Chapter 3
Affordable access –assessing cost effectiveness
3.1
As noted in Chapter 1, the Australian Government, like most governments
in developed countries, provides subsidised patient access to medicines. For
medicines listed on the Pharmaceutical Benefits Scheme (PBS), patients pay a
contribution depending on their status as a general or concessional patient.
The PBS provides safety nets to protect high medicine users from excessive
medicine costs.[1]
The Department of Health (DOH) explained that the PBS ensures that although the
cost of most new cancer therapies can run to many thousands of dollars,
Australian patients pay no more than the co-payment.[2]
3.2
Funding new cancer medicines is a challenging policy issue for all
governments. The Australian Government uses a range of Health Technology
Assessment (HTA) processes and mechanisms to determine which medicines will
receive subsidy through the PBS. HTA seeks to provide a basis for providing
subsidised access to new medicines while at the same time ensuring the sustainability
of the PBS.
3.3
The National Medicines Policy (NMP) provides the overarching framework
for the operation of the PBS. The NMP seeks to balance the following key
factors: timely access to the medicines Australians need, at a cost individuals
and the community can afford while maintaining a responsible and viable
medicines industry.[3]
3.4
This chapter examines two key factors that influence affordable access
to cancer drugs, the Pharmaceutical Benefits Advisory Committee (PBAC) assessment
of the cost and the effectiveness of new cancer medicines as a prerequisite for
listing on the PBS. The committee particularly considers concerns regarding the
appropriateness of this approach to the assessment of cancer medicines. The
methods used by PBAC to evaluate the cost effectiveness of cancer medicines are
a source of some concern to many submitters. While recognising the value of a rigorous
evidence based assessment process, many submitters expressed concern that the
current PBAC assessment processes are unable to effectively respond to the
volume and complexity of applications for listing of new and innovative cancer
drugs on the PBS. A number of submitters expressed the view that PBAC's
evaluation methodologies are limiting access to life-saving new therapies,
variously describing the current assessment methodology as 'antiquated',
inflexible, 'one-size-fits-all' approach and a key factor in limiting access to
new cancer medicines.[4]
The PBAC assessment framework
3.5
The National Health Act 1953, requires the PBAC to consider both the
cost and clinical effectiveness of a proposed PBS listing relative to existing
therapies.
Section 101 (3) (A) specifies that the 'Committee shall
give consideration to the effectiveness and cost of therapy involving the use
of the drug, preparation or class, including by comparing the effectiveness and
cost of that therapy with that of alternative therapies, whether or not
involving the use of other drugs or preparations.'
Section 101 (3) (B) states that 'where therapy involving
the use of a particular drug or medicinal preparation, or a class of drugs and
medicinal preparations, is substantially more costly than an alternative
therapy or alternative therapies, whether or not involving the use of other
drugs or preparations, the Committee:
(a) shall not recommend to the Minister that the drug,
preparation or class be made available as pharmaceutical benefits under this
Part unless the Committee is satisfied that the first mentioned therapy, for
some patients, provides a significant improvement in efficacy or reduction of
toxicity over the alternative therapy or therapies.'[5]
3.6
In recommending a listing to the Minister, PBAC also provides advice
about how the new listing compares with alternative medicines and/or the current
standard of care in terms of cost effectiveness ('value for money').[6]
3.7
Major submissions to the PBAC are required to include an economic
evaluation to enable the PBAC to consider how much it would cost to achieve
additional health outcomes with the proposed medicine compared with existing
therapies that would be replaced.[7]
The PBAC explained that consideration of 'cost' includes 'both the cost per
patient treated and the total cost to the PBS, taking into account the number
of patients likely to be given the drug'.[8]
3.8
The principles and methodologies used by the PBAC are set out in the
PBAC Guidelines (Guidelines).
The primary focus of an economic evaluation for PBAC decision
making is on how much it would cost to achieve additional health outcomes with
the new therapy ('proposed medicine') compared to existing therapies that would
be replaced ('incremental cost-effectiveness'). Therefore, in the first
instance, the costs associated with altered uses of medicines, medical and
other related health care resources all need to be taken into account and
outcomes valued in terms of overall quality and length of life; for example,
'quality-adjusted life years gained' (cost-utility analysis). This evaluation
is referred to as the base case.[9]
3.9
The PBAC told the committee that the approach used 'enables drugs to be
compared directly to existing best treatments, and the additional benefits and
costs weighed across all types of diseases and treatments. This means that two
drugs can be equitably assessed even if one treats a rare but serious disease
and another relieves the symptoms of a common but less serious chronic
condition, or if one is very expensive but will be used for very few patients
and another is low cost but will be used by very large numbers of Australians.[10]
3.10
DOH provided the following summary of the PBAC approach to cost
effectiveness:
The PBAC essentially asks the question 'Is it worth spending
an additional $x to achieve the additional benefit offered by the new drug
compared to existing therapy?'. In answering this question, the PBAC takes into
account a range of factors including the availability and cost of alternative
treatments and the total cost and probable demand for the proposed medicine.[11]
3.11
The committee notes that the PBAC Guidelines are currently being
reviewed. The review will identify significant new developments for methods
since 2008 and will consider 'the relevance to PBAC practice of existing
guidance documents on relevant methodologies contained within guidelines
published by comparable international health technology assessment agencies,
regulators and internationally recognised authorities in the assessment of
evidence'.[12]
Evaluation of cost
3.12
The PBAC noted that one of the major challenges in the evaluation of the
cost effectiveness of cancer drugs is that cancer drugs cost significantly more
than other drugs.
Cancer drugs that have been assessed by the Committee in the
recent past have nearly all been, by any standards, "substantially more
costly" than 'alternate therapies', as has recently been reported in the
media and medical literature.[13]
3.13
The committee notes that the potential total cost of the 11 major
submissions for cancer medicines considered at the PBAC's March 2015 meeting
was $589 million. These submissions represent 23 per cent of the total number
of submissions considered at the March meeting.[14]
3.14
As noted in chapter 1, cancer medicines are among the most expensive
medicines on the PBS. Figure 3.1 indicates that new cancer medicines make up an
increasing proportion of total PBS spending on cancer medicines. DOH advised
that PBS benefits paid for new cancer medicines have increased at a rate of 33
per cent per year over the last five financial year, compared to a growth rate
of only five per cent per year in benefits paid for established cancer medicines.
In addition, DOH noted that:
The PBS ensures that although the cost of most new cancer
therapies can run to many thousands of dollars, Australian patients pay no more
than the co-payment. On average over the last five financial years, the patient
co-payment funded between 2-3% of the total cost of cancer medicines, compared
to 15% for non-cancer medicines. The taxpayer funds the remainder.[15]
Figure 3.1: Patient numbers and
expenditure for cancer medicine versus non-cancer medicine.
|
Financial Year
|
Cancer Medicine
|
|
Patient Count
|
Scripts
|
Benefit
|
Patient
co-payment contribution as percentage of total cost
|
|
2009-10
|
270,510
|
1,957,274
|
$993,745,236
|
3%
|
|
2010-11
|
287,127
|
2,066,655
|
$1,086,669,622
|
3%
|
|
2011-12
|
295,470
|
2,234,906
|
$1,135,299,000
|
3%
|
|
2012-13
|
314,056
|
2,434,837
|
$1,230,201,528
|
2%
|
|
2013-14
|
337,289
|
2,607,167
|
$1,485,961,705
|
2%
|
|
Financial Year
|
Non Cancer Medicine
|
|
Patient Count
|
Scripts
|
Benefit
|
Patient
co-payment contribution as percentage of total cost
|
|
2009-10
|
9,323,301
|
196,783,171
|
$6,998,721,883
|
17%
|
|
2010-11
|
9,493,086
|
202,950,640
|
$7,359,173,190
|
17%
|
|
2011-12
|
9,521,127
|
207,170,478
|
$7,646,269,254
|
17%
|
|
2012-13
|
9,450,295
|
208,178,027
|
$7,562,826,568
|
17%
|
|
2013-14
|
9,437,378
|
211,113,143
|
$7,709,455,066
|
16%
|
Source: Department of Health,
Submission 197, p. 31.
3.15
The committee notes that the increasingly high cost of cancer medicines
poses a significant challenge for the PBAC in assessing cost-effectiveness.
3.16
DOH stated that while the cost of new cancer medicines are substantially
higher than other new non-cancer medicines, many new cancer medicines offer
only a small incremental survival benefit to patients. DOH stated that '[e]ven
where the health benefits may be considered large, the prohibitive cost can act
to restrict access, even after a reasonable timeframe to recoup development
costs'.[16]
Comparative cost-effectiveness
3.17
The calculation of value for money is based on a health economic
equation: the Incremental Cost Effectiveness Ratio (ICER), which is a
cost/benefit ratio, quantifying the additional cost incurred for an additional
health benefit derived.[17]
3.18
Unlike a number of other countries, the PBAC does not use a definitive
threshold when assessing the cost effectiveness of medicines. Instead, it references
the prices of new medicines against existing listed treatments for the same or
similar indications.[18]
Where there is no listed alternative treatment the PBAC considers the 'clinical
place, overall effectiveness, cost and cost-effectiveness of the proposed
medicine compare with standard medical care'.[19]
3.19
DOH told the committee that the comparative cost-effectiveness method is
able to achieve better price outcomes as medicines which offer the same health
benefits and have the same safety profiles will generally attract similar
prices.[20]
3.20
Ms Felicity McNeill, First Assistant Secretary, Pharmaceutical Benefits
Division, DOH, told the committee that the fact that the PBAC does not have
fixed thresholds, is one of the advantages that the PBAC has over assessment
models used in other countries:
The PBAC has the flexibility, where something is of a
particularly high cost, or there is a high cost of the quality of life you
gain, to take other factors into account, such as the high clinical need or the
severity of the disease, to make that drug suitable for recommendation. I think
the drug ... Soliris, is a very good example of where the health outcome that was
delivered, which was well beyond the expected quality of life year gained in a
traditional model, was considered by the PBAC. They have extraordinary
flexibility, and they use it where they think they can. Whereas [under the
United Kingdom's National Institute for Health and Care Excellence (NICE)
system] you will have a fixed threshold, they do not have those thresholds.[21]
3.21
However, some submitters questioned the claim that the PBAC does not
apply a fixed cost-effectiveness threshold in determining value for money. Novo
Nordisk (NN) argued that while there is no explicit cost-effectiveness
threshold for reimbursement of medicines in Australia, over the past four
years, more than half of the major cost effectiveness submissions rejected by
the PBAC have had an ICER below $45,000. NN states that this is 'despite
Australia's economic capacity to pay for innovative and advanced treatments'.
NN argued that the current PBAC policy and process significantly restricts the
ability of pharmaceutical companies to achieve a reasonable premium for new
medicines.[22]
3.22
Medicines Australia (MA) submitted that the experiences of sponsors of
new medicines 'reveal that the PBAC's acceptable ICER is in the range of
$45 000-$75 000. MA further stated that the implicit acceptable threshold is
lowered when any form of clinical, economic and financial uncertainty exists in
the economic evaluation, claiming that this contention is supported by ICER ranges
captured in Public Summary Documents for recommended medicines.
3.23
DOH provided the following table to illustrate ICERs for first cancer
submissions compared to recommended submissions. This indicates that the ICERs
of the middle 50 per cent of recommended applications are in the range of
$42 000-$61 000.
Figure 3.2: ICERs
for first cancer submissions vs. recommended cancer submissions
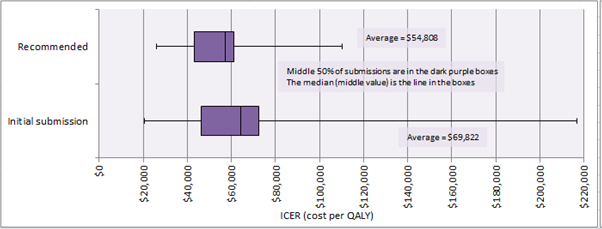
Source: Department of Health,
Submission 197, p. 31.
3.24
Pharmaceutical companies expressed concern that the PBAC comparative
costing model poses a challenge to establishing cost effectiveness for cancer
medicines. For example, Merck Sharp and Dohme (MSD) expressed concern that the
PBAC practice of referencing the prices of new medicines against older existing
treatments does not recognise the true value of new cancer medicines and cited
examples of submissions that had proved unsuccessful on the basis of an
'unacceptably high incremental cost-effectiveness ratio'.[23]
Submitters argued that price reductions as a result of post PBAC reviews have
led to an erosion of the prices of comparator medicines, 'even recently listed
on-patent medicines'.[24]
3.25
Submitters also questioned the relevance of cost-effectiveness to the
assessment of new innovative treatments for cancer, noting that a number of
factors mean that development costs for cancer medicines are invariably higher
than for non-cancer medicines.[25]
Submitters noted that advances in understanding of the formation and
characteristics of the 'myriad diseases we refer to under the "catch
all" banner that is cancer' has led to a focus on smaller disease
populations.[26]
This in turn has led to increased costs associated with the development of
clinical trials. For example, trials in small populations must be run in many
sites and over long periods of time in order to recruit sufficient patients,
with patient identification itself requiring costly and elaborate testing.[27]
3.26
Rare Cancers Australia noted that there are real challenges in
establishing the evidence to support the high cost of many cancer medicines,
especially when the benefits are incremental and apply only to a small
population.[28]
3.27
Pharmaceutical companies agreed that the current approach significantly
restricts the ability of the industry to achieve a reasonable premium for new
medicines. MSD explained the high prices associated with cancer drugs reflect
the significant investment required in research and development to bring
medicines to market. MSD noted that over time, the cost of individual medicines
becomes comparatively lower, 'because drugs are not subject to price increases,
unlike all other health care costs, and once generic they will be available at
a significantly reduced price'.[29]
3.28
On a related issue, Amgen submitted that it may be difficult to
demonstrate favourable cost effectiveness when a high cost new medicine is
compared to a low priced off-patent medicine.[30]
Eli Lilly Australia (Lilly) illustrated this by reference to its application
for listing of the drug Alimta, used in the treatment of non-small cell lung cancer:
At the time of PBAC's consideration of Alimta for first-line
use the patent on Gemzar, the existing standard of care, had expired. Gemzar
became subject to a very significant price fall (the price of the comparator
'eroded'). This price fall did not reflect any change to the therapeutic value
of Gemzar but did significantly impact on the consideration by the PBAC of the
comparative value of the benefits of Alimta for first-line use. As a
consequence, Alimta was recommended under the PBS but the price recommended by
the PBAC process for Alimta was significantly lower than if the patent on
Gemzar had not expired. That price fell substantially below what Lilly considered
to be the fair value of Alimta. As a consequence, Lilly chose not to pursue the
reimbursement of Alimta for first-line use.[31]
3.29
MSD submitted that the application of a 'shadow price' mechanism would
better reflect the fair value of innovative medicines. A shadow price would be
a Consumer Price Index adjusted price of the reference medicine when it was
launched. Cost effectiveness analyses would then be undertaken using the shadow
price.[32]
3.30
However, evidence from DOH indicated that the continual review of the
cost of PBS medicines contributes to the ongoing cost effectiveness of listed
medicines and the sustainability of the PBS. Post-PBAC reviews, together with
mechanisms such as price disclosure, which monitors the discounting behaviour
of pharmaceutical companies, helps to ensure that any discounts offered in the
private market are reflected in the price paid by government. As a result, a
number of cancer medicines have taken significant price reductions:
For example, the ex-manufacturer price of an 80 mg vial of
docetaxel was $1,420 when it was first subsidised in August 1996. As a result
of competition, the price is estimated to be reduced to $17.43 following the
next round of price disclosure, scheduled for 1 April 2015.[33]
3.31
DOH noted that while price reductions achieved through price disclosure
achieve a better price for the government and therefore for taxpayers, they can
also directly benefit patients.
For example, the price of ondansetron 8mg tablets (used to
treat nausea from cancer treatment) has decreased from $57.50 to $22.70. For
general patients, this means they now pay $22.70 per script, rather than the
co-payment of $37.70.[34]
3.32
The committee also heard that the high cost of new cancer medicines is
not simply related to the cost of development and manufacture. The PBAC
submitted it considers a major barrier to rapid PBS listing for new cancer
drugs is the expectation of pharmaceutical companies with respect to pricing.
The reason new cancer drugs are so expensive has been the
subject of considerable debate but it is not simply related to the cost of
development and manufacture. The pharmaceutical industry's expectations in
relation to price and profit at international and national levels are also
relevant.[35]
3.33
PBAC noted that for many new cancer drugs the price being requested,
relative to the benefit of the medicine, is much higher than for other serious
life-threatening diseases, or for the evidence of health outcomes provided.[36]
3.34
Dr Agnes Vitry also submitted that several studies have demonstrated
that the higher prices set for new cancer medicines are neither explained by
their therapeutic value nor the cost of development. Dr Vitry noted evidence
that prices remain high despite the marketing of competitive products.[37]
3.35
DOH summarised the competing tension inherent in the assessment of the
cost effectiveness of cancer drugs.
Cancer medicine pricing is an international issue, for an
international industry, but access and subsidy responses are necessarily
national. Funding decisions will be based on a range of local factors –
clinical need, fiscal constraints, and opportunity costs to fund other forms of
cancer care and prevention, as well as other diseases. Public funders look to
maximise societal benefit, and thus must use different criteria to individuals
making personal treatment choices that address their own needs and preferences.[38]
Evidentiary requirements
3.36
As noted previously, the assessment of cancer drugs is undertaken on the
same basis as drugs for other illnesses. It includes assessment of clinical
evidence regarding benefits and harms, relative to the cost and other factors
such as the severity of the illness, the extent of unmet need and the views of
consumers.[39]
3.37
The Act requires the PBAC to determine that a drug provides a 'significant
improvement in efficacy or reduction in toxicity' compared to alternative
therapies. In its submission, the PBAC advised the committee that the benefits
of cancer drugs are assessed in terms of effects of overall survival,
progression-free survival (PFS), response to treatment, quality of life and
toxicity.[40]
3.38
Dr Suzanne Hill, the former Chair of the PBAC, explained that for all
medicines submitted to the PBAC, the committee assesses the effects of the
medicine based on the impact of the medicine on patient relevant outcomes:
So for cancer, we think of that in terms of the likelihood of
the new medicines producing improved survival compared to what we already have
or temporarily slowing progression of disease, which is the term used for
progression-free survival or, when we have it, the effects of [the medicine] on
the quality of life of the patient. In all cases, we need to consider the risk
of side effects or harm.[41]
3.39
The committee heard that the 'gold standard' for clinical evidence comes
from randomised and controlled trials[42]
and would ideally include final outcomes data. In its July 2013 report, Access
to cancer medicines in Australia, Deloitte Access Economics noted that
overall survival is considered to be a clinically relevant and meaningful
endpoint as it is relatively easy to measure, record and define and is free of
bias.[43]
However, as a number of submitters noted, this is not always a realistic or achievable
expectation for cancer medicines.[44]
3.40
An endpoint of overall survival substantially prolongs the duration of
clinical trials and increases both the number of patients that need to be
recruited and the cost of the trial. The longer a trial, the higher the range
of factors that may impact on the interpretation of the findings and the
greater the chance of encountering ethical challenges, such as denying patients
access to experimental treatments that have potential benefits.[45]
3.41
Roche Products submitted that one of the key challenges in gaining PBAC
approval is the PBAC has 'a low tolerance for uncertainty', which frequently
results in rejection and re-submission of applications and delays for cancer
patients. Mr David Pullar, Manager, Government Affairs and Public Policy at
Roche Products, noted:
If you want to have absolute confidence that a medicine can
be used at a very specific dose in a very specific patient population and
deliver X months of additional survival and quality of life, that is very
challenging to do and may just not be possible. We would be very happy to
collaborate in that type of research. There are always benefits. But we need
this system to be able to recognise that value and take a pragmatic approach to
interpreting it.[46]
3.42
NN expressed concern that the current base case evaluation of the
benefits of a new medicine is too narrow and does not include the broader
patient perspective or the economic view of the benefits of a healthy and
productive population.[47]
Despite the economic evaluation (i.e., the cost effectiveness
analysis) being mandated to take a 'societal perspective', only direct health
care costs can be included as the base case for the majority of submissions.
That is, no account can be made of 'indirect costs', including loss of
productivity, impact of time/wages lost by carers, increase in welfare /
disability payments, etc. This is unlike some of the other HTA systems in other
jurisdictions, e.g., the Nordic countries in Europe, who do account for
indirect costs.[48]
Reliance on evidence related to
progression free survival versus overall survival
3.43
DOH noted that, one of the main difficulties in assessing cancer
medicines is that survival improvements are difficult to determine and are
generally not the main outcome measured in clinical cancer trials:
Many trials use response rates or Progression Free Survival
[PFS] as the main outcome measure. PFS refers to the length of time, from
either the date of diagnosis or the start of treatment, that patients diagnosed
with the disease survive without their disease advancing.
While this is considered an improvement in the quality of a
cancer patient's life, many new cancer medicines improve Progression Free
Survival but do not lengthen the patient's life. Further, Progression Free
Survival outcomes do not readily translate to improvements in Overall Survival
or Quality of Life, but sponsors often use Progression Free Survival clinical
trial data to make assumptions about Overall Survival. This can make Overall
Survival estimates overly optimistic. However, even with optimistic estimates,
the Overall Survival benefits for cancer medicines submitted to PBAC are
generally quite low. Combined with high medicine costs, these small
improvements means some cancer medicines are found not to be cost-effective.[49]
3.44
MA responded to this evidence from DOH:
Any rigorous method of calculating the cost-effectiveness of
a medicine, as referenced by the DOH submission, still requires one or more
assumptions to be made. There are some examples where PBAC have imposed an
'assumption' in the extrapolation methodology for survival data that they
consider reasonable, yet it produces a long-term survival curve that is
clinically unrealistic or implausible, and unfavourable to the new drug. At the
same time, another country using the same rigorous methodology of Health
Technology Assessment, makes a more balance assumption (an assumption based on
highly informed specialist clinical input), which generates a much higher
long-term survival benefit for the same drug.[50]
3.45
Roche Products noted that cancer medicines are typically registered with
the TGA on the basis of PFS, ie the medicine significantly extends the time for
the cancer to recur following treatment response. Roche Products described PFS
as a relatively straight forward measure that usually compares the new medicine
and the prior 'standard of care'.[51]
However, the PBAC Guidelines state that clinical studies undertaken to support
a general marketing application to the TGA often have not collected the array of
information necessary for an economic evaluation by the PBAC.[52]
3.46
MA told the committee that, while the current PBAC guidelines do not
mandate the provision of overall survival (OS) data, and provide advice on
translating surrogate outcomes for use in evaluations where OS data is not
available, the PBAC has a clear preference for OS data. MA cited positive PBAC
recommendations based on PFS outcomes but clarified that these are usually
associated with strict conditions, such as price reductions and/or the requirement
for further data collections.[53]
3.47
Submitters expressed concern that reliance on 'gold standard' evidence
often results in high rejection rates, requiring the sponsor to lodge several
submissions before a listing recommendation is achieved.[54]
As noted earlier, delays may also result where the conditions of approval are
not acceptable from a sponsor company's perspective.
3.48
However, a number of submitters to the inquiry expressed concern that
the PBACs evidentiary requirements pose a significant barrier to early access
to new and innovative cancer drugs. Cancer Council Australia and Clinical
Oncology Society of Australia (CCA/COSA) told the committee that the evidential
requirements for PBS listing are probably one of the most prominent points of
contention. CCA/COSA expressed concern that an endpoint of overall survival
requires too long a time line for most cancer patients:
Based on the experience of our health professional
colleagues—people who are at the front line, who actually see patients—who have
seen significant numbers of patients over a number of years who have had a
benefit, we have made the point that it may take too long for that benefit to
translate into the type of survival benefit that must then be applied to making
a judgement about PBS listing.[55]
3.49
Janssen-Cilag (Janssen) expressed the view that delaying funding for an
endpoint of overall survival is economically perverse:
[T]he better a product is at providing survival the longer it
must wait before the benefit can be assessed. Traditional assessment for
funding broadens this gap. There is a need to look beyond the traditional
hierarchy of evidence and develop new ways to incorporate growing evidence
bases to support funding.[56]
3.50
Leukaemia Foundation of Australia (LFA) submitted that these challenges
are exacerbated in the case of orphan drugs for rare cancers, such as blood
cancers, due to the small patient population size and the associated difficulty
and cost of obtaining the required data. Noting the significant delays
experienced in the listing of these drugs, LFA argued that an alternate
mechanism is required to ensure access to drugs for rare conditions for which there
is no commercial incentive.[57]
3.51
Submitters to the inquiry indicated they would like to see greater
acceptance of a broader set of clinical outcomes. CCA/COSA submitted that
overall survival is only one critical endpoint that can be used to indicate the
efficacy of a cancer drug.[58]
CCA/COSA expressed strong support for earlier reportable endpoints, such as
objective tumour response rates and PFS, to be given greater weight in PBAC
assessment processes.[59]
3.52
The Haematology Society of Australia and New Zealand (HSANZ) told the
committee that, while it understood overall survival is usually considered to
be the most appropriate endpoint for demonstrating the efficacy of a medicine,
'in terms of a patient's well-being and clinical status, an improved PFS is a
highly meaningful entity which is more appropriate for the assessment of the
benefit of a cancer drug'.
Moreover, with increasing utilisation of targeted therapy,
surrogate endpoints in trials, such as biomarker levels and functional imaging
may be used instead of survival barometers, because the results of the trial
can be measured sooner. Importantly, with the availability of more lines of
treatment, many clinical trials have to rely on assessment by PFS, since OS can
be confounded by subsequent treatment. For ethical reasons, many trials have
also allowed patients to 'cross-over' to the arm of the novel therapy, making
demonstration of OS even more difficult. Such trials, even though the
'gold-standard' randomised Phase III trials, may not be the ideal vehicle to
demonstrate an improvement in OS in an effective drug. [60]
3.53
MA told the committee that the PBAC is responding to some of these
challenges. MA noted that the PBAC recently accepted the 'two-stage Webull
approach (Latimer 2014) to be the most reliable correction method to adjust for
trial cross-over for the drug pomalidomide'. MA commented that this is a
positive communication to the industry, albeit delivered indirectly. MA said
that this example highlights the need for all sponsors to be provided with
direct advice well in advance of lodging a submission.[61]
3.54
Roche Products argued that the totality of available evidence needs to
be considered in the evaluation of cancer drugs and that subsequent evidence
collection must be fit-for-purpose. Roche Products noted that the current
Access to Medicines Working Group, that comprises DOH and the medicines
industry, is working on initiatives to address this.[62]
3.55
DOH told the committee that the PBAC does give weight to PFS where
quality of life improvements can be demonstrated, but that this then needs to
be considered in terms of the cost of the new medicine.
Medicines that offer Progression Free Survival benefits but
not Overall Survival benefits may be able to be valued as 'life enhancing', but
the evidence does not support them as being 'life saving'. This distinction is
often not reflected in the prices requested by sponsors.
3.56
CCA/COSA told the committee advances in cancer research have generated a
greater understanding of molecular biology, resulting in the identification of
smaller subsets of cancer and, along with rare cancers, naturally produces
small patient sizes. CCA/COSA argues that greater use of surrogate endpoints
which still demonstrate major outcomes in benefit, 'would support the
generation of clinically meaningful data in cancers with long survival, or
generally present at a later stage'.[63]
3.57
the Australian and New Zealand Society of Palliative Care (ANZSPC) told
the committee that 'the requirement for stringent evidence-based efficacy,
while a good fundamental principle, has its limitations in the palliative care
population'.[64]
In its submission, PCA noted that medications commonly used in palliative care,
including Midazolam and glycopyrrolate, are not listed on the PBS, even though
they are found to be quite cost effective. Dr Chapman of ANZSPC told the
committee:
... these medicines are routinely used as part of palliative
care practice, though one of the complexities of the clinical practice of
palliative care is the evidence base for some routinely used mediations that
show efficacy in the patient in front of you may not be as broad as is required
for PBS listing. So, many of these medications have not been submitted by those
companies for those indications for that reason.[65]
3.58
MA told the committee that there is a need to acknowledge both the
complexity of cancer and the limitations of current regulatory and
reimbursement systems in responding to this. MA submitted that, rather than
denying access to cancer medicines on the basis of uncertainty, more flexible
evidentiary requirements should be adopted that are capable of dealing with
issues such as crossover in clinical trials and which properly reflect the
value of cancer medicines to patients, careers and the community.[66]
Measuring quality of life - assessing the value of cancer medicines
3.59
Many submissions to the inquiry expressed concern that the current
assessment methodology does not adequately capture quality of life
considerations. Cancer Drugs Alliance (CDA) described the cost effectiveness model
as out-dated and recommended shifting from what it described as a static
assessment of cost-effectiveness to an assessment of value and quality.[67]
3.60
As noted previously, the PBAC seeks to apply a consistent assessment
methodology across all medicines. Mr Andrew Stuart, Deputy Secretary, DOH
explained that use of the quality-adjusted life year (QALY) creates a level
playing field for all medicines for all patient groups:
The QALY is a quality-adjusted life year—that is, for each
medicine, how much improvement do we get from that medicine in a
quality-adjusted year of life for a patient for a given dollar? That is a very
good way and a pretty simple way of trying to put medicines on a level playing
field so that you can compare the cost-benefit of medicines across cancer and
multiple sclerosis and Alzheimer's disease and so on.[68]
3.61
The cost per QALY is used as a guide to the cost of the medicine
necessary to extend a person's life one year in a good state of health, or for
a longer period in a reduced state of health.[69]
DOH further explained:
A QALY is a value used to measure changes in life expectancy
and changes in quality of life from health interventions such as medicines. A
QALY of 1 is a year of perfect health, whereas death is considered to be zero.
This measure is used because it can give some comparability between varying
health conditions, such as those that cause death very quickly to those that cause
significant disability but do not shorten life span.[70]
3.62
The PBAC Guidelines indicate that, in considering the suitability of a
medicine for PBS listing, the PBAC focuses on health outcomes. While the PBAC
may consider nonhealth outcomes and the costs and cost offsets of nonhealth
care resources, these may not be as influential in decision making as health
care outcomes and resources:
PBAC may also consider nonhealth outcomes, including aspects
of the delivery of a health care intervention beyond the health gain obtained;
for example, greater convenience or production gains to society beyond those
valued by the population benefiting with improved health. However, the
valuation of nonhealth outcomes is not straightforward and those outcomes might
not be as influential in decision making as health outcomes.
Similarly, PBAC mainly considers the costs of providing
health care resources. These extend beyond the costs of the medicine to include
possible cost offsets of reduced provision of health care resources as a result
of listing a medicine. PBAC may also consider costs and cost offsets of
nonhealth care resources, but these might not be as influential in decision
making as health care resources.[71]
3.63
Submitters expressed concern that considerations of quality of life are
not given more weight in the assessment of cancer drugs[72]
and that the current PBAC assessment process is limited in its ability to
properly reflect the value of the health gains deemed important by cancer
patients themselves.[73]
Submitters also called for greater transparency in how such considerations are
incorporated into final PBAC decisions.[74]
3.64
Professor Zalcberg of CDA expressed concern that as a measure, the QALY
is not sufficiently sensitive to the value that an individual places on quality
of life.
You can use a QALY to equate people having a hip replacement
to someone with cancer diagnosed and who has got a year to live. You can simply
say: A QALY is a QALY. But I would ask the committee: is a quality-adjusted
life-year the same for someone who is having a hip replacement and can now walk
to their post box and get their letters without being in pain—and I am not
trying to belittle that as an unimportant problem; it is an important problem.
Is that quality the same as the quality for someone who has advanced cancer,
has a year to live and has an extension of a year? I do not have the answer to
that. I would say it is a community issue for discussion and to think about.
But patients with cancer do not have time to wait the two or three years that we
are talking about. Yes, this is an important problem across all serious
diseases and the reform process that we have talked about is equally applicable
to all serious conditions. But we need to be cognisant of the time frames and
what is happening in cancer.[75]
3.65
LFA also argued that more importance needs to be placed on assessment of
quality of life outcomes. 'If a new drug allows a person to get well and return
to work or to normal roles in family or community, should not the economic
benefits to society be taken into account?' LFA argued that the HTA tools used
by the PBAC should be extended to include wider quality of life measures when
assessing the cost benefits of targeted drugs for rare/subtype cancers.[76]
3.66
Dr Katherine Nielsen, Director of Research and Advocacy, Ovarian Cancer
Australia, told the committee that consideration of the value of a cancer drug
should incorporate facts such as a clear extension of remission, improvement of
symptoms and quality of life.
These aspects are rated highly important by women with
ovarian cancer. Our research showed that greater than 90 per cent of women
rated the value of a treatment highly if it extended the period of remission or
made them feel better. We need a formal mechanism to evaluate and score quality
of life and progression-free survival in healthy technology assessments of
benefit and value.[77]
3.67
Novartis drew the committee's attention to a 2014 analysis of five
countries, including Australia, that use cost per QALY versus those countries
that do not, which found that access to novel cancer medicines was lower in
countries using QALY than in the countries not using QALY. Novartis noted that
this analysis also found, based on recent survival data, the countries which
use fewer novel medicines may achieve less favourable outcomes for patients.[78]
3.68
Roche Products noted that several countries are investigating
multi-criteria decision making, 'which incorporates numerous decision criteria
and also allows for weighted consideration for the criteria'. Roche Products
proposed that a review of the PBAC process could usefully draw on the
experience of countries such as the Netherlands, Sweden and the Canadian
province of Quebec in considering indirect costs and benefits such as patient
and carer work productivity.[79]
3.69
Mr Richard Vines, Executive Chair, Rare Cancers Australia, summed up the
general tenor of many submissions.
This issue is not just about money; it is about compassion.
It is about hope. It is about quality of life. It is about quantity of life. It
is about time with children. It is about time with family. And it is about
dignity and grace at the end of life. It is about how we as a community care
for those amongst us who are most vulnerable. Perhaps, most critically, it is
also about how we empower our cancer physicians to care for us. They are the
ones we trust with our lives, no-one else.[80]
Facilitating input from clinicians
and the community
3.70
Many submitters argued that a key step in balancing economic
considerations with greater recognition of broader quality of life
considerations in the assessment of cancer medicines is for there to be greater
emphasis placed on expert oncology and consumer input into the decision making
process.[81]
3.71
Current PBAC processes include provision for expert oncology and
consumer comments to be considered as part of the evaluation of applications
for PBS subsidy. Patients, carers, members of the public and health
professionals and members of consumer interest groups are able to provide
comments on applications under consideration at particular meetings via an
online submission process.[82]
3.72
The committee heard that consumers and consumer organisations can
experience difficulties in participating in the PBAC process.[83]
3.73
The PBAC Guidelines also state that the PBAC may:
-
seek expert opinion from relevant professional bodies and/or
appropriate specialists;
-
meet with relevant medical professional organisations; and
-
seek input from appropriate consumer bodies.[84]
3.74
However, the committee heard that such stakeholders should have a
stronger voice in work of the PBAC, as well as providing input to decision
makers about the reimbursement of individual cancer medicines.[85]
3.75
Dr Christopher Steer, President, Private Cancer Physicians of Australia
and Member of the Medical Oncology Group of Australia told the committee of the
key role that clinicians can play in informing the assessment of cancer drugs.
Dr Steer described clinicians as gatekeepers of the process caught between the
population based thinking of the PBAC and government and the need to advocate
for the individual patient:
We cancer clinicians understand the relative benefits and
limitations of new treatments according to clinical trial evidence. We feel we
can advise decision makers from a position of some authority based on science.[86]
3.76
Ms Nicola Richards, Head of Public Affairs at MSD noted that the PBAC
system needs to capitalise on the fact that Australia has some of the world's
leading oncologists:
We are often involved in the cutting-edge clinical trials so
who better than them to give the PBAC advice on: if we do not have overall
survival for this drug for five years, what do they think this offers their
patients and what do the patients think it offers them? Because two to three
months for patients and clinicians is often the bridge between one treatment
and the next treatment and extends their life.
Every advance in a cancer like breast cancer is a combination
of incremental benefit over time. It is not usually one massive jump. We are
always looking for the massive jump in outcome survival for any drug but that
does not happen overnight and it does not happen easily. So that input you will
see in a lot of the submissions is around formalising the way consumers can say
what is the value of this drug to them outside of the actual clinical evidence
that the companies are well positioned to place and from doctors who have used
the drug? What do they see the value to patients as? In Canada they have a way
that that is taken into formal consideration through the process.[87]
3.77
Cancer Action Victoria told the committee:
Cancer patients are important stakeholders who should have a
greater involvement. While the Australian system provides for consumer
representation on the PBAC, and allows for consumer input in relation to
individual products, the opportunity for the consumer voice is limited.[88]
3.78
Cancer Voices Australia emphasised the importance of greater involvement
of consumer organisations:
This is a compelling reason for greater input from consumer
organisations when PBAC is making approval decisions, especially as Australia
has little post-marketing surveillance of disease-control effectiveness or the
maintenance of good quality of life. We recommend that cancer consumer groups,
such as Cancer Voices and the Australian Cancer Consumer Network (a new network
of 30 cancer consumer groups), be consulted to obtain the broad view of the
many.[89]
3.79
In its White Paper, CDA noted the need for more meaningful engagement
with consumer groups by the PBAC, together with greater visibility and
transparency of PBAC processes.[90]
CDA recommended that the PBAC improve and increase its communication with
consumers and consumer groups, including through social media, and provide
improved guidance on how to make submissions, how submissions are used and how
decisions are made.[91]
3.80
CDA also noted that cancer patients and consumer organisations feel
significantly underrepresented, detached and disenfranchised from the PBAC
assessment process, 'despite being the actual end-users of the medicines and
being best placed to make judgements on the impacts of medicines'. To address
this, CDA recommended the establishment of a consumer sub-committee the PBAC
could call on for information regarding specific conditions and the inclusion
of at least one consumer representative on the PBAC with a cancer background.[92]
3.81
In its evidence to the inquiry the PBAC outlined the steps it is
currently taking to enhance the ability of clinicians and consumers to
participate in its work. The PBAC described some of the initiatives it
considers could enhance the participation of consumers and clinicians,
including increased transparency throughout the system and improving the level
of information available to consumers and patient groups. The PBAC noted that
consumers and patient groups are currently hampered in their ability to find
out what is on the agenda for PBAC meetings and to access important detail in
relation to products under consideration and acknowledged that there is no
systematic communication strategy with respect to committee recommendations.
The PBAC told the committee that it recognises the need for a more systematic
approach to communicating committee recommendations, appropriately tailored to
consumers, while still maintaining the integrity of the scientific and clinical
research that underpins them. The PBAC has been working with DOH to address
this.[93]
3.82
The PBAC submitted that the current emphasis on protecting commercial-in-confidence
information does not encourage an effective discussion in the community of the
real benefits, harms and cost of new medicines that come before the PBAC. The
PBAC noted that cost and price information is systematically redacted from
published documents and consumers and clinicians do not have access to the data
provided to the PBAC. The committee heard that this can lead to a mismatch
between the information upon which the PBAC has based a decision and the
information provided in the public domain regarding a drug. Dr Hill, told the
committee:
I guess the other part of it is that there has been a lot of
literature on what happens when you look at what is reported in the public
domain in medical journals about clinical trials, compared to what was done in
the protocols or what was planned to be done in the trial protocols. So
sometimes, for example, one outcome—maybe it is response rate, maybe it is
quality of life, maybe it is something else—will be reported in the first paper
that is publicly presented on a drug. And then what the committee might see is
the complete set of outcomes, so we might see not just response rate; we might
see some survival data; we might see some harms; we might see more detailed
side effects. We might see a whole lot of stuff that is in the regulatory
dossier and that becomes part of the PBAC submission that gives us a different
perspective to that which is presented in the public domain at public meetings
and in journal papers.[94]
3.83
Dr Hill further stated:
I think it is very important that a committee such as the
PBAC that is making recommendations to the minister on potential expenditure of
public money should be able to provide all of the data that it sees in the
public domain and if necessary say that we see an effect on X that looks like a
20 per cent effect, whereas what is being reported is an 80 per cent effect. I
think it is incumbent upon good quality decision-making to be able to present
that information.[95]
3.84
At its March 2015 meeting, the PBAC piloted a new process of consumer
and patient hearings on selected applications, prior to the meeting. The PBAC
heard presentations from consumer groups for Hepatitis C, melanoma, chronic
lymphoma and inflammatory bowel disease.[96]
In July 2015 the PBAC convened a second consumer hearing on biosimilar
medicines in the context of its consideration of applications at its March and
July meetings.
3.85
The PBAC told the committee:
For the first time, these hearings allowed a direct
conversation between the PBAC and patient groups about the benefits and harms
and costs of some of the medicines on the Committee agenda. Both the PBAC and
patient groups found these discussions extremely informative. Equally, the PBAC
members were concerned to hear directly that the perceived benefits from some
of these new drugs were completely at odds with the evidence that was in
company submissions.[97]
A role for formal consultation
mechanisms
3.86
Submitters noted that more formal mechanisms for capturing stakeholder
input could play a significant role in evaluating questions of quality of life
and value in the assessment of cancer medicines and could help to ensure that
the assessment of a new medicine for subsidisation incorporates the views of
the patients, their clinicians and the broader society.[98]
MA submitted:
The community has little voice in the system that it relies
upon to measure the value of life and the additional value new cancer medicines
provide to the public. ... This contrasts with the UK where there was widespread
debate following the approval of sunitinib in the UK in 2008/9 which resulted
in NICE's review of their current process in regard to assessing the value of
cancer medicines and adoption of new criteria, which included an increase in
ICER threshold deemed acceptable by NICE. (Rafferty, 2009) Australia has not
yet had a meaningful debate about the value of life, including 'end of life
care', and what the community considers acceptable.[99]
3.87
The PBAC also identified a need for more formal discussion around
community values and opportunity costs associated with health expenditure:
There needs to be a frank and complete discussion between the
community and pharmaceutical manufacturers about what the Australian community
expects in terms of benefits and harms of new medicines, balancing early access
uncertainty, and understanding opportunity cost compared to other use of the
same health care resources and the community's willingness to pay. The PBAC
could then reflect these values and preferences accurately in its assessment
and recommendations.[100]
3.88
Evidence to the committee noted the benefit of various models of formal
community engagement used overseas as part of HTA and suggested that Australia
could draw on this experience. Takeda submitted that formal mechanisms such as
these offer the ability to account for attributes associated with a medicine
that are beyond the narrow terms of 'survival' and 'cost'.[101]
Mr David Pullar, representing Roche Products, told the committee that citizen's
councils offer a means of balancing the academic rigour of the PBAC process
with consideration of social and ethical questions:
What we see is: the PBAC are technical experts in health
economics, medicine and related fields; they are not necessarily representative
of the broader community when it comes to making social and ethical judgements.
So what we have seen has worked well, particularly in Ontario in Canada, and in
the UK, with these citizens' juries, is: they are asked those social and
ethical questions. The PBAC will look at the data and they will then have to
translate that into a prioritisation: 'This works this well; it delivers these
benefits; here is what we are willing to pay for that, and here is how we trade
that off against other medicines we could spend money on.' So what a citizens
council could look at is: end-of-life care versus early intervention; treating
a rare condition that may be disadvantaged at the expense of maybe a large
population. So it is those social and ethical judgements, where it really is up
to the community to have a voice, where we think they would play in, and that
would complement the economic and clinical analysis.
3.89
MA outlined measures adopted in the United Kingdom (UK) to facilitate greater
stakeholder involvement:
The UK has also invested heavily in processes to place the
public and patients at the heart of decision-making through stakeholder
involvement in order to better capture the community's experiences and needs.
Members of the public now sit on the NICE Board; patient representatives
provide input to technology assessments and are involved in guideline
development in addition to the establishment of a Citizen's Council.[102]
3.90
The UK Citizen's Council (Council) is a panel of 30 members of the
public, chosen to reflect the demographic characteristics of the UK.[103]
The council meets annually to consider issues requiring value judgements
identified through the activities of NICE's advisory bodies.[104]
The Council is intended to provide NICE with a public perspective on
overarching moral and ethical issues. The Council's recommendations and
conclusions are incorporated into social value judgements and, where
appropriate, into NICE's methodology.[105]
3.91
Council members meet annually for two days at a time. The Council's
discussions are arranged and run by independent facilitators and are open to
public observers. During the meetings, Council members listen to different
views from experts on a topic and undertake exercises which allow them to
examine the issues in detail and thoroughly discuss their own views. The
members' views and conclusions are captured by an independent rapporteur and
the report is circulated to members for comment and amendment before
finalising. After a meeting, the report is made available for public comment. A
summary of these comments along with the report are then presented to NICE's
board for discussion.
3.92
MA also noted the success of the pan-Canadian Oncology Drug Review
(pCODR) process in capturing the input of all stakeholders:
The pCODR process was considered successful, partly because
of the inclusion and meaningful involvement of all stakeholders; transparency
and rigour of HTA process and decision making criteria; together with
incoproation of broad-based considerations of societal and patient value. The
pCODR model reflected a deliberate decision to adopt a stakeholder focussed
approach with cancer and to overcome challenges faced in HTA. pCODR delivered
high quality, practical, scientific advice that squarely addressed the issues
raised by patients, clinicians and cancer agencies that were unable to be
addressed under conventional HTA approaches.[106]
3.93
The committee notes that pCODR has been integrated into the Canadian
Agency for Drug Technologies and Health (CADTH), but understands that it has
retained its emphasis on incorporating stakeholder input throughout the
assessment process.
3.94
pCODR takes account of evidence from patient groups, drug manufacturers,
clinician-based tumour groups, and the pCODR Provincial Advisory Group. CADTH
notifies patient groups at the outset of a pCODR review and invites them to
provide input. This step is intended to capture patients' experiences and
perspectives of living with a medical condition for which a drug under review is
indicated, their experiences with currently available treatments, and their
expectations for the drug under review.[107]
3.95
Patient values are also considered in the deliberations of the pCODR
Expert Review Committee (pERC) which includes patient representatives alongside
clinicians and economists. An interview with patient representatives of the
pERC suggests that patient perspectives are genuinely considered alongside
economic, clinical and implementation considerations and illustrates the
capacity of a forum such as the pERC to balance competing perspectives in
funding decisions:
JSH: I want to go back to the patient values quadrant.
Some people might cynically say, "They spend time on it, but do you really
think it matters?" Can you think of an example [in which] you feel that
that quadrant made an important contribution to a recommendation that the
entire committee made?
Response: One example for me was when I could see the
sense of the table shifting as we focused on the patient reports about their
experience with the disease, their experience with the drug and the difference
that the drug was making to their quality of life. The difference, in the
presentation from the economic guidance report, was a small difference, but I
think it became clear to the table, looking at the patient input that, in fact,
it was a substantial difference to patients. We were looking at a small increase
in progression-free survival, but in the eyes of the committee, the benefit of
reducing a very unpleasant side effect was recognized to be more significant in
terms of the difference it made in quality of life: more than just applying
that small difference in progression-free survival would usually suggest in the
decision matrix that we're faced with. It made a real difference to the final
recommendation.
Response: I can remember a time talking about a
certain drug and a side effect. The side effect profile wasn't drawing too much
attention, and a patient member spoke up and said, "Whoa, I’ve had that.
That's really nasty. And, if there's a drug that has a similar cost and a
similar benefit and can avoid that side effect, we should be thinking about
that."
JSH: Do you think it's worthwhile considering the
economic evidence, or do you find [that] it’s not really that useful?
Response: In the system we have, many treatments we're
providing are going to be paid for, by and large, by the public purse.
Response: And, every time you pay for x, you can't pay
for y. I value the general practitioner's perspective on perc because of the
reminders that there’s a world out there besides cancer, and if we spend x
amount of money on oncology drugs, it may come out of mental health or heart
disease or something else, and we need to be reminded of that, because we're in
the cancer bubble.[108]
Committee view
3.96
The committee notes the significant challenges associated with assessing
the cost-effectiveness of cancer medicines. The increasingly targeted nature of
cancer treatments, often delivering significant but incremental improvements in
patient outcomes, combined with the fact that cancer medicines are generally
more expensive than non-cancer medicines is a significant test for the PBS.
3.97
Funding decisions must also be equitable and robust. The committee recognises
that the methodologies employed by PBAC seek to establish a level playing
field. Cancer patients and non-cancer patients alike, must have confidence that
decisions are based on a rigorous examination of appropriately robust clinical
data. At the same time, the committee recognises that such an approach can, in
itself be inherently time consuming.
3.98
The committee notes calls for the adoption of a more flexible approach
to the evidential requirements of the system to address the challenges
associated with assembling clinical data in relation to cancer medicines. The
committee considers that greater formal emphasis should be placed on quality of
life considerations within the PBAC process and understands the challenges this
presents. The current review of the PBAC Guidelines offers an opportunity to
examine the issues raised regarding the PBAC's cost effectiveness methodology
in closer detail in consultation with all relevant stakeholders. At the same
time, consideration should be given to avenues for facilitating more formal
discussion regarding community values and health expenditure.
3.99
The committee also notes calls for consumers and clinicians to play a
more central and substantial role in the evaluation of new medicines. The
committee recognises the PBAC's commitment to improving the effectiveness of
its engagement with clinicians and consumers and the steps it is taking,
together with DOH, to improve the transparency and accessibility of the
process.
Navigation: Previous Page | Contents | Next Page