As the gateway to the medical profession, medical schools have a role in addressing a range of issues in Australian health policy, including persistent geographical inequalities in access, and shortages in specialisations such as psychiatry.
Recent policy, including a limited redistribution of university medical places in favour of regional universities, has focused on redistributing existing resources to address chronic geographical shortages. However, on 5 May 2022, the Group of Eight (Go8) universities attracted attention with the release of a paper arguing that 1,000 additional medical places are needed to secure the pipeline of medical professionals.
This FlagPost explains Australian Government funding for university medical places, and some of the challenges associated with increasing medical student numbers.
Australian university medical courses and enrolments
Currently, 21 Australian universities operate primary medical programs, which provide a pathway to registration as a medical practitioner. Such programs must be assessed and accredited by the Australian Medical Council (AMC).
In 2021 (the latest year for which data is available) a total of 18,157 students were enrolled in these programs, including 15,310 (84.3%) domestic students and 2,847 (15.7%) international students. Total enrolments have increased slightly over the last decade, up 7.6% from 16,868 in 2012 (Figure 1).
Figure 1 Domestic and international medical student enrolments, Australia, 2012–2021
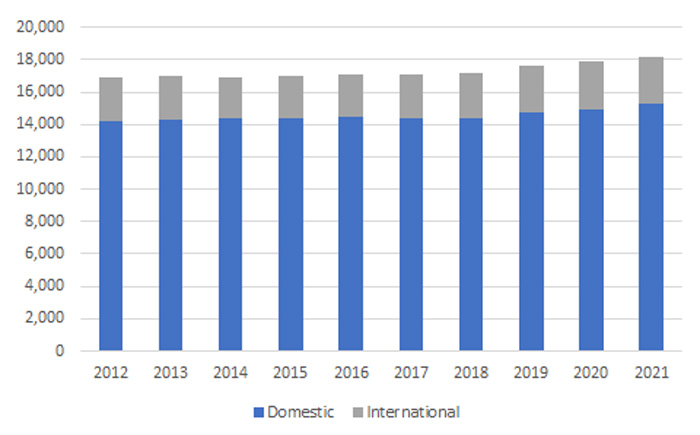
Source: Medical Deans Australia and New Zealand, Student Statistics, (Sydney: extracted 12 May 2022).
Note: international student numbers include only those enrolled in onshore programs. Totals differ slightly from those in the Department of Education, Skills and Employment’s higher education statistics collection.
Caps on enrolment numbers
The Australian Government does not impose a cap on the total number of medical students enrolled by universities in Australia. However, higher education funding arrangements do provide significant control over enrolment numbers.
Most domestic students studying medicine are entitled to a Commonwealth supported place (CSP), which provides reduced course fees, subsidised by the Australian Government through the Commonwealth Grant Scheme.
In 2022, a medical student with a CSP is liable to pay a contribution of $11,401, while the Australian Government contribution is $27,243, resulting in a total payment to the university of $38,644 per full-time student (slightly different amounts apply for students who commenced prior to 2021). An additional medical student loading of $1,465 is provided to the university for each place, to support the high cost of providing medical education. All 3 of these amounts usually increase each year of a student’s degree due to indexation.
Unlike other higher education courses offered by universities, medical CSPs are tightly controlled. The Minister allocates a set number of medical CSPs to each accredited provider for each calendar year. These allocations, and any associated conditions, are set out in providers’ funding agreements.
Courses that have CSPs allocated in this way (currently only medicine) are referred to as ‘designated higher education courses’ in the Higher Education Support Act 2003 (HESA) (section 30-12 and paragraph 30-10(1)(a)).
The Australian Government ensures domestic students enrolling in medical courses are entitled to a CSP in two ways:
Full fee-paying places
Students who enrol without a CSP, including international students and some domestic students, pay full fees, which are set by the university.
Although generally entitled to a CSP, domestic students studying medicine may be charged full fees:
- If they enrol at a ‘Table B’ (private) university. These universities are not subject to the requirement to offer undergraduate students CSPs (HESA, sections 16-20 and 36-30). Bond University is the only such university with a medical program.
- If they enrol at postgraduate level at a ‘Table A’ (public) university that does not have an allocation of medical CSPs (and the attendant conditions in its funding agreement). The Macquarie University medical program is based on this model.
How medical places are distributed to universities
Proposals for new or expanded medical programs where the university is seeking access to Australian Government higher education funding, such as CSPs or student loans, are considered by the Minister for Education, in consultation with the minister with responsibility for medical schools policy in the Health Portfolio, using an Assessment Framework.
Under this Framework, the total number of medical CSPs would be increased if the Department of Health triennial assessment of national medical workforce data indicates a need for additional medical places. Places may also be redistributed to meet an identified need.
The impact of additional medical places
Although the Australian Government could choose to fund additional medical CSPs, more university places do not necessarily equate to more doctors in the workforce.
One of the main reasons for controlling medical student numbers is the additional training that must be undertaken by medical graduates (p. 46) in order to gain general and specialist registration with the Australian Medical Board. Consisting of postgraduate year 1 (PGY1 or internship) and postgraduate year 2 (PGY2 or residency) prevocational training, and then, potentially, medical specialty training via specialist colleges, places at each stage of this additional training are highly competitive. States and territories maintain their own priorities and numbers for internship intakes after students graduate—see as examples information from the New South Wales, Queensland, and Northern Territory governments. A 2006 Council of Australian Governments agreement saw states and territories guarantee internship places to students graduating from a CSP in their jurisdiction.
The Royal Australasian College of Physicians supports the Go8 proposal for additional medical places, but continues to highlight that this will be insufficient to address workforce issues. The Australian Medical Association (AMA), while welcoming the Go8’s contribution to the debate concerning medical workforce, considers the proposal to be premature, arguing that ‘Australia can deliver much better patient access to medical services right now by looking more closely at opportunities to bolster prevocational and specialist training places around the country’ rather than diverting funding to additional university places.
The Australian Medical Students’ Association opposes additional CSPs, arguing that more investment in workforce planning via the National Medical Workforce Strategy 2021–2031 is needed, and that without additional internship places and specialty training positions, additional CSPs would ‘detrimentally exacerbate the bottlenecks we have in training doctors in this country’.