that there are regulatory barriers associated with dental
professionals accessing cone beam computed tomography (CBCT) in Western
Australia.[60]
2.55
Mr Troy Williams of the Australian Dental Industry Association outlined
the benefit of this technology for dentists and allied professionals, such as
orthodontists, explaining that health-care professionals use CBCT for a number
of purposes, including:
... to produce 3-D digital images of teeth, soft tissue, nerve
pathways and bone, and they can do it all with a single scan.[61]
2.56
The committee was informed that in Western Australia current
restrictions mean that very few practitioners are able to own and operate this
equipment.[62]
2.57
The committee heard that, with the exception of Western Australia,
healthcare professionals who wish to use the CBCT equipment are subject to only
limited regulation:
...[professionals] must be registered with the Australian
Health Practitioner Regulation Agency, usually via the Dental Board of
Australia. There is then a requirement to possess experience in radiation
safety, and often the professional will have completed a short course covering
radiation safety, along with the operation of the CBCT equipment.[63]
2.58
Mr Williams outlined that regulatory requirements in Western Australia
require a dentist to be registered with the Australian Health Practitioner
Regulation Agency in the speciality of dental maxillofacial radiology.[64]
Mr Williams noted that '[a]lmost none of Western Australia's 1,780-odd dentists
satisfy this requirement', with the result that Western Australia physicians
have 'restricted access to this equipment'.[65]
2.59
Mr Williams explained that these restrictions have limited the access of
Western Australians to this technology:
The estimate on the number of CBCT machines used nationally
in dentistry varies depending on the dataset, but it's estimated to be between
360 and 420 machines nationally. What is known is that fewer than 10 of these
are in Western Australia. Clearly, access to this important diagnostic
technology is an issue for those in Western Australia.[66]
2.60
Mr Williams accepted that a uniform approach to CBCT regulation was
not possible due to constitutional limitations, but he suggested it was
important for the committee to understand the nature of these restrictions
because it affected other parts of the health system:
...there is an additional cost burden on the patient,
particularly in Western Australia. So if you're in Bunbury, if you're in
Broome, if you're in Karratha, the access to that technology is just not
available...So it's a case of highlighting it and raising it with the Western
Australian government in terms of broader health economics. It's either
resulting in patients not getting the level of diagnosis and care that's
appropriate to them, which manifests itself in costs otherwise or, in some
cases—at the patient's expense and the broader healthcare system—of them
travelling to Perth to get access to the technology. It is understood that the
Commonwealth's powers in this area are limited...[67]
2.61
Despite this, Mr Williams informed the committee that some reform may be
forthcoming in this area. The committee understands that the Radiological
Council of Western Australia has met and proposed reforms to this system, with
the result that:
Western Australia now looks set to cut the red tape
associated with owning CBCT digital imaging equipment. It's been proposed that
registered dentists who have successfully completed a recognised CBCT course be
able to apply for a licence to own and operate the equipment. The council looks
set to recognise courses offered by the School of Dentistry at the University
of Queensland and by the Adelaide Dental School, within the University of
Adelaide and with a course by a private provider. There'll be a requirement
that all CBCT images must be reported on by an [Australian Health Practitioner Regulation
Agency]-registered radiologist or a dentomaxillofacial radiologist. As part of
the initial registration of the CBCT equipment with the council, dentists will
need to provide confirmation of a service agreement from the radiologist or the
dentomaxillofacial radiologist.[68]
2.62
However, the Australian Dental Industry Association opposes the aspect
of the proposed reform that the operation of the CBCT equipment will be limited
only to dentists who will not be permitted to direct and supervise other
practitioners in the use of the unit.[69]
Committee view
2.63
The committee considers that Australians should, to the greatest degree
possible, have equitable access to quality medical care, including diagnostic
imaging services.
2.64
The current geographical variation in diagnostic imaging equipment is
greater between urban and rural areas than between the states and territories. To
that extent, patient transport subsidies are especially important to rural
patients. The committee notes that the existing state-funded patient transport
subsidies are currently not sufficient to alleviate the financial burden placed
on regional, rural and remote patients who are required to travel for diagnostic
scans.
2.65
The committee is concerned that the implementation of the multiple
services rule requires patients to incur additional delays and costs in
accessing services and treatment. The committee is particularly concerned about
the impact this rule has on rural and remote Australians. The committee
understands that the MBS multiple services rule is currently subject to review
by the MBS Review Taskforce. The committee urges the MBS Review Taskforce to
carefully consider the impact this rule is having on patients.
2.66
The committee is concerned and disappointed by reports that many
diagnostic imaging services are not physically accessible for people with
disability. The committee considers that this underscores the need for
government and others to redouble their efforts to create accessible
communities, as noted by the committee in its recent inquiry into the National
Disability Strategy.[70]
2.67
The committee agrees that the current restrictions in place in Western
Australia for the use of CBCT seem to have hampered the access of Western
Australians to this technology. The committee welcomes the discussions between
the Western Australian Government and the Radiological Council of Western
Australia and the Australian Dental Industry Association and expects that a
suitable resolution can be found.
Navigation: Previous Page | Contents | Next Page