Pathways to supported living within the community
The main drivers of indefinite detention in the Northern
Territory are the lack of a forensic mental health facility; the shortage of
supported accommodation options and appropriate outreach support; and a lack of
support for families and people with disability, particularly in remote
Aboriginal communities.[1]
Introduction
5.1
The preceding two chapters have examined the front-end of the justice
system where people with cognitive and psychiatric impairment first interact
with courts and the experiences of these people within the prison system.
5.2
This chapter examines pathways to supported living for forensic patients
from when an order is handed down by a court; and also transition options for
those currently being detained in prison.
5.3
As noted in Chapter 3, courts and review processes tend to err on the
side of mitigating risk to the community at the expense of providing the least
restrictive method of detaining a forensic patient. Evidence to this inquiry
has shown that, too often, particularly in Western Australia (WA) and the
Northern Territory (NT), the risk to the community becomes the paramount
consideration resulting in people being indefinitely detained in prison. The
Chief Justice of Western Australia shared his thoughts on risk management and
the restrictions inherent in the Criminal Law (Mentally Impaired Accused)
Act 1996.
If, as I suggest, the focus ought to be on risk management,
then the problem is that, because of this diversion away from that system, risk
is not being managed. There is just a short-term prison sentence or a fine that
will never get paid and, no, the problem is not addressed. Whereas a properly
designed system would identify people who need management and manage them in a
way that would address risk and, hopefully, manage them in a way that is least
invasive in the sense that it involves the least interference with their right
to live a normal life within the community so that again, as we say throughout
the system, custody ought to be an absolute last result. The problem is where
you do not have any middle ground—it is either unconditional
release or custody—you get to custody much quicker than you would if there were
some opportunities in the middle.[2]
5.4
The committee is cognisant of the need for an appropriate balance to be
struck between community safety and provision of the least restrictive
environment for this vulnerable group. Notwithstanding this, the committee has
earlier stated its view, in Chapter 3, that prison is not an appropriate place
for a forensic patient. So, if law reform which provides a middle ground for
the judiciary is made available—consistent with the Chief Justice of WA's
comments above—what are the alternative forensic pathways to prison and what
are the pathways from prison to the community for forensic patients.
5.5
Previously, in this report, the committee has noted evidence from the Aboriginal
Disability Justice Campaign that the 'bones of a functioning forensic system
exist' in the NT. Arguably, the same could be said for WA. The committee has
received evidence about and visited the Complex Behaviour Unit within the
Darwin Correctional Precinct (DCP) (described in Chapter 4) and The Cottages
adjacent to the prison (described later in this chapter); the Secure Care
Facility (SCF) adjacent to the Alice Springs Correctional Centre (described
later in this chapter); and the Bennett Brook Disability Justice Centre (DJC)
in Perth (also described later in this chapter). This evidence and subsequent
site visits have informed the committee's understanding of the transition
pathways as they currently stand. These facilities—how they are structured, who
operates them and where they are—and the subsequent lack of 'access to safe and
affordable housing' in the community for forensic patients to transfer to is at
the heart of why forensic patients are being indefinitely detained.[3]
5.6
The committee agrees that the 'bones' of a forensic system are present
in the NT and WA, but that significant work remains to be undertaken to fashion
these pathways and facilities into real supported living outcomes for people on
forensic orders. This chapter looks broadly at some of the problems highlighted
by submitters and puts forward the committee's views on the path forward,
including:
-
the failure to plan, including individual support plans,
supported accommodation and the role of the National Disability Insurance
Scheme (NDIS);
-
the departments that are responsible for providing therapy and
support for forensic patients;
-
culturally appropriate care; and
-
an early intervention approach.
Failure to plan
5.7
Submitters to this inquiry have described forensic patients held
indefinitely in prison as resulting from a 'delay in developing, or a failure
to develop' a plan for these patients. The failure to plan leads to 'custody by
default'[4]
in the first instance, and then a lack of further planning can exacerbate the
likelihood of extended indefinite custody. Mr David Woodroofe from the North
Australian Aboriginal Justice Agency (NAAJA) explained:
I can say that I think the failure to plan stems throughout,
as they say, the journey of a mentally ill person in the Northern Territory—the
failure to plan so that they do not go into the justice system and the failure
to plan for having appropriate testing and identification, whether it is at the
first one contact, such as interactions with the police and first interactions
with the courts. It is the failure to plan for getting people out on bail, and
the services and supports people need. Obviously, the ultimate and key issue
now is the failure to plan for the regular reviews, as we are pushing for. You
have strict limits that people have to plan for, but there should be a default
position that a person will be released.[5]
5.8
Mr Woodroofe elaborated on this failure to plan in an answer to a
question on notice to the committee:
It has been our experience that for 3 clients under custodial
supervision orders that there still exists either a lack or inadequate
committed long term planning in equipping suitable persons, family members or
remote communities with the skills, supports and access to resources for
clients to transition to their original home...
I can only recall one example of where there has been an
escort visit of 1–2 days for a person to their home community.[6]
5.9
Ms Sally Sievers, the NT Community Visitor told the committee that
transition planning for people held in the NT was not adequate to facilitate
people to transition from the Secure Care Facility to the community:
What was really clear to us, as soon as we went in there, was
this issue of transition planning. Secure care is not supposed to be the final
place where all these people who go through it end up...
But it was really clear, even when we first went in, that the
documentation that was being prepared and the positive behaviour support plans
for these people had not identified that actually this is the start of their
journey and our aim is to upskill them and they are to end up out in the
community in the least restrictive environment that they possibly can. That
concern has continued for the past three years during which we have reported on
the secure care facility—that the documentation that is prepared and the
therapeutic program that is provided to people is not skilling them up with
enough clarity and purpose for them then to be released into supported
accommodation in the community. That is an ongoing concern—that in fact this
was never meant to be the final destination for people. And of the number of
people who have gone through, only one has gone out into the community; one
person has gone back into custody at the CBU [Complex Behaviour Unit] in
Darwin.[7]
5.10
This section discusses deficiencies around planning and implementation
in relation to individual support plans, the lack of supported accommodation, and
the role of the NDIS for forensic patients.
Individual support plans
5.11
As noted earlier, the purpose of a behaviour support plan or individual
support plan (ISP)[8]
is to provide treatment and support options to facilitate the transition of a
forensic patient from prison (or a secure care facility) to supported living in
the community. A key concern around this approach is that it is based to
address psychiatric impairments which can improve with therapeutic
intervention. Cognitive impairments do not respond to therapeutic intervention
in the same manner, and such people will therefore never reach the recovery
level required to transition to lower security accommodation options.[9]
5.12
In its submission to the committee, the NT Government noted that:
Treatment plans providing for clinical services and support
are in place for all supervised persons who are subject to Supervision Orders.
It is the overriding objective of treatment plans to rehabilitate all
supervised persons safely to a less restrictive situation and ultimately to the
community. It is acknowledged that some supervised persons are likely to remain
on some form of supervision order for their lifetime, due to the complexities
of their case.[10]
5.13
In WA, Dr Ron Chalmers of the Disability Services Commission noted that
the Bennett Brook DJC utilises a 'flow-through model, so from the day that
someone is placed in the centre, we start working to get them out of the centre'.[11]
5.14
Despite this intent, the committee has received evidence suggesting that
ISP's are not working for forensic patients who are indefinitely detained in
prison. Mr Russell Goldflam, President of the Criminal Lawyers Association of
the NT noted that:
Individual care plans are in use in the Northern Territory
with persons on supervised orders—both custodial and non-custodial—but often
they appear to be more in the nature of a tick-a-box form filling exercise than
an effective tool to manage the rehabilitation and care and supervision of the
client.[12]
5.15
The committee received evidence that individual (behaviour) support
plans do not work where a forensic patient is detained in prison, because of
the overlap between different departments—primarily disability and corrections—with
vastly different philosophies and approaches to people within their care. Patrick
McGee, Convenor of the Aboriginal Disability Justice Campaign submitted an
example of the breakdown in the implementation of an ISP:
It was a really good behaviour support plan that did
everything that it should have done, but there are a couple of things about
that. Firstly, the disability system constructed the plan, but it was
completely and utterly overridden at any time by the wishes and the policy requirements
and the resource issues of the department of corrections. One of those issues
was the management of his behaviour and the use of restraint. It is hit and
miss in that you can have a system that does not work very well but then allows
for these spontaneous and individualised moments where something great happens,
or you can have a system that is supposed to work but is not properly
resourced, so you do not get the sustained outcomes that these people need.[13]
5.16
Mr Patrick McGee, also noted that there is confusion about who is
resourced and responsible for delivering aspects of an ISP for forensic
patients held in prison:
It is hard at the moment because the assumption from the
department of corrections is that Disability will provide this support and the assumption
from Disability is, of course, that Corrections will provide the support. At
the end of the day it has always been Disability that has been called upon by
the courts, by Corrections, by the prisons, to provide whatever support is
needed whilst the person is in prison. I think probably Victoria has gone
beyond that somewhat, but most of the states and territories do not. So it is
individualised, not systemic; the outcomes do not seem to be learned from and
drawn upon in terms of understanding what else to do, and there are no
connections between the various different parts of the system that might play a
part in getting those programs and activities and supports into the prison in a
regular way that leads to sustained outcomes.[14]
5.17
The NT Community Visitor Program (CVP) highlighted that leadership or
responsibility paralysis can even occur within departments:
The CVP has observed that clients receiving services from
different areas of the Department of Health can find themselves in a position
where there are no clear lines of responsibility or leadership for resolving
their community accommodation needs. In one instance, a young person with a
cognitive and psychiatric impairment has been detained for a number of years in
a mental health facility while these issues remain unresolved. The mental
health and disability needs of this client are such that release from
involuntary detention poses unacceptable risks, however the discharge
destination with appropriate support cannot be agreed by all relevant agencies
involved in this care.[15]
5.18
In WA, the committee received evidence from Ms Chelsea McKinney, Manager
from WA Association for Mental Health, that some of these barriers are being
broken down, with the WA Disability Services Commission providing a more active
role in delivering services in prisons:
There have historically been many problems with people being
provided with treatment from or support from any agency other than the
Department of Corrective Services. In recent years, that has improved with the
Disability Services Commission coming to the party. Their hand was kind of
forced.[16]
5.19
Unfortunately though, where individual support plans do exist, many are
not working—that is, not facilitating transition to the community—due to an
absence of clear objectives with a specific target of providing the support
people need to transition to less secure accommodation, as opposed to a
generalised risk assessment approach. Ms Felicity Gerry noted:
That is exactly what I was trying to say about general health
care. The through plan is part of that. If the long-term goal is to get
somebody out and living independently in the community then you have to work
towards a plan for enabling that to happen. Currently that does not happen. The
question is, 'Do we still keep this person here?' rather than, 'How do we make
sure that this person can live independently in the community?'[17]
Committee view
5.20
Individual support plans form a critical element of transitioning
forensic patients from prison (or secure care) to living in supported
accommodation in the community. The committee acknowledges that such plans are
being developed for most forensic patients; however, questions some of the
fundamental components that underpin these individual support plans.
5.21
The committee notes that all ISP's should be predicated on the clear
objective of transitioning a forensic patient to supported living in the
community, or from prison to secure care. Clear lines of responsibility for the
different departments must be underscored within the ISP, so it is clear how
services and supports will be delivered, particularly where the lines of
responsibility can be blurred such as between corrective services and
disability services. The committee's view on which department is best placed to
care for forensic patients is outlined later in this chapter.
Lack of supported accommodation
5.22
Many submitters and witnesses have highlighted the shortage of supported
accommodation as a critical impediment to ending the indefinite detention of
forensic patients within the prison system.[18]
The Principal Community Visitor for the NT submitted to the committee that:
We have a real dearth in the Northern Territory of supported
accommodation options. This has been an issue of concern for the Community
Visitor Program for the decade before secure care came online. They monitored mental health
facilities. It has always been a problem that there has been no step-down
facility for people in mental health facilities, so people stay in secure
settings for much longer than what is necessary. What has become even more
obvious with secure care is that they are in secure care and the planning for
them to move into the community becomes stuck by the fact that there are
actually no supported accommodation options. [19]
5.23
In an answer to a question on notice, NAAJA pointed out that in the NT:
a court cannot commit a person to an 'appropriate place' (or
provide for a person to receive treatment or services in 'an appropriate
place') unless the court has received certificate from the CEO (Department of
Health) stating that facilities or services are available in that place for the
custody, care or treatment for that person.[20]
5.24
The committee understands that Golden Glow Nursing is the only
non-government provider of supported accommodation for forensic patients in the
NT. Ms Maureen Schaffer, Director of Golden Glow Nursing noted that there is a
significant waiting list to enter their programs due to a lack of
infrastructure. In many cases, forensic patients with more complex needs are
the ones who are being denied placements.
We have a bit of a waiting list for clients. They are always
phoning us—especially form Cowdy Ward—to see if we have got any beds. There are
some clients that we have not been able to accept, because they cannot fit in
with the clients that we have got. If we had a different infrastructure
available, they could go there, but, at the moment, it just will not work. They
have been out on trial and for some reason they are the wrong skin group, they
do not like each other to start with, they already know they do not like each
other or something has happened in the past and they remember that. Other
times, if they sit down and share a smoke, we know it is going to be okay. They
will talk and give permission for that person to come and live with them for a
while—until things go pear-shaped a little bit.[21]
5.25
The lack of supported accommodation options is driven in part by state
governments that are not planning for the needs of forensic patients. The
Principal Visitor (NT) recommended that an audit be undertaken to assist with
infrastructure needs and planning:
I would be asking for an audit of needs in the Northern Territory
for supported accommodation, both for people who are in the mental health
facilities and for people who are in secure care facilities.[22]
5.26
Golden Glow Nursing highlighted the need for a range of supported
accommodation options in the community, noting that in some cases, the
conversion of residential homes for this purpose may be more appropriate and
cost-effective than purpose building large institutional infrastructures:
I think what Maureen is bringing out as well is that [Golden
Glow Nursing] actually purchase homes in the community, so people are coming to
a home. I have visited them and they are actually a home environment. If you
could purchase more homes rather than build a facility like a Cowdy Ward—it
makes more sense to have more homes based in the suburbs; most of the
neighbours would not even know, because the home is maintained like any other
normal home—that would be the way to go.[23]
5.27
The committee also received evidence at its Brisbane hearing which
highlighted the need for specialist secure supported accommodation options for
people with complex needs such as those with Foetal Alcohol Spectrum Disorders
(FASD). Mrs Elizabeth Russell noted the need for:
supported accommodation staffed by people who have accredited
training in FASD. Clearly there is a high need for secure supported
accommodation suitable for high-risk individuals who are unable to live
independently.[24]
5.28
Professor Patrick Keyzer of La Trobe University said that state governments
have an obligation to ensure that forensic patients have 'reasonable access to
a secure care facility or other supported accommodation and care and
treatment'.[25]
The ADJC agreed and recommended the need for 'accommodation and support
programs both as an alternative to prison and post-release'. The ADJC cited the
specialist forensic accommodation services utilised in Victoria and NSW as
being a practical alternative to prison.[26]
Lack of dedicated facilities for women
5.29
The committee received conflicting evidence about the availability of
non-prison secure forensic care options for female forensic patients in the NT.
Ms Schaffer of Golden Glow Nursing explained some of the complexities of mixed
sex housing in forensic units:
we have had experiences with a female requiring support in
the community, and there is absolutely no way it would be appropriate for her
to mix with males at all. There are a lot issues behind that, and if you want
to go further we can certainly go into it. But it is just not an appropriate
thing for someone with mental illness, cognitive impairment and all the social
implications that go along to be in a mixed-sex facility.[27]
5.30
The NT Community Visitor noted that the lack of appropriate facilities
for women forensic patients actually resulted in prison placement.[28]
Ms Schaffer also noted that 'there is nothing available for women in the
community', citing an example of a recent failed trial:
We did have one lady that came out on a trial into a separate
unit by herself. She kept absconding, and it did not really work.[29]
5.31
Mr Richard Campion, Acting General Manager at the NT Department of
Health (Office of Disability) acknowledged that positions in forensic
facilities largely favoured males due to their configuration, but contended
that the department made other provisions for females:
It is the case that the provision is predominantly for males
and most of the referrals that we do get are males, but we acknowledge that
there are females out there who require the support, and we have had that issue
in the past. When that has arisen, in the absence of a female-dedicated
facility, we have spot purchased. We have purchased a facility, a house,
somewhere where we can provide that service and we have commissioned staff in
that facility to support the females. So, we have not left women without the
service where it has been required.[30]
5.32
When questioned, Mr David Woodroofe of NAAJA did not know about any
properties that the department has bought in the community.[31]
5.33
The committee is concerned at the lack of secure care and community
options in general, and particularly for female forensic patients.
Underutilisation of secure care
facilities
5.34
A common theme heard in WA and the NT was about the underutilisation of
new secure care facilities. The Principal Community Visitor for the NT, Ms
Sally Sievers noted that the Alice Springs Secure Care Facility is currently
underutilised.[32]
Professor Neil Morgan, the Inspector of Custodial Services agreed, making the
point that the WA Government has focused on using the Bennett Brook DJC as a
pre-release centre rather than as a diversion option for new forensic patients.
You have talked about the Bennett Brook facility. I agree
with everything that was said this morning. It has not been used for many people,
to date. It was really designed as a prerelease facility, so we are always
going to have this issue with people who are being detained in prison prior to
being able to access that place.[33]
Committee view
5.35
It is clear that where no supported accommodation placements exist, a
person cannot be transitioned from prison or secure care to a less restrictive
environment in the community. The committee is concerned that there is a lack
of facilities that provide supported accommodation in the community.
5.36
The committee recognises that the Complex Behaviour Unit and the Bennett
Brook DJC have only recently been opened late last year and acknowledges that
there are a range of practical considerations in the commissioning of new
facilities that result in initial underutilisation. The committee also
understands, as noted in Box 5.1, that the Alice Springs Correctional Centre
has been established as a transition centre, and as such, numbers will
fluctuate as people progress into and out of the centre. Notwithstanding this,
since the opening of the Complex Behaviour Unit and the Bennett Brook DJC,
there still remain a large number of forensic patients in prison in WA and NT.
It is the committee's view that where vacancies exist in secure care facilities
that forensic patients are either transitioned from prison as a priority or new
forensic patients are simply diverted directly to these facilities.
5.37
There is a need for additional resources to be made available to build
or acquire supported accommodation options for forensic patients in the
community, particularly in regional and remote locations. Later in this
chapter, the issue of culturally appropriate care and placements will be dealt
with in more detail.
Box 5.1—Committee site visit to the Alice Springs
Secure Care Facility
Introduction
At
the conclusion of its visit to the Alice Springs Correctional Centre (ASCC) (as
described in Chapter 4), the committee visited to the Secure Care Facility
(SCF), a facility operated by the Department of Health (Office of Disability). The
SCF supports people who have transitioned from the ASCC on custodial
supervision orders. The committee was welcomed by the staff and residents of
the SCF, and provided with a short briefing and tour of the facility.
At
the time of the visit, there were two people on custodial supervision orders
(forensic orders) housed in the ASCC in G Block (John Bens Unit). G Block is a
section of the ASCC repurposed to house people on custodial supervision orders.
Seven people are currently being supported by the SCF. Six of those people live
permanently in the SCF after being transitioned from the ASCC. One of the
people living in G-Block visits the SCF three to five times a week on day trips
as part of his transition plan. Four of the people living in the SCF are being
prepared to transition into supported accommodation in the community.

Figure 1.1: A view of an outside courtyard within the
SCF
Transition to the Secure Care Facility
The
Secure Care Facility (SCF) is located adjacent to the ASCC and is operated by
the Office of Disability. The SCF provides secure, supported accommodation for
people subject to custodial supervision orders. As noted previously, transition
to the SCF commences once a person has a transition and treatment plan in
place. Subject to certain criteria being met, primarily management of violent
behaviours, a person may commence being introduced to the SCF. Depending on the
level of cognitive functioning, the starting point for transition may range
from a person being shown photos of the facility and told a story about it to
spending a few hours in the SCF, then extending to day trips. Transition is
conducted at a pace commensurate with the person's capacity to process changes
in their physical and social environment. Subject to the transition process
being successful, a person could be expected to move into and live in the SCF.
It is expected that people can over time then be expected to move into and live
in supported accommodation in the community.
Despite
being a secure facility, the SCF is a home-like environment, with televisions,
computer access, communal areas (outdoor and indoor), kitchen and private
individual rooms. Access to vehicles and the capacity to undertake chaperoned
community visits is provided on a daily basis. Freedom of movement is generally
not constrained. Disability Support Workers (DSW) provide day-to-day support in
the SCF at a ratio of two workers to one patient. DSW work closely with
patients to meet the objectives of their plans; whilst access to medical professionals
is also provided.
Role of the NDIS
5.38
The committee has received some evidence suggesting that prisoners or
people in prisons are not eligible for support under the NDIS. At the Canberra
hearing, the Department of Social Services noted that people deemed eligible
for the NDIS before entering prison remain eligible for some supports and
services such as aids and equipment after entering prison. However, in
presenting evidence to the committee, the department did not provide clarity on
whether 'allied health and other therapy directly related to their disability...including
for challenging behaviours' is provided for under the NDIS or becomes the
responsibility for the relevant corrective services department. Furthermore, it
was not made clear to the committee by the department whether someone not
evaluated for the NDIS prior to entering prison may seek an eligibility
assessment (and be approved) for the NDIS after entering the prison system.[34]
This is particularly concerning in light of evidence received and examined in
Chapter 4 regarding the lack of diagnosis and therapeutic support options
available within prisons.
5.39
The NSW Council for Intellectual Disability has noted that:
The NDIS provides an opportunity to provide reasonable and
necessary disability support to people with criminal justice involvement. This
will only occur if there are strong outreach, engagement and linking systems to
support individuals into the NDIS.[35]
5.40
In its submission, NSW Council of Intellectual Disability described the
Community Justice Program (CJP) trial being operated in the Hunter Valley in
NSW. This trial seeks to provide 'a small number of offenders with intellectual
disability' with 'disability support for the first time through funded
packages'. Although this trial was commended for utilising 'best practice' to
'support some of its clients to see the potential benefit of accessing the
NDIS, go through the NDIS processes and achieve positive participant plans',
only three people had been placed by April 2016. The Barwon trial site in
Victoria was highlighted as having worked better due to working with 'a
long-standing "justice plan" arrangement between Victorian justice
and disability agencies'.[36]
5.41
In November 2016, in an answer to a question on notice, the Department
of Social Services provided a brief summary of the CJP's progress and indicated
slightly higher participation rate, but still only half the expected number:
In February 2015, FACS [NSW Family and Community Services],
CJP and the National Disability Insurance Agency (NDIA) agreed to utilise the
CJP as a pilot to oversee the transition of CJP clients into the NDIS during
the Hunter Trial. Two providers were identified to provide support for 20
people who were due to transition to the NDIS. Ten of those people achieved an
approved plan during the pilot.[37]
5.42
There are other concerns more generally with the NDIS. The committee heard
evidence from Developmental Disability WA that there are groups of people with
mild intellectual disabilities who may not be eligible for the NDIS, but who
still require supports:
The National Disability Insurance Scheme offers lots of
opportunities if we can get ways of modelling that interface right and if we
can get over the usual argy-bargy of who pays for what where. I also have
concerns though, based on the huge amount of work we are doing at the moment to
support people who are caring for people with fetal alcohol spectrum disorder,
that the reality is that there are a whole lot of people who we are talking
about who would not be eligible for the NDIS. This idea that the NDIS is going
to give full access to support pathways for people with spectrum conditions
like FASD is simply not realistic, so we need to make sure that those people
who are at the margins of eligibility for schemes like the NDIS are being
supported.[38]
5.43
The committee has also heard concern in this inquiry regarding the
withdrawal of state governments' disability services as the NDIS is being
rolled out. There are concerns about forensic patients, and other people with disability
more generally, falling through the cracks during this process. The NSW
Government was cited as an example by the NSW Council on Intellectual
Disability:
In parallel with the implementation of the NDIS in New South
Wales, the New South Wales government is exiting from service...[39]
5.44
In response, the Department of Social Services noted that:
Prior to the full nationwide implementation of the National
Disability Insurance Scheme (NDIS) under the National Disability Agreement,
state and territory governments remain responsible for non-NDIS trial site
disability services in their respective jurisdictions, including but not
limited to the provision of supported accommodation, respite, community access
and community support services.[40]
Committee view
5.45
The committee agrees with evidence that the NDIS could provide
significant disability support for people with cognitive and psychiatric
impairment in the prison system. The committee is concerned with the
conflicting evidence it has received regarding eligibility and access to
supports through the NDIS for people held in prisons. Noting not only the
cognitive and/or psychiatric impairments of forensic patients, but the
prevalence of these disabilities in the general prison population, there is a
need to better understand how the NDIS will interface with people held in
prison.
The responsible department
5.46
There are different operating arrangements for the secure treatment
facilities in the NT and WA. For instance, in WA, the declared place, the
Bennett Brook Bennett Brook DJC is operated by the WA Disability Services
Commission. Likewise, in the NT, the SCF and The Cottages, despite being
located adjacent to the DCP are also operated by the NT Department of Health
(Office of Disability). The primary facility in the NT for forensic patients,
the Complex Behaviour Unit is managed by the NT Correctional Services, with the
support of officers and medical professionals from the Department of Health
(Office of Disability).
5.47
The previous chapter has noted some of the negative aspects of placing forensic
patients in a prison environment. The committee also notes that the Complex
Behaviour Unit, when originally conceived was to be outside the perimeter of
the prison and operated by the NT Department of Health (Office of Disability). Later
design plans incorporated the Complex Behaviour Unit 'within the razor wire'
and made it 'part of the prison'.[41]
The committee has visited the Complex Behaviour Unit, and recognises and
commends the hard work and dedication of corrections officers assigned to the Complex
Behaviour Unit.
5.48
The committee acknowledges that the Complex Behaviour Unit is also used
to provide support for regular custodial prisoners who have mental health or
cognitive issues. Notwithstanding this, there is a requirement for 'a forensic
mental health facility which can provide specialist therapeutic care' outside a
prison environment in the NT.[42]
5.49
After its Darwin public hearing, the committee visited the DCP. Part of
this visit was to The Cottages. Transition to The Cottages from the Complex
Behaviour Unit is an option for those who demonstrate improved behaviour in
accordance with their treatment and transition plan and who are also deemed a
low risk to the community. The Cottages provide an intermediate form of
accommodated support between a secure location such as a prison, and living in
the community with no restrictions and limited supports. The Cottages are
operated by the Department of Health (Office of Disability). The objective of The
Cottages is to provide a supported accommodation model that allows a person to
learn or re-establish a range of life skills before potentially being
transitioned into the community into a supported living arrangement. The
committee's visit to the Bennett Brook DJC is documented in Box 5.2. The Bennett
Brook DJC has similar objectives and is operated by the Disability Services
Commission rather than Corrective Services.
5.50
In NSW, the Justice Health and Forensic Mental Health Network 'provides
health services to those in contact with the forensic mental health system and
the NSW criminal justice system'.[43]
This Network is directly responsible to the Secretary of NSW Health. Similar
arrangements apply in other states such as Victoria and South Australia.[44]
Committee view
5.51
Consistent with the committee's view in Chapter 3 and 4 that prison is
not a suitable place for forensic patients to be held, the committee also
considers that secure care facilities—such as the Complex Behaviour Unit —should
be operated by the relevant disability department rather than corrective
services. It is the committee's view that a therapeutic approach, rather than
punitive, is more likely to lead to behavioural improvements which are
consistent with a reduction of risk that will ultimately lead to less
restrictive accommodation options for forensic patients.
Box 5.2—Committee site visit to the Bennett Brook
Disability Justice Centre
Introduction
Following
the public hearing in Perth on 19 September 2016, the committee visited the
Bennett Brook Disability Justice Centre (DJC) in the Swan region of Perth. The
committee was welcomed to the DJC and provided with a tour by Ms Myra Parry,
Manager of Disability Justice Services and staff of the DJC.
Until
late last year, one of the reasons that people subject to forensic orders were
being indefinitely detained in WA prisons was the lack of a 'declared place' or
a DJC—a secure alternative to prison where therapeutic and other support
services can be provided. This has now been partially rectified with the
construction of the state's first declared place, a ten bed facility. The DJC
is operated by the WA Disability Services Commission (DSC).
Description of the facility
This
purpose-built secure facility consists of a ring of buildings built around a
central courtyard with paths, basketball court, vegetables gardens and shared
social spaces including a firepit. The buildings surrounding this area consist
of apartments where the residents live, a common amenities area with kitchen,
laundry, lounge room, games facilities and computers; a workshop with
woodworking tools; and an administrative area with observation rooms, meeting
rooms, medical rooms and staff offices.


Figure 1.1: An aerial view of
the DJC at Caversham showing the buildings situated around a central courtyard;
and view across the central courtyard area to the administrative and activities
buildings
Placements in the facility
Placements
in the DJC are limited to people with cognitive impairments subject to custody
or forensic orders. Placement can only be recommended by the Mentally Impaired
Accused Review Board (MIARB). Residents are selected on the basis that they
will be suitable to transition to live in the community. Similarly, any leave
of absence or separation from the DJC can only be approved by the MIARB.
Support provided in the DJC and
pathways to the community
DJC
staff and external private service providers support residents to live independent,
positive and purposeful lives in the centre and in the community on leave of
absence. Leaves of absence are an opportunity for residents to spend extended
periods of time living in the community. Residents are transitioned to
independently live and manage their own home (e.g. cooking meals, washing,
cleaning) and engage in social activities with positive friends and
acquaintances. A staged and supported transition back to the community ensures
that this transition to the community is sustainable for that individual in the
longer term.
Progress so far
Since the DJC's opening late last
year, two residents have successfully transitioned back into the community; two
residents currently live in the DJC; and three prospective residents are being
considered for placement. In evidence to the committee, the DSC suggested that
the centre will be close to full capacity by the end of this year. During the
tour, committee members were able to meet with two current residents. DJC staff
noted that there had been a vast improvement in the social interactions and
functioning of the residents since moving to live in the DJC.
Culturally appropriate care
5.52
The committee has received evidence that there needs to be greater
involvement of Aboriginal and Torres Strait Islander support workers in the
journey of Aboriginal and Torres Strait Islander peoples subject to forensic
orders. The Aboriginal Disability Justice Campaign (ADJC) noted its concern
about the 'lack of culturally responsive service systems' for Aboriginal and
Torres Strait Islander peoples.[45]
The Aboriginal Legal Service of Western Australia outlined why culturally
appropriate care is important.
...if things are going to improve there needs to be a greater
involvement of Aboriginal people in helping these people. If you get
blackfellas involved—ideally where people are on country, but where they are
surrounded by people from their own community who they trust and who they have
a rapport with—that is a hope for the future. So often what I find in my job at
the ALS is if you have non-Aboriginal people dealing with these people things
go off the rails in a heartbeat. We are continually confronted with
pre-sentence reports done on these people and other clients—psychological
reports—which are indescribably damning about the client and very seriously
adversely affect their prospects in terms of the disposition that a court may
impose.[46]
5.53
A lack of rapport and cultural understanding between Aboriginal and
Torres Strait Islander peoples and non-indigenous support workers often results
in extended detention and a person's underlying disability remaining
undiagnosed. Mr Peter Collins, Director at the Aboriginal Legal Aid Service of
Western Australia (ALSWA):
On the boy that I acted for between the ages of 10 and 18
from the East Kimberley, the reports would routinely come back in terms of him
being defiant, uncooperative, unwilling to listen—all of those things. Well, he
had [Foetal Alcohol Spectrum Disorders] FASD. But, in terms of the compilation
of those sorts of reports, the issue is there is no rapport established, there
are often language difficulties, and Aboriginal interpreters are never used to
assist in the compilation of these reports, so these people are at
cross-purposes absolutely with the clients, and then it dovetails further down
the track. So I am very strongly of the view and very passionate about the need
for the involvement of Aboriginal people in assisting, assessing and so on with
these people—in a culturally appropriate way, obviously.[47]
5.54
Mr David Woodroofe from the North Australian Aboriginal Justice Agency
noted the issue of cultural and language communication issues were brought up
in Alice Springs. The demand for culturally appropriate signing supports is
simply not being met.
That has been a key learning thing for our organisation.
NAAJA itself literally today in Oenpelli is working with an Auslan interpreter
on assessing a person and establishing communication and obtaining
obstructions. NAAJA has also worked with cognitive impairment and also deafness
where one of the key gaps in the Northern Territory with Auslan is the fact of
Aboriginal signing and community signing. There are 55 signing languages in
Australia and in the Northern Territory there eight key groups. You can have
community signing and individual or family signing so one of the key gaps in
the service in the Northern Territory has been relay signing or and Aboriginal
cultural broker signing. I can recall a most fascinating and powerful case
where we had a person with hearing loss and also with cognitive issues. A
family member from their community was signing and assisting, we had Ms Jodie
Barney, who was the Aboriginal relay interpreter, and then we had an Auslan
interpreter so we had in fact three people involved. That can be the level of
complexity that an individual person has so obviously they are very resource
intensive proceedings but sometimes it is imperative that you go to that level.
It is clear that we do not have the level of support to the lengths we wish we
could have in servicing remote regions in particular.[48]
5.55
NAAJA also noted that the:
Northern Territory could and should be taking a lead—for
example, by developing NT Indigenous-specific cognitive tests; or culturally
relevant materials for psycho-education. It is also important for such
materials to be developed given the very high staff turnover experienced by
many professions in the NT, including health.[49]
5.56
Mr Joseph Knuth of Danila Dilba Health Service was quite direct in his
advice to the committee:
The only way you are going to fix the cultural understanding
is actually employ Indigenous people to be in those positions. Give them the
skill sets to be able to do it.[50]
Pathways to country
5.57
The committee has heard evidence about the locations of secure care
facilities such as the Bennett Brook DJC. Although there were mixed opinions on
facilities such as the Bennett Brook DJC, many witnesses agreed that the
establishment of the state's first declared place is a step in the right
direction in WA.[51]
As a first step, the establishment of the Bennett Brook DJC in the Perth
metropolitan area makes sense; however, greater consideration needs to be given
to where the next declared place will be. The WA Inspector of Custodial
Services observed the following about geographical demand for placements:
I also have a fundamental problem, and it is this: the
declared place that we have set up is in Perth; it is a metropolitan place.
When you look at the backgrounds of the people who are caught by the act, lots
of them are not from Perth. So what is the point of a prerelease facility in
the metropolitan area for people are going to go back and live in the Kimberley
or the lands. So it does not meet the needs of all of the cohort. It is also
going to be very difficult, if not impossible, in my view, to set up adequate
declared places, given the gender, male-female; the age differences; the
cultural differences; and, with some of the people who are caught by the act,
the issues around sexual behaviour. It would be very difficult to manage the
large cohort of different need. So I welcome the centre, but as I say I have a
fundamental difficulty as to whether a Perth based declared place, or two, is
really going to meet the cohort that we have.[52]
5.58
Mr Peter Collins of ALSWA concurred, noting that transitional forensic
facilities need to be made available closer to the home communities that people
will transition to:
Consider the need for more regional and remote declared
places
If these centres could be located in regional areas all the better, in my view.
For example, I have acted for a client from
a community called Tjuntjunjara. Tjuntjunjara is probably one of the most isolated Aboriginal communities in Australia if not
one of the most isolated communities in the world. It is on the Northern
Territory- South Australian border, several hundred kilometres south of
Warburton, which in itself is a very isolated community. Warburton is 800
kilometres from Kalgoorlie and about 1,600 kilometres from Alice Springs.
This client was what I have described as a 'first contact
person'. He and his family had been living in the bush before they first came
into contact with non-Aboriginal people. This was in the mid- to late eighties,
from memory. He was sentenced in relation to the manslaughter of his best
friend. He was in a Perth jail and he had no visits for the entirety of his
jail sentence. He had no telephone contact. There were no video link-ups. So
these people are being locked up in Perth jails incredibly socially isolated,
and the only prospect of any interaction with someone they know is if there is
another prisoner, a countryman, who is in the same unit as them.[53]
5.59
Mr Collins recommended:
If you can decentralise these centres so that they are in
places like Kalgoorlie, Broome, Hedland, all the better because, at least, it
offers the hope that these people will get visits from family and they will
have that critical interaction with Aboriginal people, which can only help
their mental health.[54]
5.60
The other consideration raised about declared places, but that equally
applies to transitional forensic health facilities, is that they need not necessarily
be an institution or a prison. Ms Taryn Harvey of Developmental Disability WA
noted:
Depending on the nature of the support that they need and the
particular risks that they present, a declared place can be a supported
accommodation facility, for example. There is nothing in the legislation that
actually says a declared place must be an institution with 10 beds. To declare
a place is to effectively gazette it. It has to meet certain conditions in
terms of being secure and other things, but there is nothing that mandates that
it has to represent an institutional model.[55]
Committee view
5.61
The committee considers that Aboriginal and Torres Strait Islander
forensic patients should have access to culturally appropriate therapeutic and
support services. It is imperative that Aboriginal and Torres Strait Islander
peoples with cognitive and/or psychiatric impairment are able to communicate effectively
with service providers, police and the judiciary. Chapter 3 discussed programs
which might assist to improve participation for people with cognitive and
psychiatric impairment in the justice system. For Aboriginal and Torres Strait
Islander peoples, this may also require additional supports from culturally
specific aids and trained Aboriginal and Torres Strait Islander support workers.
5.62
The committee reiterates the evidence of the intellectually impaired Tjuntjunjara
man who was held over 1100 kilometres from his home in the eastern goldfields desert
country of WA. The committee considers that there is a need for more
geographically and culturally appropriate secure care facilities or declared
places that allow forensic patients to maintain connections to family,
community and country.
An early intervention approach
5.63
This inquiry has focused primarily on people with cognitive and/or
psychiatric impairment once they have come into contact with the criminal
justice system and are held in prison indefinitely as a forensic patient.
5.64
Many submitters to the inquiry have highlighted the importance of early
intervention approaches, with a move away 'from sentences to services'.[56]
The Western Australian Association for Mental Health (WAAMH) acknowledged that
'there are far too few forensic mental health beds in WA'; however, noted that
the 'investment and focus on prevention and early intervention in forensic
mental health is woefully inadequate'.[57]
5.65
The National Disability Insurance Agency (NDIA) has a critical role in
providing outreach to people with cognitive and/or psychiatric impairment and
ensuring that diagnosis and early intervention occurs as early as possible in a
person's development to ensure the necessary supports are provided. The NSW
Council for Intellectual Disability submitted that:
Through outreach and engagement and working closely with
early childhood services, schools, child protection and juvenile justice, the
NDIA should provide early intervention to children and young people with
intellectual disability who are [at] risk of lives of offending.[58]
5.66
In its submission, the Department of Social Services highlighted two
early intervention programs—the Personal Helpers and Mentors program and Family
Mental Health Support Services—that 'provide early intervention services to
assist families, children and young people up to the age of 18 who are affected
by, or at risk of mental illness'.[59]
At face value, these appear to be good programs, however, there do not appear
to be any federally funded programs which focus on people with intellectual or
cognitive impairments. In fact, those with cognitive impairments are actively
excluded from these two programs.
5.67
The NSW Government, through Juvenile Justice Australia operate:
a specific diversion program Youth on Track (YOT) to provide
early intervention support. Uniting-Care Burnside are contracted to coordinate
a range of services for 10–17 year old young people before they become
entrenched in the criminal justice system in Newcastle, Mid North Coast and
Blacktown. YOT engage young people and their families in case work and
interventions targeted at addressing the young person's individual needs.
All young people in the YOT Program are assessed using the
Adolescent Intellectual Disability Screening Questionnaire (CAIDS-Q) that
identifies whether the young person may have an intellectual disability. This
is followed up with a referral for further assessments and to disability
services.[60]
5.68
Again, ostensibly this appears to be a good program; however, the
committee questions why early intervention programs are not being made
available to younger cohorts of people. Engagement with younger people at
earlier stages of development is crucial. In its submission, the Australian
Medical Association (AMA) noted that:
Early intervention for children with intellectual
disabilities, including Foetal Alcohol Spectrum Disorder, is necessary to
improve developmental outcomes, minimise the development of secondary
disabilities, and reduce the likelihood of future involvement with the criminal
justice system.[61]
5.69
The NSW Council of Intellectual Disability highlighted the economic
sense of early intervention, which will be explored further in the next
section:
There is a net saving to governments from early action to
meet the disability support needs of potential and actual offenders with
intellectual disability rather than allowing justice systems to bear large cost
from responding to their offending.[62]
Investing in people and their
futures
5.70
There is a substantial economic cost in detaining people deemed unfit to
plead. The 2016 Report on Government Services noted that the annual cost of
detaining a person in a WA correctional facility is over $131 000. The
cost in the NT is slightly lower at nearly $118 000.[63]
This compares to the significantly lower cost of community corrections which
equates to $17 144 and $15 877 respectively.[64]
5.71
There remain questions as to whether this money is not better deployed
to therapy, housing and other supports for people with cognitive and
psychiatric impairment who should not be held in the criminal justice system
having been deemed unfit to plead.
5.72
There is a strong economic case to be made for investment in lifetime
support for people deemed unfit to plead. In an August 2013 research paper,
Professor Eileen Baldry and her colleagues highlighted a series of lifetime cost-benefit
analyses for people with cognitive and/or psychiatric impairment who come into
contact with the criminal justice system. This research highlighted that the provision
of early support and diversion services not only yielded improvements to
wellbeing and other outcomes for this group, but that for every dollar spent,
the government realised savings of between $1.40 and $2.40 over the lifetime of
this person.[65]
A case study that examines the cost-benefit analysis for "Casey" is
outlined below in Box 5.3.
Box 5.3: Cost-benefit analysis for "Casey"
quantifying the benefits of early support and diversion over a lifetime.
Casey
is an Aboriginal woman in her early 20s who has an intellectual disability and
has been diagnosed with a range of mental and other cognitive conditions,
including Attention Deficit Hyperactivity Disorder, conduct disorders,
adjustment disorders, personality disorder and bipolar affective disorder. She
has a long history of self-harm, physical abuse and trauma.
Casey's
intellectual disability and personality disorders are key factors precipitating
her very high levels of institutional contact from a young age, particularly
with police. The extreme costs of Casey's contact with the criminal justice
system are significantly reduced after she becomes a client of the NSW Ageing,
Disability and Home Care (ADHC) Community Justice Program at the age of 18.

By
age 20, Casey ends up on an intensive support package from ADHC and on
Centrelink supports, amounting to $1 million per annum. If Casey is given an early
intervention from the age of seven, that would mean she didn't offend, come
into the criminal justice system, or end up on such an intensive package,
substantial savings of up to $2.9 million could be achieved by age 20. In
another five years, further savings of up to $3.7 million could be achieved.
The
following assumptions are made in the calculation of the benefits for Casey:
-
from age 7, Casey is provided with
an intensive early intervention package of $150,000 pa
-
from age 18, Casey moves to an
increased level of support, including accommodation, of $250,000 pa
-
these supports prevent Casey from
contact with the criminal justice system and such high contact with the health
system, and mean that she does not require crisis supports from ADHC.
The
figure below compares the trajectory of Casey's lifetime cost without
investment to the lifetime cost with early intervention. The extra investment
early in Casey's life is not much more than was invested between 7 and 15 years
of age.
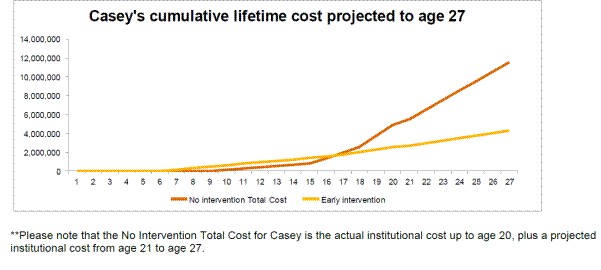
The
cumulative savings from early intervention become apparent at age 16.

Source: E.
Baldry, R. McCausland, S. Johnson, A. Cohen, People with mental health
disorders and cognitive impairment in the criminal justice system: Cost benefit
analysis of early support and diversion, August 2013, pp 7, 10.
Justice
reinvestment
5.73
In NSW, one non-government organisation is endeavouring to take an
investment approach with its justice reinvestment program, Just Reinvest NSW.[66]
In its submission to the committee, Just Reinvest NSW described justice
reinvestment:
The aim of Justice Reinvestment (JR) is to redirect funding
from the corrections system to the community to fund programs and services to
support people in the community to reduce offending behaviours and build
community capacity (Tucker & Cadora 2003). The Justice Reinvestment for
Aboriginal Young People Campaign advocates that the methodology and objectives
of justice reinvestment must be:
-
Data driven
-
Place based
-
Fiscally sound
-
Supported by a centralised strategic body[67]
5.74
An example of such an approach is the justice reinvestment project being
run with Maranguka in the north-west NSW town of Bourke. This town, which has a
population of less than 2 500 people has over $4 million spent annually incarcerating
the children and youth.[68]
The community of Bourke experiences significant economic and social
disadvantage characterised by a high Aboriginal and Torres Strait Islander
peoples population, high unemployment rates, low levels of education, and predominantly
non-violent crime.[69]
Mr Alistair Ferguson, Executive Officer for Maranguka highlighted the problem:
Kids were being taken away. Too many of my community were
being locked up. Families were being shattered, again and again, and this was
happening despite the huge amount of money government was channeling through
the large number of service organisations in this town.[70]
5.75
The purpose of the Maranguka initiative is to:
create better coordinated support to vulnerable families and
children in Bourke through community-led teams working in partnership with
existing service providers, so that together we could look at what’s happening
in our town and why Aboriginal disadvantage was not improving, and together we
could build a new accountability framework which wouldn’t let our kids slip
through.[71]
5.76
In September 2016, KPMG released a report which noted that the cost of
the Maranguka community-led initiative has an 'annual staffing cost of $554 800'
compared to the over $4 million spent on incarcerating the youth of Bourke.[72]
This initiative is still in its early implementation stage, so it is too early
to meaningfully measure outcomes, however, KPMG noted that:
When contrasted with several other crime prevention
approaches, the Justice Reinvestment approach was found to be promising on a
number of criterion. The approach has the potential to address the underlying
causes of crime, the approach is data-driven and the approach is community-led...
The development of the approach is being progressed and has
the potential to have a significant impact in Bourke.[73]
5.77
Although the Maranguka initiative in Bourke focuses more broadly
on the incarceration of young Aboriginal people, this community investment
initiative is a useful template to consider for communities in other parts of
Australia with high levels of youth incarceration. The AMA 'would like to see a greater commitment to justice
investment principles being used to fund early intervention and diversion
efforts, particularly for people with mental health problems, substance use
disorders, and cognitive disabilities, in Aboriginal and Torres Strait
Islander communities'.[74]
5.78
In its submission to the committee, Just Reinvest NSW reiterated
the work of Professor Eileen Baldry summarising the successful approach of
Justice Reinvestment.:
The evidence is stark that...early lack of adequate services is
associated with costly criminal justice, health and homelessness interactions
and interventions later...Millions of dollars in crisis and criminal justice
interventions continue to be spent on these vulnerable individuals whose needs
would have been better addressed in early support or currently in a health,
rehabilitation or community space. It is obvious that access to integrated and
responsive support services including drug and alcohol support, mental health
and disability services or other psycho-social forms of support is needed.[75]
Committee view
5.79
The committee considers the preceding section one of the more important components
of this inquiry. Much of this report has dealt with what happens and what
should happen to people with cognitive and/or psychiatric impairment once they
come into contact with the criminal justice system. Ideally, an early
intervention approach, where people with cognitive and/or psychiatric
impairment are identified and given appropriate supports, is a more preferable
pathway and outcome than attempting to divert a person once they have been
charged, are subject to forensic orders or are in prison.
5.80
The committee notes some of the programs being conducted at a state and
federal level, and commends the work of such programs. However, the committee
is concerned that such programs are not targeted at those with cognitive
impairment, and they are targeted at older cohorts of children. To paraphrase
one submitter, intervention must commence at earlier stages of development 'to
improve developmental outcomes, minimise the development of secondary
disabilities, and reduce the likelihood of future involvement with the criminal
justice system'.[76]
5.81
The committee also notes the economic sense of up-front funding and
implementation of early intervention programs to facilitate people with
cognitive and psychiatric impairment to lead full and productive lives.
Concluding committee view (Chapter 5)
5.82
This chapter has explored the challenges that face forensic patients as
they attempt to transition from prison or secure care facilities into supported
accommodation in the community.
Failure to plan
5.83
The committee is concerned that there is a failure to plan on a number
of levels. ISP's are not structured with the key objective of moving forensic
patients out of prison or secure care into the community. ISP's are also not
clear on who is responsible for the provision of services and supports. The
committee considers that ISP's must have the clear objective of providing
therapeutic (or behavioural support) which leads to a person living as
independently as possible in the community. The committee also considers that
disability services must be the lead agency to implement and provide supports
under an ISP.
5.84
There is a need to plan more effectively for the numbers of forensic
patients who need supported accommodation in the community. It is the committee's
view that supported accommodation options need to be made available to enable
forensic patients to live supported in the community. There is also a need to
better understand the role that the NDIS will play in providing supports to
forensic patients in prison, secure care facilities and in the community.
The responsible department
5.85
Consistent with the committee's view in Chapter 3 and 4 that prison is
not a suitable place for forensic patients to be held, the committee also
considers that secure care facilities—such as the Complex Behaviour Unit —should
be operated by the relevant disability department rather than corrective
services. It is the committee's view that a therapeutic approach, rather than
punitive, is more likely to lead to behavioural improvements which are
consistent with a reduction of risk that will ultimately lead to less
restrictive accommodation options for forensic patients.
Culturally appropriate care
5.86
The committee considers that Aboriginal and Torres Strait Islander
forensic patients should have access to culturally appropriate therapeutic and
support services. These services need to be provided by trained Aboriginal and
Torres Strait Islander support workers at all stages of a forensic patient's
journey. Culturally appropriate care must be made available in locations closer
to the family, community and country of Aboriginal and Torres Strait Islander
forensic patients.
Early intervention
5.87
The committee considers the need for early intervention services to be equally
important as the support provided once a person with cognitive and/or
psychiatric impairment reaches the courts and becomes a forensic patient.
Preventing a person from reaching this point through early identification,
diagnosis and provision of support services is a much better outcome than
someone remaining undiagnosed and/or unsupported and engaging with the criminal
justice system. There are a handful of programs that seek to provide early
intervention services; however, the committee is concerned at the lack of
programs to engage children with cognitive impairments at a younger age.
Conclusions—forensic orders (Chapters 2–5)
5.88
'Prisoner B' is one of thirteen forensic patients currently indefinitely
detained in a Northern Territory (NT) prison; there are fifteen forensic
patients held in similar circumstances in Western Australian prisons.
Anecdotally, there are nearly 100 people on forensic orders held indefinitely
in Australian prisons. Most are Aboriginal and Torres Strait Islander peoples;
all have severe cognitive and/or psychiatric impairments. These are some of the
most vulnerable Australians, and they are detained in the harshest of
facilities and are denied the natural justice of knowing when they will be
freed:
I am the guardian for [Prisoner B], who is detained in Alice
Springs Correctional Centre. His life was actually pretty full of tragedy and
injustice, and his life whilst he has been detained is full of tragedy and
injustice.[77]
5.89
They are ostensibly held for therapeutic purposes, but without the
necessary supports required to make a transition back into the community. Many
have lifetime cognitive impairments, yet are required to 'recover' in order to
be considered for release.
Pre-detention
5.90
The committee received a range of evidence which shows that good quality
therapeutic treatment and intervention for people with a cognitive or
psychiatric impairment is often delivered as a last-minute, crisis-induced
response, and often comes after police involvement once a person has
deteriorated to the point of being a risk of harm to themselves or others.
5.91
The committee acknowledges the weight of evidence that shows early
intervention, diversion programs, court advocacy and the use of advance
directives for people with cyclical impairment issues, would significantly
reduce the need for this belated therapeutic response. It would bring mental
health treatment in line with other branches of health service delivery, where
prevention and early intervention are universally acknowledged as better health
approaches.
5.92
The failure to appropriately divert people with a cognitive or
psychiatric impairment away from the criminal justice system is highlighted by
the evidence presented to the committee, that people are pleading guilty to
offences rather than mounting an appropriate mental impairment defence. The
committee heard people are likely to be released much faster and be dealt with
in a more regulated fashion in the criminal justice regime.
Detention
5.93
The committee has received a significant body of evidence which has
highlighted that prisons are not appropriate places for forensic patients. The
committee is concerned that the therapeutic and support needs of this
vulnerable group of people have not been met prior to an escalation of their
condition which resulted in detention. Equally, the committee is not convinced
that the needs of this group have or will be met in a prison environment. In
addition to the lack of therapeutic support, the committee is concerned that
placement of people on forensic orders in prison unnecessarily exposes them to
physical risk and to isolation—both within the prison and from the community.
5.94
The committee strongly concurs with the advice put forward by the
Australian Medical Association and the Australian New Zealand College of
Psychiatrists, that prisons are not appropriate places to hold people with a
cognitive or psychiatric impairment, and that prisons are not hospitals and
should never be viewed as such.
5.95
The committee notes evidence that forensic detention is largely founded
on the premise that a person is detained for the purpose of involuntary
treatment, and once the impairment has improved and the person is no longer a
risk, they will be released. However, cognitive impairments are generally
constant impairments, from which a person does not 'recover'. The committee is
deeply concerned with this conflation of permanent cognitive impairments within
a regime designed for people with a recoverable psychiatric impairment.
Exiting detention
5.96
The committee also has received disturbing evidence that many people
remain indefinitely detained in secure facilities, not because they are a
safety risk, but because there is no other place to house them.
5.97
Evidence has been presented that across Australia, people languish in
detention, often in harsh facilities which are counter-productive to their
recovery, simply because there is no appropriate community-based accommodation
to allow for their release. There are few issues of greater injustice, than the
continued detention of people because of a lack of appropriate spending on
disability accommodation.
Conclusion
5.98
Because indefinite detention takes so many forms and has so many causes,
there is no simple one-stop fix. It will take a concerted effort from all
jurisdictions, and will require coordination and leadership at a Commonwealth
level.
5.99
The committee acknowledges that this issue does not impact a large
number of Australians. However, the committee contends that despite being a
small population, the deeply negative impact to these Australian's lives and
human rights is one that a just society cannot accept.
Navigation: Previous Page | Contents | Next Page