Chapter 2
Out-of-pocket expenditure in Australian healthcare
Introduction
2.1
Health expenditure occurs when money is spent on health goods and
services. It occurs at different levels of government, as well as by
non-government entities such as private health insurers and individuals.[1]
2.2
This chapter discusses the following terms of reference:
(a) the current and future trends in
out-of-pocket expenditure by Australian health consumers; and
(e) key areas of expenditure,
including pharmaceuticals, primary care visits, medical devices or supplies,
and dental care.
2.3
Evidence provided to the committee discussed total out-of-pocket
expenditure in healthcare as well as expenditure in particular areas of health
care. This chapter will first discuss the evidence received related to overall
expenditure in healthcare and then the evidence related to expenditure in
different areas of healthcare.
What is out-of-pocket expenditure?
2.4
Individuals incur out-of-pocket expenditure when they meet the full cost
of a health good or service as well as when they share the cost of goods and
services with third-party payers such as governments or private health
insurance funds.[2]
2.5
The following list of examples of out-of-pocket healthcare costs was
provided by the National Rural Health Alliance in their submission:
-
the 'gap' between the fee for a doctor’s consultation and the
amount rebated by Medicare;
-
the 'gap' between the fee for a dental or allied health
consultation and the amount rebated by a private health insurance fund (for
someone with private health insurance);
-
the total cost of a dental or allied health consultation (for
someone without private health insurance);
-
the cost of prescription medicines to the consumer (after the
subsidy for PBS-listed medicines has been applied);
-
the total cost of 'over the counter' medicines, such as aspirin
and cough syrup;
-
the total cost of natural and complementary medicines, such as
vitamins and nutritional supplements; and
-
the net cost of medical devices (after any subsidies and rebates
are applied), such as prostheses, dental devices, syringes and contraceptives.[3]
2.6
The Department of Health noted private health insurance premiums as
another out-of-pocket cost incurred by individuals.[4]
Current out-of-pocket healthcare expenditure
2.7
The Australian Institute of Health and Welfare (AIHW) collects and
analyses data about individual out-of-pocket expenditure in healthcare. When
providing evidence to the committee, a large number of submitters and witnesses
referenced AIHW data.
2.8
Total health expenditure in Australia in 2011–2012 was estimated to be
$140.2 billion. Governments funded 69.7 per cent of total health expenditure
which included 42.4 per cent from the Commonwealth Government and 27.3 per cent
from state and territory governments. Non-government sources funded 30.3 per
cent of the estimated $140.2 billion spent in 2011–12.
2.9
Funding by individuals accounted for 57.2 per cent of the estimated
non-government funding of health goods and services in 2011–12. The
contribution by individuals accounted for 17.3 per cent of the total health
expenditure funding (government and non-government). This includes:
-
where individuals meet the full cost of goods and services—for
example, medications that are not subsidised by the PBS, health services not subject
to a Medicare rebate;
-
where individuals share the cost of health goods and services
with third party payers—for example, Medicare, private health insurance funds.[5]
2.10
According to the Department of Health:
Of the $140.2 billion spent on health care in Australia in
2011–12 ($6 230 per capita), a total of $24.3 billion was from out-of-pocket
payments by individuals (adjusted for the Net Medical Expenses Tax Offset—NMETO).
This is equivalent to $1 078 per capita ($1 102 before the NMETO). A further
$11.2 billion ($496 per capita) was paid by private health insurers, and so
indirectly by individuals.[6]
2.11
Data from the AIHW indicates that total individual out-of-pocket
expenditure in 2011–12 ($24.3 billion) was more than double the $11 billion
spent a decade earlier in 2001–02. With respect to the proportion of total
health expenditure funded by individual out-of-pocket payments, in 2011–12 this
was 17.3 per cent, relatively unchanged from 17.5 per cent in 2001–02 (see
Table 2.1 below).
2.12
Further to this, the AIHW advised that the contribution of
non-government funders of health to total expenditure reduced from 32.8 per
cent in 2001–02 to 30.3 per cent in 2011–12. Government expenditure increased
from 67.2 per cent in to 69.7 per cent in 2011–12.[7]
2.13
The committee notes that this data indicates that individual expenditure
($11 billion) accounted for 53 per cent of health expenditure from all
non-government sources ($20.7 billion) in 2001–02. In 2011–12, individual
expenditure ($24.3 billion) accounted for 57 per cent of health expenditure
from all non-government sources ($42.4 billion).
Table 2.1: Total individual health expenditure and
proportion of health expenditure from all sources of funds
|
Year
|
Amount ($m)
|
Proportion (%)
|
Year
|
Amount ($m)
|
Proportion (%)
|
|
2001–02
|
11 050
|
17.5
|
2007–08
|
17 416
|
16.8
|
|
2002–03
|
11 514
|
16.7
|
2008–09
|
19 451
|
17.1
|
|
2003–04
|
12 828
|
17.5
|
2009–10
|
21 246
|
17.5
|
|
2004–05
|
14 131
|
17.4
|
2010–11
|
23 834
|
18.3
|
|
2005–06
|
15 108
|
17.4
|
2011–12
|
24 254
|
17.3
|
|
2006–07
|
16 553
|
17.4
|
|
|
|
Source: Australian Institute of Health and Welfare 2013. Health
expenditure Australia 2011–12. Health and welfare expenditure series no.
50. Cat. no. HWE 59. Canberra: AIHW, p. 42.
2.14
The Department of Health also observed that the share of health expenses
met by individual out-of-pocket payments remained relatively stable between
2001–02 and 2011–12.
... while the share of health expenses met by out-of-pocket
payments clearly increased in the five years after 1986–87, from 13.6 per cent
in 1986-87 to 16.5 per cent in 1991-92, and in the five years after 1995-96, it
has remained relatively stable over the past decade.[8]
2.15
Further to this, the Department submitted:
Overall health expenditure per capita and out-of-pocket
expenditure on health per capita continue to grow at a faster rate than the
broader economy, average incomes and overall household expenditure. Measured in
current prices, overall health expenditure per capita and out-of-pocket
expenditure on health per capita have grown by 91.4 per cent and 89.0 per cent
respectively over the decade to 2011–12. That is, out-of-pocket expenditure on
health per capita is currently growing at the same rate as total expenditure on
health. Over the same period, GDP per capita grew by 69.7 per cent, average
weekly earnings grew by 54.0 per cent and total household expenditure grew by
an estimated 65.6 per cent in nominal terms.[9]
Figure 2.1: Share of health expenditure funded by
out-of-pocket payments,
1986–87 to 2011–12.

Source: Department of Health, Submission 101, p.
7. (Departmental analysis of AIHW health expenditure data)
2.16
Several submitters and witnesses commented on the proportion of health
expenditure contributed by individuals[10],
noting that there are a number of issues that need to be considered when
analysing the proportion of individual health expenditure.
2.17
The committee heard evidence from the Consumers Health Forum of
Australia (CHF) that 17.3 per cent out-of-pocket expenditure is contributed by
individuals. It was explained that this percentage comprises areas of
healthcare where there are no (or limited) government subsidies including: some
pharmaceutical spending, dental services, and aids and appliances. This
suggests that there are some areas of health care where individual consumers
are paying a large proportion—in some cases the entirety—of the cost.[11]
Growth in individual expenditure
2.18 Evidence to the committee stated that individual expenditure has risen
in real terms whilst individual expenditure as a proportion of overall health
expenditure has remained relatively stable.
2.19
According to the AIHW:
People are definitely paying more—that is, taking into
account inflation and having adjusted for the medical expenses rebate—out of
their pockets than they were in the past. It has been increasing as per person,
so it is not just about population growth. Per person, we are also spending
more. It has not been increasing as a proportion of total expenditure. So
whilst growth has been strong, growth across the health sector has been strong.[12]
2.20
Dr Stephen Duckett, Director, Health Program, Grattan Institute observed
that out-of-pocket costs are increasing because total health expenditure is
increasing and there has been a real increase in out-of-pocket costs over the
last five years.[13]
In particular, since 2007, the average out-of-pocket payments for Medicare
services have risen by a quarter in real terms. Out-of-pocket costs have
increased in all but three categories[14]
(see Figure 2.2).
Figure 2.2: Real increase in out-of-pocket costs, 2007-2013
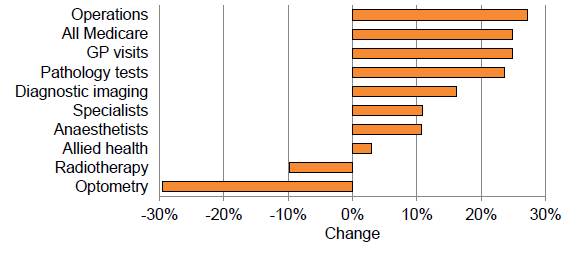 Source:
Grattan Institute, Submission 79,
p. 4.
Source:
Grattan Institute, Submission 79,
p. 4.
2.21
Submitters observed that individuals are carrying an increasing burden
of out-of-pocket costs for health care in a variety of areas, including GP
visits, medications, pathology and imaging, dental services, hospital services.[15]
2.22
Data from the AIHW indicates that per person health expenditure by
individuals (that is averaged over the whole population) grew at an average of
5.2 per cent per year from 2001–02 to 2011–12. The areas of expenditure with
the highest per person growth rates in 2011–12 included benefit-paid
pharmaceuticals (4.2 per cent) and dental services (2.2 per cent). The areas
with negative growth included community and public health services (–18.8 per
cent), patient transport services (–7.4 per cent) and hospital services (–5.9 per cent).[16]
Household expenditure on out-of-pocket health costs
2.23
Another measure of health expenditure analysed by the AIHW is the
household final consumption expenditure which measures household expenditure as
opposed to income. There has been an increase from approximately 2.7 per cent
to 3.2 per cent over the last 10 years in the proportion of household
expenditure being spent on out-of-pocket healthcare costs.
2.24
The AIHW advised that this data is not currently compared against proportion
of household income.[17]
2.25
The Department of Health submitted details from the 2009–10 ABS
Household Expenditure Survey which showed that weekly expenditure on 'medical
care and health expenses' (including the cost of private health insurance) was
$65.60 for the average Australian household, making up 5.3 per cent of total
household expenditure. The Department observed that components of household
expenditure have grown at different rates over time, sometimes decreasing in
real terms. The fastest growing direct health costs for households are for the
category that includes non-prescription medicines, pharmaceutical products and
therapeutic appliances.[18]
International comparisons
2.26
Several submitters and witnesses discussed Australia's out-of-pocket
costs in comparison to a range of international jurisdictions. It was noted
that out-of-pocket expenditure for Australian health consumers is high by
international standards.[19]
2.27
Data from the AIHW indicates that in 2000, Australia's average
out-of-pocket expenditure per person using OECD criteria ($583) was $35 above
the weighted OECD average ($548). In 2010, Australia's average out-of-pocket
expenditure per person ($1 075) was $94 above the weighted OECD average ($981).
2.28
The AIHW also noted that out-of-pocket expenditure fell as a proportion
of total health expenditure, accounting for 19.8 per cent of total health
expenditure in 2000 and 19.3 per cent in 2010[20].
However, out-of-pocket expenditure increased as a percentage of total household
final consumption expenditure in Australia, from 2.7 per cent in 2000 to 3.2
per cent in 2010. The OECD weighted averages against these measures were 16.3
per cent in 2000 and 13.9 per cent in 2010, and 2.7 in 2010 and 2.9 per cent in
2010 respectively.[21]
2.29
Several submitters and witnesses discussed Australia's out-of-pocket
costs in the context of comparisons against OECD data.
2.30
Professor Stephen Jan, The George Institute for Global Health, told the
committee that the level of out-of-pocket costs in Australia, when compared
with the OECD average, is third only to the US and Switzerland.
2.31
The committee inquired into the underlying reasons for this ranking and were
advised by Professor Jan:
In general terms, it is the level of co-payments that we pay
for Medicare reimbursed services and also the fact that we have a significant
number of medical expenses that are not covered by Medicare or through the
hospital system that people have to incur out of pocket. One example might be
home oxygen for people. The coverage for that varies for chronic obstructive pulmonary
disease, and we found that to be a significant burden for a particular patient
population. There are a number of allied healthcare services that often are not
covered under Medicare or through the hospital system that people have to pay
for out of pocket. Those are really the two areas. It is gap payments or
co-payments and also the services that are not covered.[22]
2.32
The Grattan Institute submitted that Australia is ranked in the middle
of the OECD for the proportion of health costs paid for with out-of-pocket
fees. It was also noted that the amount Australians pay as a proportion of
their household expenditure is relatively high (see Figure 2.3).
Figure 2.3: Out-of-pocket
medical spending as a share of final household consumption, 2011 (or nearest
year)
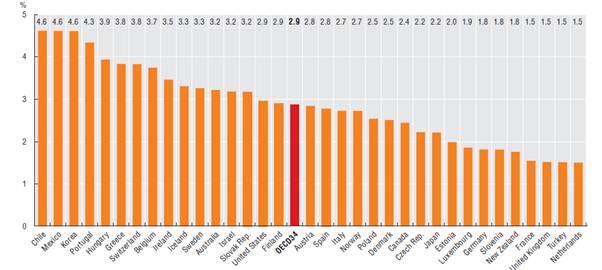
Source:
OECD, Health at a Glance 2013, OECD Indicators, p. 141.
2.33
The Grattan Institute also compared countries in terms of out-of-pocket
payments and GDP per capita. When comparing against this indicator with similar
countries, only Switzerland is ranked much higher than Australia.[23]
2.34
According to the Department of Health:
In 2011, Australia expended 9.1 per cent of its GDP on
health. This is lower than the average level of expenditure across the OECD, at
9.3 per cent. It is also lower than the median across the OECD, at 9.3 per
cent. Australia ranks 21st out of the 34 OECD countries on this measure. This
places Australia in the 2nd lowest quintile on this measure.[24]
2.35
The Royal Australian College of General Practitioners (RACGP) observed:
I would like to begin by saying that Australians already pay
high out-of-pocket costs, with the average Australian paying $1 075 annually on
health care. Total patient out-of-pocket expenses for primary health care have
significantly increased over the past 10 years, rising from $9.7 billion in
2001–02 to $17.1 billion in 2011–12—that represents a 76 per cent increase.
These costs are above the OECD average and are already delaying or preventing
1.8 million Australians from seeking the health care that they need—and that is
based on ABS data.[25]
2.36
The AIHW explained to the committee that individual out-of-pocket
expenditure is collected by drawing together approximately 80 data sources from
all levels of government as well as the private sector. The AIHW collects this
information in accordance with OECD requirements and standards and provides
this data to the OECD and the World Health Organisation annually. The AIHW
noted that there are many OECD countries that are not able to estimate
out-of-pocket expenditure.[26]
The AIHW added:
They [the OECD] try to pull together the expenditure
information and, by and large, they look at that at a high level and they try
to produce country rankings to give people a sense of where they sit in the
overall expenditure. As to whether we are fifth or 10th or 15th, it is a bit
hard to tell but we are probably not 30th and we are probably not first. They
take that information and look at health outcomes information. Obviously, the
OECD reports have a wide range of information—not just about expenditure but
also about all the key indicators of health. As Dr Duckett and others have
mentioned, we are known for a system that is relatively efficient. In terms of
the dollars spent for the health outcomes achieved, we do well.
... That is an international comparison. That judgement about
relative efficiency is comparing us to other nations that perhaps spend a
similar quantum of dollars but do not achieve the same health outcomes.[27]
2.37
Officials from the Department of Health cautioned against drawing
comparisons between Australia and other OECD countries:
A number of submissions have highlighted the absolute value
of out-of-pockets as evidence of an issue across the system. The trend over the
last couple of years for out-of-pockets as a percentage of total health
expenditure is down. It peaked at 19 per cent some years ago; it was 18.3 per
cent in 2010–11; and in 2011–12 it was 17.3 per cent. It is lower than the OECD
average, and Australia ranks 15 out of 34 of OECD countries for out-of-pockets
as a percentage of health expenditure. The absolute dollars in many ways are an
indication of the wealth of a society, rather than the appropriateness or
inappropriateness of the level of out-of-pockets being charged. The extent to
which out-of-pockets are discretionary is highlighted when an analysis of the
out-of-pocket data is undertaken. The largest and fastest-growing area is
non-prescription medicines, including complementary medicines. They are nearly
one third of the total out-of-pocket costs. Medical services are about 12 per
cent, and prescription pharmaceuticals are less than seven per cent of the
total.[28]
Key areas of expenditure
2.38
Australian consumers spend money on healthcare in a number of different
areas. In 2011–12, the AIHW estimates that individuals spent $24.8 billion[29]
in recurrent funding for health goods and services. Over one-third (39.2 per
cent) of this was for medications (mostly non benefit-paid pharmaceuticals). A
further 19.1 per cent was for dental services; 11.9 per cent for medical
services; 10.1 per cent for aids and appliances; and 7.8 per cent for other
health practitioner services (see Table 2.2).[30]
Table 2.2: Individuals' funding of recurrent health
expenditure, by area of expenditure—current prices—2011–12
|
Area of expenditure
|
Amount ($ million)
|
Per cent
|
|
Public hospital services
|
1 117
|
4.5
|
|
Private hospitals
|
1 334
|
5.4
|
|
Patient transport services
|
351
|
1.4
|
|
Medical services
|
2 955
|
11.9
|
|
Dental services
|
4 736
|
19.1
|
|
Other health practitioners
|
1 928
|
7.8
|
|
Community health and other
|
115
|
0.5
|
|
Public health
|
20
|
0.1
|
|
Benefit-paid pharmaceuticals
|
1 665
|
6.7
|
|
All other medications
|
8 067
|
32.5
|
|
Aids and appliances
|
2 503
|
10.1
|
|
Administration
|
—
|
—
|
|
Research
|
5
|
—
|
|
Total
|
24 795
|
100.0
|
- Individuals' expenditure has not been adjusted
down for the medical expenses tax rebates
- Public hospital services exclude certain services
undertaken in hospitals. Can include services provided off-site, such as
hospital in the home, dialysis or other services
- 'Other' refers to other recurrent health services
not elsewhere classified.
Note: Components
may not add to totals due to rounding
Source: Australian
Institute of Health and Welfare[31]
2.39
Although individual health expenditure as a proportion of health
expenditure from all sources has remained stable between 2001–02 and 2011–12, there
have been changes in expenditure in different areas of healthcare over the same
period (see Table 2.3).
Table 2.3: Average individual
recurrent health expenditure per person, constant prices, and annual growth
rates, by area of expenditure, 2001–02 to 2011–12
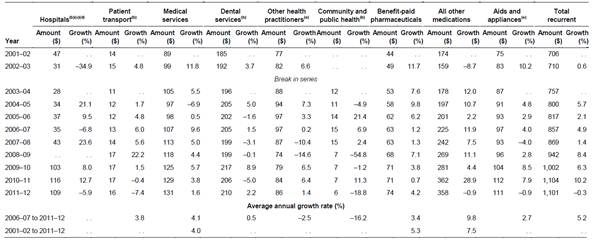
2.40
The Department of Health observed that there has been a considerable
change in the out-of-pocket costs associated with medications and with medical,
dental and other health practitioners over time. In particular:
The share of out-of-pocket costs spent on medicines and
pharmaceutical products doubled between 1986–87 and 2011–12 from 19.5 per cent
to 39.3 per cent; and the share of out-of-pocket costs spent on medical, dental
and other health practitioners fell from 64.1 per cent to 38.8 per cent.[32]
2.41
The range of goods and services captured as part of health expenditure
is broad. The Department of Health explained that out-of-pocket costs comprise a
broad range of components including an element of cosmetic surgery,
complementary medicines, complementary therapies and a range of vitamins and
supplements.[33]
2.42
Further to this, the Department explained the discretionary choices that
people are making in terms of their health expenditure. In 2007, Australians
spent $4 billion on complementary medicines and therapies. Whilst acknowledging
that detailed data is limited, departmental officials noted that expenditure in
this area has continued to grow strongly.[34]
2.43
The Department also advised that out-of-pocket costs for medical
services (broader than the MBS) are $2.9 billion and prescription pharmaceuticals
(broader than the PBS) are $1.7 billion. This equates to about 20 per cent of
the total out-of-pocket costs.[35]
2.44
Mr Gordon Gregory, Executive Director, National Rural Health Alliance
described an alternate model for consideration of the different areas of health
expenditure:
We ask you to conceive of three concentric circles: the
centre one has the out-of-pocket costs for seeing a GP; next, what might be
called the rest of the standard out-of-pocket health care costs; and, on the
outside, the actual total out-of-pocket health care costs for rural and remote
people, which includes the cost of transport to and from services. All three of
these are relevant, but evidence about the middle circle is not available by
remoteness and the importance of the outside circle—that is transport and
accommodation—is obvious but not easily quantified.[36]
2.45
The next section summarises the evidence received by the committee in
the following areas of health expenditure:
-
pharmaceuticals and other medications, such as over-the-counter
medications that do not require a prescription;
-
medical services;
-
specialist services;
-
medical devices and supplies;
-
dental care;
-
health related travel costs.
Medical services
2.46
In 2011–12 Australians spent $2.955 billion on medical services,
comprising 11.9 per cent of total healthcare expenditure.[37]
Medical services in this category include GP visits, pathology and imaging
services.
2.47
The committee heard evidence that in 2012–13, 81.1 per cent of GP
consultations were bulk billed and 88.7 per cent of private in-hospital medical
services were charged at the private health insurance benefit (i.e. no
out-of-pocket costs).
2.48
The committee notes that there is some variability across regions in
terms of GP bulk billing rates.
2.49
The Australian Medical Association (AMA) submitted:
In the decade to 2012–13, the percentage of medical services
attracting out of pocket costs has either stayed the same or declined. The
medical profession has effectively absorbed the relative reductions in
Government and PHI contributions to the cost of medical services. However,
patients who do have out of pocket costs for medical services are paying more
today than they were a decade ago. These services partly offset the services
provided at no cost.[38]
2.50
Furthermore, the AMA observed that contrary to common perceptions,
medical services do not make up the majority of out-of-pocket costs for
individuals, accounting for 11.9 per cent of the total of individuals'
out-of-pocket costs.[39]
2.51
The committee was reminded that the figure of 81 per cent of bulk-billed
GP consultations relates to each individual item number that is bulk-billed.
The provision of this information at item number level does not allow for
analysis of the number of individuals that are bulk-billed, the frequency of
bulk-billing and the location.[40]
2.52
Evidence received from Catholic Health Australia indicated that the
average out-of-pocket cost for a GP visit is now $28, which represents a 50 per
cent increase in five years.[41]
2.53
The AMA advised that the average out-of-pocket cost for a GP visit was
$28.58 in 2012–13 compared to $12.46 in 2002–03, reflecting an 11.8 per cent
growth per annum.[42]
2.54
COTA Australia provided evidence about the average out-of-pocket cost
for a visit to non-bulk-billing doctors, noting that the average was $46.50 in
2012.[43]
2.55
During the 2014–15 Budget Estimates, the Department of Health advised
that in 2012–13, total expenditure on out-of-hospital pathology was $2.14
billion, 98.5 per cent paid by government and 1.5 per cent paid by patients.[44]
2.56
The Australian Diagnostic Imaging Association submitted that out-of-pocket
costs for non-bulk billed services are growing at rates significantly higher
than inflation, and averaged $88 in 2012–13 ($158 for MRI), with patients
contributing $475 million to their cost of their care. The growth in gaps was
9.8 per cent in , 7.0 per cent in 2011–12 and 4.7 per cent in 2012–13.[45]
Pharmaceuticals and other
medications
2.57
Data from the AIHW indicates that Australians spent approximately $9.7 billion
on medications in 2011–12 which is approximately 39 per cent of total
expenditure. The table below shows the breakdown between benefit-paid
pharmaceuticals and all other medications.
Table 2.4: Amount of out-of-pocket costs paid by Australian
consumers on benefit-paid pharmaceuticals and all other medications.
|
Area of expenditure
|
Amount ($ million)
|
Per cent (of total expenditure)
|
|
Benefit-paid pharmaceuticals
|
1 665
|
6.7
|
|
All other medications
|
8 067
|
32.5
|
Source: Australian
Institute of Health and Welfare
2.58
The Department of Health submitted that the share of out-of-pocket costs
on PBS medication has remained stable over the period from 2001–02 to , reporting a small rise from 6.3 per cent to 6.7 per cent of total out-of-pocket
costs. In contrast, the out-of-pocket costs incurred from purchasing non-PBS
subsidised medications have increased over the same period:
In 2002–03, non-PBS subsidised medications (most of which are
non-prescribed medications) accounted for 22.3 per cent of total out-of-pocket
costs. In 2011–12 they accounted for 32.5 per cent of all out-of-pocket costs.
Some of this increase is due to an increase in the number of PBS listed
medications whose cost is fully covered by the level of the non-concessional
co-payment, as the cost of these medications is shown in the non-PBS subsidised
category. However, most of the increase is due to an increased use of
non-prescribed medications. The Department estimates that the share of
out-of-pocket costs associated with non-prescribed medications increased from
17.2 per cent in 2002–03 to 23.5 per cent in 2011–12.[46]
Benefit-paid pharmaceuticals
2.59
Evidence from the Pharmacy Guild of Australia noted that the cost of
pharmaceuticals has increased since 2000 on average by 2.1 per cent, compared
with the 2.8 per cent increase in the Consumer Price Index. The concessional
co-payment for pharmaceuticals has increased from $3.30 in 2000 to $6.00 in
2014 which equates to 4.4 per cent average annual change. The general
co-payment has increased from $20.60 in 2000 to $36.90 in 2014 which is 4.5 per
cent average annual change.[47]
2.60
Further to this, the committee was advised that approximately 72 per
cent of prescriptions for general patients have a dispensed price less than the
$36.90 general payment.[48]
Other medications
2.61
As evidenced in Table 2.5 above, the majority of medication expenditure
relates to the 'all other medications' category. The AIHW advised that 63 per
cent of the other medications category relates to over-the counter medications.
The remaining components in this category are approximately 20 per cent for
under co-payment prescriptions and approximately 10 per cent for private prescriptions.[49]
2.62
The committee heard evidence that information about the sale of products
in the other medications category is collated from pharmacies, supermarkets and
the health food sector using broad categories (see Table 2.5 and Table 2.6[50]).
This data is not broken down to a product level so the quantum of particular
products in each industry category is unknown.[51]
2.63
The committee notes that it is unclear what proportion of expenditure is
attributed to complementary medicines. As outlined earlier, the Department advised
results from a market survey which found that Australians are spending $4
billion annually on complementary medicines and natural therapies.[52]
This data provides the total amount spent nationally but does not give any
indication about where this spending occurs and by whom.
2.64
Data from the ABS related to household weekly expenditure may provide
some additional detail on this matter. 2009–10 figures indicate that a weekly
household spend is $5.83 on prescription medicines, $2.12 on first aid supplies
and therapeutic appliances, 84 cents on non-prescribed painkillers, 16 cents on
sunscreen and $8.91 on other non-prescribed items.
2.65
The committee notes that expenditure in the 'other medications' category
does not contribute to the PBS safety net threshold amount. Safety nets are
discussed in greater detail in chapter three of this report.
Table 2.5: Categories that
AIHW uses to compile expenditure on over-the-counter pharmaceuticals purchased
from supermarkets
|
Sunscreen and after sun care
|
Cotton e.g. cotton wool, cotton
balls, cotton buds/tips
|
Throat care
|
|
Adult incontinence
|
Dietary supplements
|
Wound care
|
|
Allergy care
|
Laxatives
|
Nappy rash treatment
|
|
Analgesics
|
Anti-diarrhoeal
|
Footcare
|
|
Antacids
|
Fluid replacement
|
Anti-dandruff hair care
|
|
Antiseptics
|
Rheumatic rubs
|
Toothbrushes and toothpaste
|
|
Cold relief
|
Sinus remedy
|
Medical non-durables (i.e. family
planning)
|
|
Cold sore care
|
Smoking control
|
Facial treatment and cleansers
|
Source: Retail World Annual
Reports[53]
Table 2.6: Categories that AZTEC provides to compile
expenditure on over-the counter pharmaceuticals purchased from pharmacies
|
Total allergy
|
Total first aid
and sports medicine
|
Total smoking cessation
|
|
Total analgesics
|
Total footcare
|
Total sports nutrition
|
|
Total cough and cold
|
Total home self care
|
Total weight management
|
|
Total digestive care
|
Total natural health
|
|
|
Total eye care
|
Total sexual health
|
|
Source: AZTEC[54]
Medical devices and supplies, aids
and appliances
2.66
Evidence provided to the inquiry indicated that individuals contribute a
high proportion of expenditure for medical devices and supplies, aids and
appliances. High out-of-pocket costs in this area is partly due to the high
cost of these items and the low level of contribution from other sources (if
any at all).[55]
2.67 Several individuals submitted details about out-of-pocket costs
associated with purchasing necessary medical supplies such as catheters.
Examples of the annual costs of purchasing catheters provided were in excess of
$2 000 up to over $7 000.[56]
Dental care
2.68 Costs associated with dental care are a significant area of health
expenditure. Dental expenditure in Australia is made up of government and
non-government funding. In 2011–12, total expenditure paid on dental health was
estimated at $8.336 billion comprising the following:
-
federal and state governments paid $2.3 billion:
-
state and territory governments paid $718 million through public
sector service provision;
-
federal government paid $1.59 billion through private providers;
-
non-government contributed $6.03 billion;
-
health funds contributed $1.26 billion;
-
individuals contributed $4.74 billion; and
-
$34 million came from other sources.[57]
2.69 The committee notes that these figures demonstrate that individuals make
the second highest contribution towards the cost of dental care.
Figure 2.4: Dental expenditure in Australia 2011–12
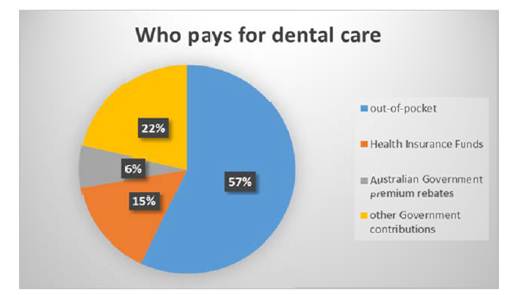
Source: Australian Dental Association, Submission 57,
p. 1.
2.70 The committee heard evidence from the Australian Dental Association (ADA)
that Australians contributed $4.7 billion towards their dental care in 2011–12.
Much of this amount relates to private health insurance premiums and
out-of-pocket costs created by gap fees between fees and the rebate.[58]
2.71 The ADA advised that treatment charged by dentists have not risen a
great deal since 2006. The ADA explained that although the costs charged by
dentists and private health insurance rebates have remained relatively stable,
private health insurance premiums have increased. Increased premiums contribute
to the increased out-of-pocket costs for individuals.
2.72 The Australian Healthcare & Hospitals Association highlighted that
out-of-pocket costs for dental services were the same as the costs for medical
services, public hospital and private hospital care combined.[59]
Health related and other travel
costs
2.73 Health related travel costs are not accounted for when health
expenditure data is collected. The Department of Health confirmed:
As soon as they are subsidised they are captured but—you are
right—a huge proportion will not be subsidised and will not be captured, just
as those sorts of costs are not captured for a whole range of other things.[60]
2.74 Evidence provided to the committee indicated that health related travel
costs contribute significantly to individuals' out-of-pocket costs. These costs
include direct travel costs (flights, train or bus, fuel), accommodation as
well as costs associated with loss of income due to inability to work and the
cost of care arrangements for other family members.[61]
Submitters emphasised that travel costs may act as a barrier to accessing
required health services.[62]
2.75 Parkinson's Victoria explained that transport assistance schemes are
means tested and often limited to concession card holders. This places a
significant cost burden for individuals without healthcare cards who need to
travel to health services. Even when financial assistance is available,
benefits are only payable if the journey exceeds 100 kilometres.[63]
2.76 The cost of travelling to access healthcare is particularly significant
for regional and remote communities. Mr Gregory explained to the committee:
The standard measurement of out-of-pocket health care cost
does not include the cost of transport to services, which due to the distances
to be covered and the lack of public transport are much higher for rural people
for every occasion of service. These transport costs—including accommodation,
income forgone and logistical complexities—often dwarf standard out-of-pocket
costs for families in more remote areas. The jurisdictional patient travel and
accommodation schemes are poorly understood, poorly promoted and not sufficient
to cover the real costs involved in travelling to and staying in major cities.[64]
2.77 Further to this, Mr Gregory advised that 'there is almost nothing that
pops up on our radar here at the Rural Health Alliance more regularly, than
patients' travel and accommodation—it is still a major issue'.[65]
2.78 Dr Christine Walker, Executive Officer, Chronic Illness Alliance
provided evidence about the impact of the high cost of hospital parking:
We had a dreadful example—somebody whose child was a
transplant patient who eventually died at one of Sydney's major hospitals. They
did not think about the cost of parking. After the child had died, they worked
it out and they reckoned they had spent something like $6 000 on parking their
car at the hospital.[66]
Specialist services
2.79 Professor Jan advised that when looking at the level of out-of-pocket
costs in the health system, the majority of the costs incurred relate to
specialist services. In contrast to the approximately 80 per cent of bulk-billed
GP services, only a very low percentage of specialist services are bulk billed.[67]
2.80 Evidence provided to the inquiry suggested that a large volume of
expenses incurred by individuals using the health system relate to services
provided by specialists.[68]
2.81 The Australian Healthcare & Hospitals Association provided evidence
that in the 2012 December quarter, medical specialist fees for in-hospital
services totalled $254 million, with Medicare covering $67 million and private
health insurance contributing $47 million. Patients incurred out-of-pocket
costs of $140 million.[69]
2.82 Evidence provided by the Australian Society of Anaesthetists (ASA) suggests
out-of-pocket expenses for anaesthesia services is significantly less that than
of other specialists.[70]
2.83 Further to this, the ASA noted:
...approximately 3.5 million to 3.7 million anaesthetics are
given in Australia each year, and more than 90 per cent of all anaesthesia
services are provided at no out-of-pocket cost to the patient. In the private
sector, more than 85 per cent are provided at no out-of-pocket cost to the
patient. The primary reason for any out-of-pocket expenses has essentially been
the lack of adequate indexation over the last 30 years and also, in anaesthesia
specifically, the level of rebates have been significantly lower when compared
to other craft groups. For example, anaesthesia rebates represent about 40 to
45 per cent of the AMA recommended fee, whereas for other surgical specialties
that is up to 60 to 65 per cent and even up to 70 per cent, varying on
different specialties.[71]
2.84 The ASA explained that out-of-pocket costs for anaesthesia relate to
private services. There are approximately 2.1 million anaesthesia services
provided in the private sector annually and approximately one in six of these
patients will incur out-of-pocket costs. The ASA advised the committee that
‘over the past 30 years the issue of out-of-pocket expenses for anaesthesia and
for health services in general have arisen because of the failure of
indexation’.[72]
2.85 The committee notes that out-of-pocket costs incurred for private
anaesthesia services are in addition to private health insurance premiums.
Private health insurance
2.86 Individual expenditure associated with private health insurance is a
combination of insurance premiums and out-of-pocket costs to cover treatment
costs not paid by Medicare or the private health insurer. The committee heard
evidence that gap payments may vary significantly across private health
insurers.
2.87 The Department of Health submitted that one third of household
expenditure in 2009–10 on medical care and health expenses was associated with
the cost of private health insurance.[73]
2.88 According to data provided by the Private Health Insurance
Administration Council (PHIAC) in The Operations of Private Health Insurers
Annual Report 2012-13, during 2012–13 the funding of privately insured
services totalled $22.402 billion and comprised the following components:
-
benefits provided by private health insurance of $15.303 billion
(68.3 per cent);
-
benefits provided by Medicare of $2.376 billion (10.6 per cent);
and
-
payments by patients of $4.722 billion (21.1 per cent).[74]
2.89 The Australian Healthcare Reform Alliance submitted:
PHIAC quarterly statistics for June 2013 show that the
average co-payment for one episode of hospital treatment was $307 and for
non-hospital services it was $47. Due to their higher average level of need,
older people incur higher out-of-pocket payments than younger people using
private health services.[75]
2.90 Bupa Australia observed two recent issues that have affected the out-of-pocket
costs for individuals with private health insurance: (1) changes to the
government private health insurance rebate and (2) contract arrangements
between private health insurers and hospitals.[76]
2.91 Issues relating to private health insurance are discussed in more detail
in chapter five of this report.
Other areas of expenditure
2.92 The committee received evidence outlining other areas of out-of-pocket expenditure.
The Australian Wound Management Association referred to a study undertaken in
2012 that reported a median of $142 a month for dressing products over an
average duration of 22 weeks with a total expense as high as $10 400.[77]
2.93 Optometrists Association Australia submitted that prescription glasses
and contact lenses do not qualify for a Medicare rebate, although a portion of
the cost is covered under some private health insurance policies. This means
that the out-of-pocket costs can be a barrier to accessing essential primary
eye care, particularly those on low incomes and without private health insurance.[78]
Committee view
2.94 The Australian community incurs out-of-pocket costs in healthcare in a
number of different areas. Individual expenditure as a proportion of overall
expenditure on healthcare has remained relatively stable since 2001–02 although
there have been changes in expenditure in different areas of the health system.
2.95 The committee notes evidence from several submitters and witnesses that
individual expenditure has risen in real terms while individual expenditure as
a proportion of overall health expenditure has remained relatively stable.
2.96 Evidence received about the impact of out-of-pocket expenditure in some
areas of health is subject to debate. The committee notes that analysing
Australia's healthcare system and out-of-pocket expenditure against international
comparisons is useful but that these comparisons need to be made with caution
and in context.
2.97 The committee notes the importance of developing and maintaining
comprehensive and robust national data about different areas of the health
system. This would ensure there is a solid evidence base to assist policy
development and ongoing evaluation and analysis, and would reduce the
likelihood of unintended consequences arising once policies are implemented.
Navigation: Previous Page | Contents | Next Page